1. A patient diagnosed with focal tuberculosis of the upper lobe of the right lung had been taking isoniazid as a part of combination therapy. After some time, the patient reported of muscle weakness, decreased skin sensitivity, blurred vision, impaired motor coordination. Which vitamin preparation should be used to address these phenomena?
2. A 60-year-old male patient has a 9-year history of diabetes and takes insulin Semilente for the correction of hyperglycemia.10 days ago he began taking anaprilin for hypertension. One hour after administration of the antihypertensive drug the patient developed hypoglycemic coma. What is the mechanism of hypoglycemia
in case of anaprilin use?
3. Pterin derivatives (aminopterin and methotrexate) are the inhibitors of di- hydrofolate reductase, so that they inhibit the regeneration of tetrahydrofolic acid from dihydrofolate. These drugs inhibit the intermolecular tranfer of monocarbon groups, thus suppressing the synthesis of the following polymer:
4. A child with suspected tuberculosis was given Mantoux test. After 24 hours the site of the allergen injection got swollen, hyperemic and painful. What are the main components that determine such response of the body?
Explanation
Mantoux test is a type IV Hypersensitivity reaction (HSR), which involves macrophages,T-lymphocytes and lymphokines(cytokines). Mononuclear cells (lymphocytes,monocytes,macrophages).
Remember,it is antibody independent (i.e does not involve antibodies).
B-lymphocytesPlasma cellsIg(Antibodies)------- none is involved in Type IV HSR.
5. Hemoglobin catabolism results in release of iron which is transported to the bone marrow by a certain transfer protein and used again for the synthesis of hemoglobin. Specify this transfer protein:
6. A 12-year-old boy has been hospitalized for suspected food poisoning. The fecal samples were inoculated on the Endo agar, which resulted in growth of a large number of colorless colonies. What microorganism is most likely to be EXCLUDED from the list of possible causative agents of the disease?
7. A 23-year-old patient has been admitted to a hospital with a craniocerebral injury. The patient is in a grave condition. Respiration is characterized by prolonged convulsive inspiration followed by a short expiration. What kind of respiration is it typical for?
8. It has been experimentally proven that the excitation of the motor neurons of flexor muscles is accompanied by the inhibition of the motor neurons of extensor muscles. What type of inhibition underlies this phenomenon?
9. A 3-year-old boy with pronounced hemorrhagic syndrome doesn’t have anti-hemophilic globulin A (factor VIII) in the blood plasma. Hemostasis has been impaired at the following stage:
10. A patient got a gunshot wound of hip which damaged the sciatic nerve. Any impact on the affected limb causes severe, excruciating pain. What mechanism of pain is most likely in this case?
11. A 60-year-old patient with a long history of stenocardia takes coronarodilator agents. He has also been administered acetylsalicylic acid to reduce platelet aggregation. What is the mechanism of antiplatelet action of acetylsalicylic acid?
12. A patient with bronchial asthma has developed acute respiratory failure. What kind of respiratory failure occurs in this case?
13. On the fifth day after the acute blood loss a patient has been diagnosed with hypochromic anemia. What is the main mechanism of hypochromia development?
14. A patient with diabetes developed a diabetic coma due to the acid-base imbalance. Specify the kind of this imbalance:
15. A girl receives antibiotics of the penicillin group for acute bronchitis. On the third day of treatment she developed allergic dermatitis. Which drug should be administered?
16. A female patient has been diagnosed with cervical erosion, which is a precancerous pathology. What defense mechanism can prevent the development of a tumor?
17. Microscopy of the coronary artery of a dead 53-year-old patient revealed luminal occlusion due to a fibrous plaque with some lipids. The most likely form of atherosclerosis in this case is:
18. Autopsy of the patient revealed bone marrow hyperplasia of tubular and flat bones (pyoid marrow), splenomegaly (6 kg) and hepatomegaly (5 kg), enlargement of all lymph node groups. What disease are the identified changes typical for?
19. As a result of an injury a patient cannot extend his arm at the elbow. This may cause abnormal functioning of the following muscle:
20. A man sitting with his eyes closed, undergoes electroencephalography. What rhythm will be recorded on the EEG if there is an audible signal?
21. Electrophoretic study of a blood serum sample, taken from the patient with pneumonia, revealed an increase in one of the protein fractions. Specify this fraction:
22. Examination of an 18-year-old girl revealed the following features: hypoplasia of the ovaries, broad shoulders, narrow pelvis, shortening of the lower extremities, \"sphinx neck\". Mental development is normal. The girl was diagnosed with Turner’s syndrome. What kind of chromosome abnormality is it?
23. Hypertrichosis is the Y-linked character. The father has hypertrichosis, and the mother is healthy. In this family, the probability of having a child with hypertrichosis is:
24. A casualty has a fracture in the region of the inner surface of the left ankle. What is the most likely site for the fracture?
25. Some infectious diseases caused by bacteria are treated with sulfanilamides which block the synthesis of bacteria growth factor. What is the mechanism of their action?
26. A 42-year-old male patient with gout has an increased blood uric acid concentration. In order to reduce the level of uric acid the doctor administered him allopurinol. Allopurinol is the competitive inhibitor of the following enzyme:
27. A 40-year-old female patient diagnosed with acute pancreatitis has been delivered to the admission department of a regional hospital. What drug should be administered the patient in the first place?
28. A patient consulted a doctor about being unable to abduct his right arm after a past trauma. Examination revealed that the passive movements were not limited. The patient was found to have the atrophy of the deltoid muscle. What nerve is damaged?
29. After a trauma of the upper third of the anterior forearm a patient exhibits difficult pronation, weakening of palmar flexor muscles and impaired skin sensitivity of 1-3 fingers. Which nerve has been damaged?
30. A 38-year-old female patient complains of general weakness, cardiac pain, increased appetite, no menstruation. Objectively: the height is 166 cm, weight 108 kg, the patient has moon-shaped face, subcutaneous fat is deposited mainly in the upper body, torso and hips. There are also blood-red streaks. Ps- 62/min, AP- 160/105 mm Hg. Which of the following diseases is the described pattern of obesity most typical for?
Explanation

Cushing Syndrome: Etiology:
INCREASE Cortisol due to a variety of causes (Glucocorticoids):
Exogenous corticosteroids: result in decrease ACTH (MCC).
Primary adrenal adenoma, hyperplasia or carcinoma (Cushing’s Syndrome).
ACTH-secreting pituitary adenoma (Cushing Disease).
Findings: Hypertension, Weight Gain, Moon Facies, Truncal Obesity, Buffalo Hump, Skin Changes (thinning striae), Osteoporosis, Hyperglycemia (Insulin resistance), Amenorrhea, Immunosuppression.
31. A 60-year-old patient with a long history of atherosclerosis and a previous myocardial infarction developed an attack of retrosternal pain. 3 days later the patient was hospitalized and then died of progressive cardiovascular insufficiency. At autopsy a white fibrous depressed area about 3 cm in diameter with clear boundaries was found in the posterior wall of the left ventricle and interventricular septum. The dissector evaluated these changes as:
32. Measurements of the arterial pCO2 and pO2 during an attack of bronchial asthma revealed hypercapnia and hypoxemia respectively. What kind of hypoxia occurred in this case?
33. A female patient with bronchial asthma had taken prednisolone tablets (1 tablet 3 times a day) for 2 months. Due to a significant improvement of her condition the patient suddenly stopped taking it. What complication is likely to develop in this case?
34. A patient with suspected dysentery has been admitted to the infectious diseases hospital. Which basic method of laboratory diagnosis must be applied in the first place?
35. During a surgery with the use of hygronium the patient had an abrupt fall in blood pressure. Blood pressure can be normalized by the representatives of the following drug group:
36. A patient with respiratory failure has blood pH of 7,35. pCO2 test revealed hypercapnia. Urine pH test revealed an increase in the urine acidity. What form of acid-base imbalance is the case?
37. On examination a patient was found to have medial strabismus, the inward deviation of the eyeball and inability to abduct the eyeball outwards. What nerve is damaged?
38. A patient with a dislocated shoulder had been admitted to a hospital. With the purpose of skeletal muscle relaxation he was given an injection of relaxant dithylinum acting normally 5-7 minutes. However, the effect of dithylinum in this patient lasted up to 8 hours. What is the most likely cause of the prolonged effect of dithylinum in this patient?
39. As a result of an injury of the knee joint a patient shows a drawer sign, that is the anterior and posterior displacement of the tibia relative to the femur. What ligaments are damaged?
40. The neurosurgical department has admitted a 54-year-old male complaining of no sensitivity in the lower eyelid skin, lateral surface of nose, upper lip. On examination the physician revealed the inflammation of the second branch of the trigeminal nerve. This branch comes out of the skull through the following foramen:
41. Bacteriological examination of purulent discharges from the urethra revealed some gram-negative bean- shaped bacteria located in the leukocytes. They can be identified as the causative agent of the following disease:
42. A male patient is 28 years old. Histological study of a cervical lymph node revealed a change of its pattern due to the proliferation of epithelioid, lymphoid cells and macrophages having nuclei in form of a horseshoe. In the center of some cell clusters there were non-structured light- pink areas with fragments of nuclei. What disease are these changes typical for?
43. A 35-year-old male patient has been referred by an andrologist for the genetic counselling for the deviations of physical and mental development. Objectively: the patient is tall, has asthenic constitution, gynecomastia, mental retardation. Microscopy of the oral mucosa cells revealed sex chromatin (single Barr body) in 30% of cells. What is the most likely diagnosis?
44. A patient with jaundice has high total bilirubin that is mainly indirect (unconjugated), high concentration of stercobilin in the stool and urine. The level of direct (conjugated) bilirubin in the blood plasma is normal. What kind of jaundice can you think of?
45. A male with a lesion of one of the CNS parts has asthenia, muscular dystonia, balance disorder. Which CNS part has been affected?
Explanation
During cerebellar lesions, there are disturbances in posture, equilibrium and movements. Disturbances in movements: Speech disorders, ataxia, asynergia, asthenia (weak muscle contractions with characteristically rapid onset of muscle fatigue), Dysmetria, Intention tremor, astasia (loss of the capacity for sustained tetanic contractions), nystagmus, rebound phenomenon, dysarthria, adiadochokinesis, atonia (lack or impairment of muscle tone).
NB: Scanned or staccato speech is as a result of cerebellar disorders; while monotonus speech is as a result of parkinson's disease.
46. A 50-year-old patient has been administered laevomycetin for the treatment of typhoid fever, but on the next day the patient’s condition worsened, the temperature rose to 39, 60C . The deterioration of the patient’s condition can be explained by:
47. A 12-year-old patient has been admitted to a hospital for hemarthrosis of the knee joint. From early childhood he suffers from frequent bleedings. Diagnose the boy’s disease:
Explanation
Hemophilia is a genetic disorder. Its an intrinsic coagulation pathway defect. Since its genetic, it can manifest early in life (childhood). Types:
Hemophilia A: X-linked recessive; deficiency of factor VIII
Hemophilia B: X-linked recessive; deficiency of factor IX
Hemophilia C: Autosomal recessive; deficiency of factor XI
Findings: macrohemorrhage in hemophilia – hemarthroses (bleeding into joints, such as knee), easy bruising, bleeding after trauma or surgery (e.g. dental procedures).
Idiopathic or Immune thrombocytopenic purpura: characterized by bleeding which results from unusually low levels of platelets, affects both and children and adults. Children often develop Idiopathic thrombocytopenic purpura after a viral infection and usually recover fully without treatment. In adults, however the disorder is often chronic.
Hemorrhagic vasculitis is an inflammatory disorder characterized by a generalized vasculitis involving the small vessels of the skin, GI tract, kidneys, joints and rarely the lungs and CNS. It is the most common vasculitis in children. It is an immune complex HSR disease; inciting agents (antigens) include: group A β-hemolytic streptococci and other bacteria, viruses, drugs, food, insect bites.
48. Examination of a patient with ischemic heart disease revealed the impaired venous blood flow in the territory of the cardiac vein running in the anterior interventricular sulcus of heart. What vein is it?
49. For the direct injection of medications into the liver surgeons use the round ligament of liver. This manipulation involves bougienage (lumen dilatation) of the following vessel:
50. A patient with lobar pneumonia has had body temperature of 39oC with daily temperature fluctuation of no more than 1oC for 9 days. This fever can be characterized by the following temperature curve:
51. The temperature in a production room is 36oC . Relative air humidity is 80%. Under these conditions the human body transfers heat mainly through:
52. A hospitalized patient bitten by a rabid animal has an avulsive wound of shin. What kind of vaccine must be given to prevent rabies?
53. At autopsy the occipital lobe of brain was found to have a cavity 2,5x1,5 cm large filled with a transparent liquid. The cavity had smooth brownish walls. What process had developed in the brain?
54. A child entering the school for the first time was given Mantoux test in order to determine if there was a need for revaccination. The reaction was negative. What is the meaning of this test result?
Explanation
Tuberculin (Mantoux) skin test: this test is done by intradermal injection of tuberculoprotein (tuberculin), purified protein derivative (PPD). Type IV hypersensitivity reaction.
Immunization against tuberculosis is induced by injection of attenuated strains of bovine type of tubercle bacilli, Bacilli Calmette Guerin (BCG).
The Mantoux skin test should be read between 48 and 72hrs after administration. The basis of reading is the presence or absence of induration, which may be determined by inspection and by palpation. A record should also be made of formation of vesicles, bullae, lymphangitis, ulceration and necrosis at the test site. The formation of vesicles, bullae or necrosis at the test site indicates positive result. A negative mantoux result usually signifies that the individual has never been exposed to Mycobacterium tuberculosis i.e. absence of cell mediated immunity to tuberculin.
Mantoux test is a type IV Hypersensitivity reaction (HSR), which involves macrophages,T-lymphocytes and lymphokines(cytokines). Mononuclear cells (lymphocytes,monocytes,macrophages).
55. Study of the biopsy material revealed a granuloma consisting of lymphocytes, plasma cells, macrophages with foamy cytoplasm (Mikulicz cells), many hyaline globules. What disease can you think of?
Explanation
Microscopic examination of specific granulomas:
* In Rhinoscleroma of nose, the granuloma (scleroma) consists of plasma cells, epitheloid cells, lymphocytes and hyaline sphere. Large macrophages with light cytoplasm containing klebsiella rhinoscleromatis (Mikulicz’s cells), sclerosis and hyalinosis takes place.
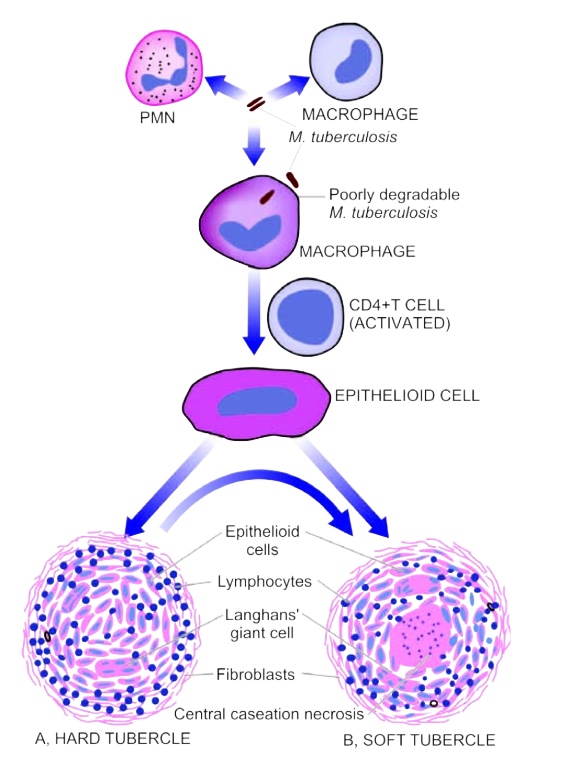
* In TB, the granuloma is reffered to as a tubercle and is classically characterized by the presence of central necrosis surrounded by epitheloid cells, lymphocytes, plasma cells and giant langhance cells. In contrast, caseous necrosis is rare in other granulomatous diseases.
* The syphilis granuloma is calle Gumma. Gumma consist of a central area of fibrinoid or caseous necrosis surrounded by mononuclear inflammatory cells, mostly plasma cells, lymphocytes, epitheloid cells and seldom-giant langhance cells. Around gumma forms the granulation tissue and endovasculitis.
* In Tuberculoid Leprosy, the epidermis contains confluent granulomas composed of macrophages, plasma cells and leprous Virchow’s cells – Leprous Virchow’s cells (or Leprous cells) refer to large foamy macrophages within fatty vacuoles containing leprous mycobacterium.
* Actinomycosis caused by Actinomyces. It occurs rarely in human but rather frequently in cattle. Characterized by the formation of painful abscess. Infected man often have poor oral hygiene or recent dental work. Does not form granulomas.
56. Autopsy of a 78-year-old patient revealed that retroperitoneal tissue was soaked with blood, the abdominal aorta had a sacciform protrusion including a defect with irregular edges. The wall of the aorta was here and there of stone-like density. This is the complication of the following disease:
57. Glycogen polysaccharide is synthesized from the active form of glucose. The immediate donor of glucose residues during the glycogenesis is:
58. After the diagnostic tests a 40-year-old male has been referred for the lymphography of the thoracic cavity. The surgeon revealed that the tumor had affected an organ whose lymphatic vessels drain directly into the thoracic duct. Specify this organ:
59. A patient with biliary dyskinesia and constipations has been prescribed a cholagogue having also a laxative effect. What drug has been administered?
60. It is known that individuals with genetically caused deficiency of glucose 6-phosphate dehydrogenase may develop RBC hemolysis in response to the administration of some antimalarial drugs. Manifestation of adverse reactions to drugs is called:
61. A 40-year-old patient with the progressing staphylococcal purulent periodontitis developed purulent inflammation of bone marrow spaces of the alveolar process, and then of the body of mandible. Microscopy revealed thinning of bone trabeculae, foci of necrosis, bone sequesters surrounded by the connective tissue capsule. What is the most likely diagnosis?
62. Curariform substances introduced into a human body cause the relaxation of all skeletal muscles. What changes in the neuromuscular synapse cause this phenomenon?
63. A number of diseases can be diagnosed by evaluating activity of blood transaminases. What vitamin is one of cofactors of these enzymes?
64. After a car accident a 23-year-old male presented to the hospital with a cut wound of the anteromedial region of shoulder and arterial bleeding. Which artery was damaged?
65. During the operation on the small intestine the surgeon revealed an area of the mucous membrane with a single longitudinal fold among the circular folds. Which portion of the small intestine is this structure typical for?
66. 14 days after quinsy a 15-year-old child presented with morning facial swelling, high blood pressure, \"meat slops\"urine. Immunohistological study of a renal biopsy sample revealed deposition of immune complexes on the basement membranes of the capillaries and in the glomerular mesangium. What disease developed in the patient?
67. A diseased child has a high fever, sore throat, swelling of submandibular lymph nodes. Objectively: pharyngeal mucosa is edematous, moderately hyperemic, the tonsils are enlarged, covered with grayish membrane tightly adhering to the tissues above. Attempts to remove the membrane produce the bleeding defects. What di- sease are these presentations typical for?
68. Study of the biopsy material of an embryo revealed a zone of developmental abnormality in a somite. The zone was located close to the endoderm and the notochord. What formations may have abnormal development in case of pregnancy continuation?
69. A smear of sputum from the patient with suspected lobar pneumonia was stained with the use of the following stains and reagents: solution of gentian violet, Lugol’s solution, 96o alcohol, water magenta. What staining method was applied in this case?
70. A patient has normally coloured stool including a large amount of free fatty acids. The reason for this is a disturbance of the following process:
71. Examination of the removed stomach revealed a deep roundish defect with regular edges at the lesser curvature of the antrum. The defect reached the muscular tunic and was 1,5 cm in diameter. Within the defect floor there was a translucent dense area resembling of a hyaline cartilage. What process had developed in the floor of the stomach defect?
72. By the decarboxylation of glutamate in the CNS an inhibitory mediator is formed. Name it:
73. Thermometry revealed that the temperature of the exposed skin is by 1-1,5oC lower than the temperature of the adjacent areas covered with clothing from natural fabrics. The reason for this is that the clothes reduce the heat loss through:
74. A specimen of pia mater includes a vessel whose wall doesn’t have the tunica media, the tunica externa is adherent to the surrounding tissues, the intima is composed of a basement membrane and endothelium. What vessel is it?
75. A patient with extensive burns of torso skin exhibits signs of severe intoxication. What stage of the burn disease is this typical for?
76. As a result of a craniocerebral injury a patient has a decreased skin sensitivity. What area of the cerebral cortex may be damaged?
77. A histological specimen of the eyeball shows a biconvex structure connected to the ciliary body by the fibers of the Zinn’s zonule and covered with a transparent capsule. Name this structure:
78. A comatose patient was taken to the hospital. He has a history of diabetes mellitus. Objectively: Kussmaul breathing, low blood pressure, acetone odor of breath. After the emergency treatment the patient’s condition improved. What drug had been administered to the patient?
79. In order to stimulate breathing in a child born with asphyxia, the doctor gave him a drug injection into the umbilical vein. What drug might have been injected?
80. A patient complains of pain in the right lateral abdomen. Palpation revealed a dense, immobile, tumor-like formation. A tumor is likely to be found in the following part of the digestive tube:
Explanation
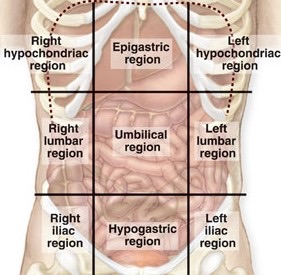

Anterolateral abdominal wall has 9 regions and 4 quadrants (RUQ, LUQ, RLQ, LLQ)
· Right lateral abdominal region: Ascending colon (colon ascendens), right kidney, right ureter and loops of small intestine.
· Umbilical region: Transverse colon (colon transversum), head of pancreas, duodenum (except superior part)
· Left lateral abdominal region: Descending colon (colon descendens), left kidney, left ureter and loops of small intestine.
· Left inguinal region: Sigmoid colon (colon sidmoideum), left ureter, left external iliac artery of artery and vein.
· Right Inguinal region: Caecum, vermiform appendix, right ureter
81. A patient underwent biopsy of the soft palate arches for a suspected tumor (macroscopy revealed an ulcer with a dense floor). Study of the biopsy material revealed mucosal necrosis with infiltration of lymphocytes, epithelioid cells, plasma cells, single neutrophils in the submucosa. There were also apparent signs of endovasculitis and perivasculitis. The described changes are typical for:
82. Healthy parents with unremarkable family history have the child with multiple developmental defects. Cytogenetic analysis revealed the trisomy 13 in the somatic cells (Patau syndrome). What phenomenon has caused the defects?
Explanation
In preparation for fertilization, germ cells undergo gametogenesis, which includes meiosis, to reduce the number of chromosomes. Chromosomal abnormalities may be numerical or structural. Abnormalities in chromosome number may originate during meiotic or mitotic divisions. In meiosis, two members of a pair of homologous chromosomes normally separate during the first meiotic division, so that each daughter cell receives one member of each pair. Sometimes, however, separation does not occur (nondisjunction) and both members of a pair move into one cell. As a result of nondisjunction of the chromosomes, one cell receives 24 chromosomes and the other receives 22 instead of the normal 23. When at fertilization a gamete having 23 chromosomes fuses with a gamete having 24 or 22 chromosomes, the result is an individual with either 47 chromosomes (e.g.trisomy 13, 18,21, klinefelter) or 45 chromosomes (monosomy – 45 XO turner’s syndrome). Nondisjunction which occurs during either the first or the second meiotic division of the germ cells, may involve the autosomes (trisomy 13,18,21) or sex chromosomes (turner’s and klinefelter’s syndrome).
If nondisjunction occurs during mitosis (mitotic nondisjunction) – such conditions produce mosaicism, with some cells having an abnormal chromosome number and others being normal. Therefore abnormal gametogenesis can produce nondisjunction.
83. A specimen shows an organ covered with the connective tissue capsule with trabeculae radiating inward the organ. There is also cortex containing some lymph nodules, and medullary cords made of lymphoid cells. What organ is under study?
84.
A 25-year-old patient consulted a doctor about dysmenorrhea and infertility. Examination revealed that the patient was 145 cm high and had underdeveloped secondary sex characteristics, alar folds on the neck. Cytological study didn’t reveal any Barr bodies in the somatic cells. What diagnosis was made?
85. To prevent attacks of acute pancreatitis a doctor prescribed the patient trasylol (contrycal, gordox), which is an inhibitor of:
86.
A patient died from progressive heart failure. Autopsy revealed that the heart was enlarged in diameter, flabby. The muscle section exhibited irregular blood supply. Histological study of myocardium revealed hyperemia, the stroma was found to have lymphohistiocytic infiltrates with degeneration of cardiomyocytes. The revealed morphological changes are indicative of:
87.
A 13-year-old teenager underwent X-ray examination of the hip joint. Examination revealed a 3mm wide radiolucent zone between the head and the shaft of femur. This situation should be evaluated as:
88.
A surgeon examined the patient and found the injury of the upper third of the kidney. Considering the syntopy of the left kidney, the intactness of the following organ should be checked at the same time:
89.
A patient with urolithiasis has unbearable spasmodic pain. To prevent pain shock, he has been given an injection of atropine along with a narcotic analgesic having antispasmodic effect. What drug was it?
90.
Despite the administration of cardiotonics and a thiazide diuretic a patient with chronic heart failure has persistent edemata, there is a risk of ascites. What medication should be administered in order to enhance the diuretic effect of the drugs used?
91.
A patient with a pathology of the cardiovascular system developed edemata of the lower extremities. What is the mechanism of cardiac edema development?
92. During the fight, a man had a cardiac arrest due to the strong blow to the upper region of the anterior abdominal wall. Which of the following mechanisms has led to the cardiac arrest?
93. A pregnant woman underwent AB0 blood typing. Red blood cells were agglutinated with standard sera of the I and II blood groups, and were not agglutinated with the III group serum. What is the patient’s blood group?
94.
Amniocentesis revealed two sex chromatin bodies (Barr bodies) in each cell of the sample. What disease is this character typical for?
95.
A hospital has admitted a patient complaining of abdominal bloating, diarrhea, flatulence after eating protein foods. These signs are indicative of the impaired digestion of proteins and their increased degradation. Which of the following compounds is the product of this process?
96.
An attack of tachycardia that occurred in a patient was stopped by pressing on his eyeballs. Which of the following reflexes underlies this phenomenon?
97. A male patient has been diagnosed with acute post-streptococcal glomerulonephritis. It is most likely that the lesion of the basement membrane of renal corpuscles was caused by the following allergic reaction:
98.
An unconscious patient was taken by ambulance to the hospital. On objective examination the patient was found to have no reflexes, periodical convulsions, irregular breathing. After laboratory examination the patient was diagnosed with hepatic coma. Disorders of the central nervous system develop due to the accumulation of the following metabolite:
Explanation
Substances absorbed into the bloodstream from the intestine pass through the liver, where toxins are normally removed. Many of these toxins (such as ammonia) are normal breakdown products of the digestion of protein. In hepatic encephalopathy (hepatic coma), toxins are not removed because liver function is impaired. Ammonia is produced by amino acid metabolism and intestinal urease-positive bacteria. In physiological conditions, it is mostly present as ammonium (NH4+) in serum. The urea or ornithine cycle, which is fully expressed in the liver exclusively, serves to converts NH4+ to urea prior to renal excretion and to maintain low serum concentrations. In hepatic coma, when the liver cannot remove toxins and urea cycle is not functional, all this occurs:
NH3 + α-ketoglutarate → Glutamate
α-ketoglutarate is used up which leads to:
· ↑glutamate → ↑GABA (inhibitory neurotransmitter)
· Inhibition of citric acid cycle/tricarboxylic acid cycle; this causes impairment of ATP formation.
· Inhibition of metabolism of amino acids (impairment of transamination reactions).
NH3 + Glutamate → Glutamine
Glutamine is an amide of glutamic acid which provides a non-toxic storage and transport form of ammonia (NH3). Ammonia increase synthesis of glutamine in brain. Accumulation of glutamine in brain results in elevation of osmotic pressure in nervous cells leading to brain edema.
NH3 + H+ → NH4+
In blood ammonia (NH3) is represented as ammonium ion (NH4+). Accumulation of ammonium ion impairs transport of ions (Na+, K+) through cell membranes and failure of transmission of nerve impulse.
Urea cycle takes place exclusively in the liver, so in hepatic coma, urea level is low. Glutamine toxicity in brain is dependent on increased ammonia concentration.
Bilirubin toxicity will most likely be related to increase hemolysis, which is not the case in this question. Histamine is a biogenic amine produced from the amino acid histidine.
99.
A 20-year-old male patient complains of general weakness, rapid fatigability, irritability, decreased performance, bleeding gums, petechiae on the skin. What vitamin deficiency may be a cause of these changes?
Explanation
Vitamin C (ascorbic acid): found in fruits and vegetables; an antioxidant; also facilitates iron absorption by reducing it to Fe2+ state. It is necessary for hydroxylation of proline and lysine in collagen synthesis; necessary for dopamine β-hydroxylase, which converts dopamine to norepinephrine. Deficiency leads to: scurvy – swollen gums, bruising, petechiae, hemarthrosis, anemia, poor wound healing, perifollicular and subperiosteal hemorrhages, “corkscrew” hair; Weakened immune response.
Type III collagen is found in blood vessels; Type IV collagen is found in basement membrane. Deficiency in Vitamin C disrupts the second stage of collagen synthesis in fibroblasts (hydroxylation of collagen) which results in petechiae, bruising, hemarthrosis.
Vitamin B2 (riboflavin) deficiency – growth retardation, glossitis, conjunctivitis
Vitamin B1 (thiamine) deficiency – Beri-Beri (polyneuritis)
Vitamin A (retinol) deficiency – Night blindness
Vitamin B9 (folic acid) deficiency – macrocytic megaloblastic anemia
100.
It is known that the monoamine oxidase (MAO) enzyme plays an important part in the metabolism of catecholamine neurotransmitters. In what way does the enzyme inactivate these neurotransmitters (norepinephrine, epinephrine, dopamine)?
101. The cellular composition of exudate largely depends on the etiological factor of inflammation. What leukocytes are the first to get into the focus of inflammation caused by pyogenic bacteria?
Explanation
Neutrophils are the first leukocytes that cross the blood vessel wall to enter inflammatory sites. Under normal conditions, leukocytes are restricted to the center of small blood vessels, where the flow is fastest. In inflammatory sites, where the vessels are dilated, the slower blood flow allows the leukocytes to move out of the center of the blood vessel and interact with the vascular endothelium. Even in the absence of infection, monocytes migrate continuously into the tissues, where they differentiate into macrophages; meanwhile, during an inflammatory response, the induction of adhesion molecules on the endothelial cells, as well as induced changes in the adhesion molecules expressed on leukocytes recruit large numbers of circulating leukocytes, initially Neutrophils and later monocytes, into the site of an infection (inflammatory focus).
First –Neutrophils; second –monocytes and macrophages; third –lymphocytes.
102.
At the end of the working day a worker of a hot work shop has been delivered to a hospital. The patient complains of a headache, dizziness, nausea, general weakness. Objectively: the patient is conscious, his skin is hyperemic, dry, hot to the touch. Heart rate is of 130/min. Respiration is rapid, superficial. What disorder of thermoregulation is most likely to have occurred in this patient?
103.
Alveolar space of the acinus was invaded by some bacteria which interacted with the surfactant. This led to the activation of the cells that are localized in the alveolar walls and on the surface. What cells are these?
Explanation
Alveolar macrophages remove inhaled particulate matter from the air spaces and red blood cells (RBCs) from the septum of alveoli. They are unusual in that they function both in the connective tissue of the septum (alveolar wall) and in the air space of the alveolus (surface of alveolar cells). In air spaces they scavenge the surface to remove inhaled particulate matter (e.g. dust, pollen, pathogens), thus giving them one of their alternate names – Dust cells. They also phagocytose infectious organisms such as Mycobacterium tuberculosis. Other macrophages remain in the septal connective tissue, where, filled with accumulated phagocytized material, they may remain for much of an individual’s life. Thus, at autopsy, the lungs of urban dwellers as well as smokers will usually show many alveolar and septal macrophages filled with carbon particles, anthracotic pigment and birefringent needle-like particles of silica.
Type I alveolar cells (type I pneumocytes): the junctions formed between this cells form an effective barrier between the air space and the components of the septal wall. They are not capable of cell division. They make up 95% of the surface of the alveoli.
Type II alveolar cells: secretory cells; have lamellar bodies; progenitor cells for type I alveolar cells.
Clara cells: non-ciliated; low columnar/cuboidal cell with secretory granules. They secrete components of surfactant, degrade toxins and act as reserve cells.
Endothelial cells line blood vessels.
104.
A 35-year-old male developed acute heart failure while running for a long time. What changes in the ionic composition can be observed in the cardiac muscle?
105. Workers of a conveyor workshop received recommendations for the effective organization of working time and higher working efficiency. What peculiarity of work in this workshop causes the greatest stress for the workers?
106.
Mother of a boy who had recently returned from a summer camp found some small whitish insects up to 3 mm long on the child’s clothing. Specify the parasite:
107.
Histological examination of the removed skin neoplasm revealed clusters and cords of atypical cells of stratified squamous epithelium, growing into the underlying tissue. What diagnosis can be assumed?
108.
An 18-year-old male has been diagnosed with Marfan syndrome. Examination revealed a developmental disorder of connective tissue and eye lens structure, abnormalities of the cardiovascular system, arachnodactylia. What genetic phenomenon has caused the development of this disease?
109.
A patient has severe catarrhal symptoms. Material growth on Bordet-Gengou agar showed mercury-drop-like colonies. Examination of the blood smears revealed some small ovoid gram-positive bacilli sized 1-3 microns. What microorganisms were isolated?
110. A 66-year-old patient with Parkinson’s disease shows an improvement in locomotor activity after prolonged use of a certain drug which is converted to dopamine by the decarboxylation. What drug has the patient taken?
111.
Enzymatic jaundices are accompanied by abnormal activity of UDP-glucuronyl transferase. What compound is accumulated in blood serum in case of these pathologies?
112.
For the study of serum proteins various physical and physicochemical methods can be used. In particular, serum albumins and globulins can be separated by this method:
113. Negative environmental factors have caused the dysfunction of myosatellite cells. What function of the whole muscle fibre is likely to be changed in this case?
114.
The laboratory for especially dangerous infections conducts microscopic examination of pathological material from a patient with suspected plague. The sample was stained by Burri-Gins technique. What property of the causative agent can be identified by this technique?
115. Autopsy of a 62-year-old woman revealed a dense well-circumscribed node of 6 cm in diameter in the cranial cavity. The node was attached to the dura mater and histologically consisted of clusters and micro-concentric structures of endothelial cells, psammoma bodies. What kind of tumor was found at autopsy?
116.
Inherited diseases, such as mucopolysaccharidoses, are manifested in metabolic disorders of connective tissue, bone and joint pathologies. The sign of this disease is the excessive urinary excretion of the following substance:
117. An animal has an increased tonus of extensor muscles. This is the result of enhanced information transmission to the motoneurons of the spinal cord through the following descending pathways:
118.
A specimen of a parenchymal organ shows poorly delineated hexagonal lobules surrounding a central vein, and the interlobular connective tissue contains embedded triads (an artery, a vein and an excretory duct). What organ is it?
119.
A patient has been admitted to the infectious diseases department for malaise, fever up to 38oC , jaundice. A few months ago, the patient underwent blood transfusion. The doctor suspected viral hepatitis B. What are the principal methods of laboratory diagnosis of hepatitis B?
120.
After resection of the middle third of the femoral artery obliterated by a thrombus the limb is supplied with blood through the bypasses. What artery plays the main part in the restoration of the blood flow?
121.
During the intravenous transfusion of the saline the patient’s condition deteriorated dramatically, and the patient died from asphyxiation. Autopsy revealed acute venous congestion of internal organs with the dramatic right heart dilatation. When the right ventricle was punctured underwater, the bubbles escaped. What pathological process occurred in the patient?
122.
At the post-mortem examination the stomach of a patient with renal failure was found to have a yellow-brown coating on the thickened mucosa. The coating was firmly adhering to its surface and had significant thickness. Microscopy revealed congestion and necrosis of mucosal and submucosal layers, fibrin presence. What is the most likely diagnosis?
123.
Infectious diseases are treated with antibiotics (streptomycin, erythromycin, chloramphenicol). They inhibit the following stage of protein synthesis:
124. Diseases of the respiratory system and circulatory disorders impair the transport of oxygen, thus leading to hypoxia. Under these conditions the energy metabolism is carried out by anaerobic glycolysis. As a result, the following substance is generated and accumulated in blood:
125.
A patient has been hospitalized for a suspected tumor of the prostate. During the surgery, it was revealed that the tumor invaded the bladder. Which part of the bladder was affected?
126. A casualty with an injury of the temporal region has been diagnosed with epidural hematoma. Which of the arteries is most likely to be damaged?
127.
A 19-year-old male was found to have an elevated level of potassium in the secondary urine. These changes might have been caused by the increase in the following hormone level:
128.
Analysis of the ECG revealed the missing of several PQRST cycles. The remaining waves and complexes are not changed. Specify the type of arrhythmia:
129.
ECG of a patient displays an abnormally long R wave (up to 0,18 s). This is caused by a decrease in the conduction velocity of the following heart structures:
130.
6 hours after the myocardial infarction a patient was found to have elevated level of lactate dehydrogenase in blood. What isoenzyme should be expected in this case?
131.
A 46-year-old female is scheduled for a maxillofacial surgery. It is known that the patient is prone to high blood coagulation. What natural anticoagulant can be used to prevent blood clotting?
132.
A 50-year-old patient with food poisoning is on a drip of 10% glucose solution. It not only provides the body with necessary energy, but also performs the function of detoxification by the production of a metabolite that participates in the following conjugation reaction:
133. To assess the effectiveness of breathing in patients, the indicator of functional residual capacity is used. It includes the following volumes:
134. It is required to evaluate the level of tissue excitability. For this purpose one should determine:
135.
Due to the use of poor-quality measles vaccine for preventive vaccination, a 1-year-old child developed an autoimmune renal injury. The urine was found to contain macromolecular proteins. What process of urine formation was disturbed?
136. A patient has been administered an anti-inflammatory drug that blocks the action of cyclooxygenase. Specify this anti-inflammatory agent:
137.
A pneumonia patient has been administered acetylcysteine as a part of complex therapy. What principle of therapy was taken into consideration when applying this drug?
138.
A 26-year-old female patient with bronchitis has been administered a broad spectrum antibiotic as a causal treatment drug. Specify this drug:
139.
A 65-year-old male suddenly lost the vision in one eye due to the retinal detachment. The patient underwent enucleation. Histological examination of the removed eye retina and choroid revealed clusters of atypical cells with marked polymorphism of cells and nuclei, with a moderate number of mitoses including the pathological ones. The cell cytoplasm and intercellular medium contained brown pigment giving a positive DOPA reaction. Perls’ reaction was negative. What is the most likely diagnosis?
140.
A child cut his leg with a piece of glass while playing and was brought to the clinic for the injection of tetanus toxoid. In order to prevent the development of anaphylactic shock the serum was administered by Bezredka method. What mechanism underlies this method of desensitization of the body?
141.
Microscopy of the myocardium of a patient who had died from heart failure revealed foci of fibrinoid necrosis located diffusely in the interstitial stroma, and often around the vessels. Such foci were surrounded by lymphocytes, macrophages, histiocytes. Pericardium was found to have signs of sero-fibrinous pericarditis. What is the most likely diagnosis?
142.
One of the factors that cause obesity is the inhibition of fatty acids oxidation due to:
143.
The genetic defect of pyruvate carboxylase deficiency is the cause of delayed physical and mental development and early death in children. This defect is characterized by lacticemia, lactaciduria, disorder of a number of metabolic pathways. In particular, the following process is inhibited:
144.
Deficiency of linoleic and linolenic acids in the body leads to the skin damage, hair loss, delayed wound healing, thrombocytopenia, low resistance to infections. These changes are most likely to be caused by the impaired synthesis of the following substances:
145.
During ventricular systole, the cardiac muscle does not respond to additional stimulation because it is in the phase of:
146. A mother had taken synthetic hormones during pregnancy. Her daughter was born with hirsutism formally resembling of adrenal syndrome. Such manifestation of variability is called:
147. Since a patient has had myocardial infarction, atria and ventricles contract independently from each other with a frequency of 60-70 and 35-40 per minute. Specify the type of heart block in this case:
148.
A 67-year-old male patient consumes eggs, pork fat, butter, milk and meat. Blood test results: cholesterol - 12,3 mmol/l, total lipids - 8,2 g/l, increased low- density lipoprotein fraction (LDL). What type of hyperlipoproteinemia is observed in the patient?
149.
A 12-year-old child has a viral infection complicated by obstructive bronchitis. Bronchospasm can be eliminated by inhalations of a drug from the following pharmacological group:
150.
In course of an experiment there has been an increase in the nerve conduction velocity. This may be caused by an increase in the concentration of the following ions that are present in the solution around the cell:
151.
A male working as a blacksmith has been tested for auditory acuity. The tests revealed 50% hearing loss in the low-frequency range and a near-normal auditory acuity in the high-frequency range. This condition has been caused by the damage to the following structures of the auditory system:
152.
In our country, routine preventive vaccinations against poliomyelitis involve using live vaccine that is administered orally. What immunoglobulins are responsible for the development of local post-vaccination immunity in this case?
153.
An experiment proved that UV-irradiated skin cells of patients with xeroderma pigmentosum restore the native structure of DNA slower than the cells of healthy people due to the defect in repair enzyme. What enzyme takes part in this process?
154.
A patient who has recently come from an endemic area presents with elevated body temperature, headache, chills, malaise, that is with the symptoms which are typical for a common cold. What laboratory tests are necessary to confirm or to refute the diagnosis of malaria?
155.
What condition may develop 15-30 minutes after re-administration of the antigen as a result of the increased level of antibodies, mainly IgE, that are adsorbed on the surface of target cells, namely tissue basophils (mast cells) and blood basophils?
Explanation
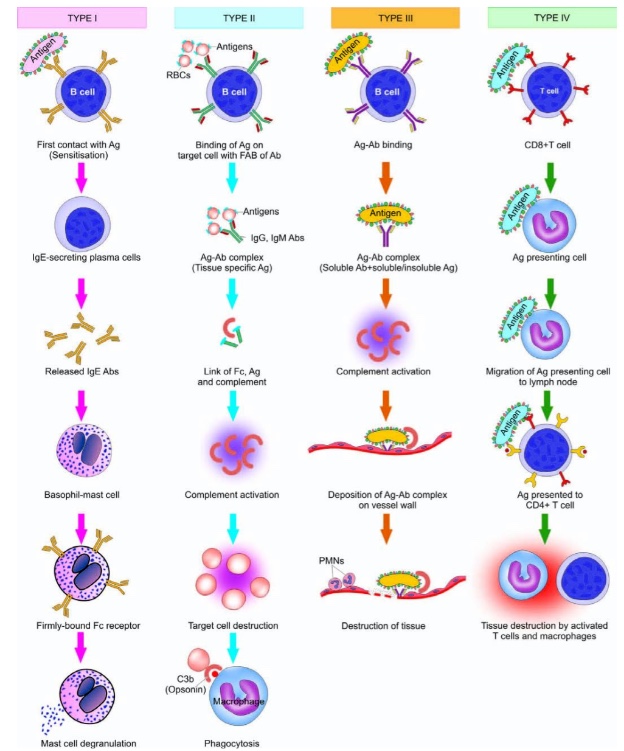
Type I Hypersensitivity reaction (HSR); anaphylactic and atopic: free antigen cross-links IgE on presensitized (i.e. exposed to the antigen before) mast cells and basophils, triggering immediate release of vasoactive amines that act at postcapillary venules (i.e. histamine). Reaction develops rapidly after antigen exposure because of preformed antibody from first exposure. IgE is the main immunoglobulin involved in type I HSR. Type I: uses IgE and IgG4
Type I (Immediate, Anaphylaxis, Reagin): IgE (immunoglobulin E)-dependent activation of mast cells/basophils, usually accompanied by eosinophilia e.g. urticaria (hives), hay fever, asthma (wheezing), rhinitis and conjunctivitis (stuffy nose and itchy eyes; usually seasonal)
Type II (cytotoxic): antibody dependent reactions e.g. Goodpasture syndrome, Myasthenia gravis, Graves disease, ABO hemolytic disease of newborn etc.
Type III (immune-complex): deposition of antigen-antibody complexes e.g. systemic lupus erythromatous (SLE), Arthus reaction, serum sickness, poststreptococcal glomerulonephritis etc.
Type IV (cell mediated, delayed): antibody-independent T-cell mediated reactions e.g. positive mantoux reaction (tuberculin test), hashimoto’s thyroiditis or transplant rejection etc.
156.
10 days after having quinsy caused by beta-hemolytic streptococcus a 6- year-old child exhibited symptoms of glomerulonephritis. What mechanism of glomerular lesion is most likely in this case?
157.
A 22-year-old woman ate some seafood. 5 hours later the trunk and the distal parts of limbs got covered with small itchy papules which were partially fused together. After one day, the rash disappeared spontaneously. Specify the hypersensitivity mechanism underlying these changes:
158.
A hypertensive patient had been keeping to a salt-free diet and taking antihypertensive drugs together with hydrochlorothiazide for a long time. This resulted in electrolyte imbalance. What disorder of the internal environment occurred in the patient?
159.
A miner consulted a physician about the appearance of body rash followed by a loss of appetite, bloating, duodenal pain, frequent bowel movements, dizziness. Ovoscopic probes of feces and duodenal contents revealed some eggs covered with a transparent membrane through which 4-8 germinal cells could be seen. What disease is likely to have occurred in the patient?
160. Children with Lesch-Nyhan syndrome have a severe form of hyperuricemia accompanied by the formation of tophi, urate calculi in the urinary tracts, as well as serious neuro-psychiatric disorders. The cause of this disease is the reduced activity of the following enzyme:
161.
In a car accident a man got injured and lost a lot of blood. What changes in peripheral blood are most likely to occur on the 2nd day after the injury?
162.
In the surgical ward, the dressing material was undergoing sterilization in an autoclave. Through an oversight of a nurse the mode of sterilization was changed and the temperature in the autoclave reached only 100oC instead of the due 120oC . What microorganisms can stay viable under these conditions?
163.
As a result of a mechanical injury an over 10 cm long portion of a peripheral nerve was damaged. This led to the impairment of the upper limb activity. The patient was offered nerve transplantation. What glial cells will participate in regeneration and provide the trophism of the injured limb?
164. A 26-year-old woman at 40 weeks pregnant has been delivered to the maternity ward. Objectively: the uterine cervix is opened, but the contractions are absent. The doctor has administered her a hormonal drug to stimulate the labor. Name this drug:
165.
A patient has recurrent attacks of epileptic seizures and stays unconscious between them. In order to stop convulsions the drugs of the following group should be used in the first place:
166.
A patient with arthritis and varicose veins has been taking a non-steroidal anti-inflammatory drug for a long time, which caused thrombosis of skin veins. Which of the following drugs might have caused this complication?
167.
Students study the stages of gametogenesis. They analyze a cell having a haploid number of chromosomes, and each chromosome consists of two chromatids. The chromosomes are located in the equatorial plane of the cell. Such situation is typical for the following stage of meiosis:
168.
A 35-year-old female patient underwent biopsy of the breast nodules. Histological examination revealed enhanced proliferation of the small duct epithelial cells and acini, accompanied by the formation of glandular structures of various shapes and sizes, which were located in the fibrous stroma. What is the most likely diagnosis?
169. Examination of the duodenal contents revealed some pear-shaped protozoa with two nuclei and four pairs of flagella. The organisms had also two axostyles between the nuclei and a ventral adhesive disc. What protozoan representative was found in the patient?
170.
A specimen of an onion rootlet includes a cell in which the fully condensed chromosomes are located in the equatorial plane making the monaster. What phase of the mitotic cycle is the cell in?
171.
When examining a patient, the doctor revealed a tumor of the bronchus which borders on the aorta. Which bronchus is affected?
172.
A 54-year-old female was brought to the casualty department after a car accident. A traumatologist diagnosed her with multiple fractures of the lower extremities. What kind of embolism is most likely to develop in this case?
173. Microscopy of the bronchial wall revealed atrophy of the mucosa, metaplastic change from columnar to squamous epithelium, an increase in the number of goblet cells, diffuse infiltration of the bronchial wall with lymphoplasmacytic elements with a large number of neutrophilic granulocytes, pronounced sclerosis. Specify the morphological form of bronchitis:
174.
Due to the blockage of the common bile duct (which was radiographically confirmed), the biliary flow to the duodenum was stopped. We should expect the impairment of:
175.
Typical manifestations of food poisoning caused by C. botulinum are double vision, abnormal functioning of the swallowing and breathing. These symptoms develop as a result of:
176.
At the stage of translation in the rough endoplasmic reticulum, the ribosome moves along the mRNA. Amino acids are joined together by peptide bonds in a specific sequence, and thus polypeptide synthesis takes place. The sequence of amino acids in a polypeptide corresponds to the sequence of:
177. After the prolonged vomiting a pregnant 26-year-old woman was found to have the reduced volume of circulating blood. What change in the total blood volume can be the case?
178.
On allergological examination a patient has been diagnosed with pollinosis. Specific desensitization can be performed by:
179.
A patient consulted a physician about chest pain, cough, fever. Roentgenography of lungs revealed eosinophilic infiltrates which were found to contain the larvae. What kind of helminthiasis are these presentations typical for?
180.
A patient with signs of osteoporosis and urolithiasis has been admitted to the endocrinology department. Blood test revealed hypercalcemia and hypophosphatemia. These changes are associated with abnormal synthesis of the following hormone:
181.
Histological examination of the biopsy material obtained from the lower third of the esophagus of a 57-year-old male with the symptoms of continuous reflux revealed the change of the stratified squamous epithelium to the single-layer columnar glandular epithelium with signs of mucus production. Specify the pathological process in the mucous membrane:
182.
A 30-year-old female exhibits signs of virilism (growth of body hair, balding temples, menstrual disorders). This condition can be caused by the overproduction of the following hormone:
183. A patient with bacterial periodontitis has been administered iontophoresis with the use of iodine solution. Specify the mechanism of therapeutic action of this agent:
184.
A patient with extensive myocardial infarction has developed heart failure. What pathogenetic mechanism contributed to the development of heart failure in the patient?
185.
A patient who had been continuously taking drugs blocking the production of angiotensin II developed bradycardia and arrhythmia. A likely cause of these disorders is:
186.
A patient has arterial hypertension. What long-acting drug from the group of calcium channel blockers should be prescribed?
187.
Human skin has a high breaking strength. It is known that the skin consists of epithelial tissue and two kinds of connective tissue. Which of the following tissues provides the skin strength?
188.
As a result of a home injury, a patient suffered a significant blood loss, which led to a fall in blood pressure. Rapid blood pressure recovery after the blood loss is provided by the following hormones:
189.
A patient with constant headaches, pain in the occipital region, tinnitus, dizziness has been admitted to the cardiology department. Objectively: AP- 180/110 mm Hg, heart rate - 95/min. Radiographically, there is a stenosis of one of the renal arteries. Hypertensive condition in this patient has been caused by the activation of the following system:
190.
A patient complains that at the bare mention of the tragic events that once occurred in his life he experiences tachycardia, dyspnea and an abrupt rise in blood pressure. What structures of the CNS are responsible for these cardiorespiratory reactions in this patient?
191.
A patient consulted a dentist about limited mouth opening (trismus). He has a history of a stab wound of the lower extremity. What infection may cause these symptoms?
192. Anatomical dead space is the portion of the air that is left in the airways after expiration. The reduction of the anatomical dead space is typical for the following situation:
193.
Analysis of the experimental spirogram of a 55-year-old person revealed a decrease in tidal volume and respiratory amplitude compared to the situation of ten years ago. The change in these indicators is caused by:
194.
A patient underwent a course of treatment for atherosclerosis. Laboratory tests revealed an increase in the anti-atherogenic lipoprotein fraction in the blood plasma. The treatment efficacy is confirmed by the increase in:
195.
A 65-year-old female patient has chronic constipations due to the colon hypotonia. What drug should be chosen in this case?
196.
A female patient complains of vision impairment. On examination she was found to have obesity, fasting hyperglycemia. What complication of diabetes can cause vision impairment?
197.
Analysis of the family history of children with Van der Woude syndrome revealed that in their families one of the parents had the typical for this syndrome defects (cleft lip and palate, lip pits regardless of gender). What is the type of inheritance of this syndrome?
198.
Administration of doxycycline hydrochloride caused an imbalance of the symbiotic intestinal microflora. Specify the kind of imbalance caused by the antibiotic therapy:
199.
A 3-year-old child had eaten some strawberries. Soon he developed a rash and itching. What was found in the child’s leukogram?
200. A 12-year-old patient was found to have blood serum cholesterol at the rate of 25 mmol/l. The boy has a history of hereditary familial hypercholesterolemia, which is caused by the impaired synthesis of the following protein receptors: