1. During examination of a patient, the doctor detected in him disorders of the eyes (hemeralopia, Bitots spots), skin and skin appendages, mucosa, and gastrointestinal tract. He was provisionly diagnosed with Prasad\'s syndrome. What causes the development of this pathology?
2. A 45-year-old man with thrombophlebitis of the deep veins in his legs suddenly after physical exertion developed sharp pain in his thorax on the right, dyspnea, and hemoptysis. Objectively his condition is severe; he presents with acrocyanosis, shortening of pulmonary percussion^ sound on the right, and weakened respiration. Respiration is 30/min., blood pressure is 110/80 mm Hg. ECG shows sinus tachycardia, his heart rate is 120/min., the electrical axis of the heart deviates to the right, S7-Q777. What is the most likely diagnosis?
3. A 37-year-old woman received an occupational trauma that resulted in a severe vision impairment. Now she needs to be trained for another occupation. What type of rehabilitation should the doctor choose for the patient in this case?
4. A 22-year-old postparturient woman on the 12th day after the normal childbirth informs of fever up to 39°(7 for the last 3 days and pain in her right mammary gland. The right mammary gland is enlarged, hot to touch, tense, hyperemic, and painful. Palpation reveals there a dense infiltration 8x8 cm with a fluctuation in its center. What is the most likely diagnosis?
5. A 38-year-old woman has been suffering from glomerulonephritis for 20 years. For approximately 16 years she has been presenting with progressing renal parenchymal arterial hypertension that became refractory and accompanied by leg edemas. She receives a combination of 100 mg losartan and 20 mg lercanidipine with insufficient antihypertensive effect. What medicine can she be recommended for intensification of the antihypertensive effect of her therapy?
6. A 45-year-old man has been suffering from ankylosing spondylitis for 15 years. For the last 3 years he has been noticing facial swelling and edemas of the limbs. Objectively he assumes a ’’beggar’s” position. X-ray shows,’bamboo spine” changes in the thoracic and lumbar segrilents. Heart ultrasound shows aortic regurgitation. Complete blood count: Hb- 106 g/L; leukocytes - 8.9 ■ 1010 /L; ESR- 40 mm/hour. Daily proteinuria - 9.6 grams per 24 hours. Blood creatinine ⼔ 230 mcmol/L. What is the cause of kidney failure in this case?
7. A patient was brought into the pulmonology department with complaints of inspiratory dyspnea and dry cough at the highest point of inhalation. On examination the following is observed: pale skin, cyanotic lips, ’Hippocratic fingers? Auscultation detects Velcro-type crackles (like opening a Velcro fastener). X-ray shows a ’ground glass opacity” pattern. What is the most likely diagnosis?
8. A 45-year-old man came to the hematologist with complaints of general weakness, elevated body temperature, excessive sweating, enlarged cervical lymph nodes. Objectively his body temperature is 37.5°C, the skin is pale and dry the posterior cervical lymph nodes are dense and elastic, up to 2 cm in diameter, mobile. There are no peculiarities in the patient\'s heart and lungs. Hepatosplenomegaly was detected. What examination is necessary to determine the scope of the pathologic process?
9. A 65-year-old man underwent a left hemicolectomy due to a malignant tumor in the descending colon. On the 4th day after the surgery he developed pain and edema in his left shin. The Homans sign is positive on the left. What postoperative complication developed in this patient?
10. A 35-year-old forestry officer was delivered to the hospital on the 7th day after the onset of the disease. He complains of chills, elevated body temperature up to 40.0°C, sharp headache, and myalgias. On examination his face is puffy and hyperemic, the tongue is dry, \"chalk- dusted.\" In the left inguinal area, a sharply painful conglomeration of enlarged lymph nodes can be palpated. The skin over the conglomeration is hyperemic and tense. What etiotropic therapy should be prescribed to this patient?
11. Examination detected vesicles with seropurulent content on the neck, back of the head, and buttocks of an infant on the 4th day of life. The patients condition is satisfactory the child is active, all newborn reflexes can be fully induced, the umbilical cord is at the stage of mummification, the umbilical area is without any peculiarities. What disease can be suspected?
Explanation
Vesiculopustulosis is a purulent inflammation found in newborns. Their causative agents include staphylococci, streptococci, e.coli etc. Clinical features – Evanescent vesicles (a few mm in diameter —> first transparent, later muddy content —> break down over 2-3 days —> small erosions, then crusts which disappear without pigmentation. Localization - skin of buttocks, hips, inguinal folders, head. Treatment is usually local – chlorhexidine, fucorcin, brilliant green.
Pemphigus neonatorum is characterised by the presence of erythematous patches coupled with the presence of vesicles and small bullaes usually localised in the lower abdomen and on extremities. The bullaes later form crusts but pigmentation is absent.
Miliaria is also called sweat rashes, in this case we see numerous very itchy rashes caused due to the blockage or clogging of sweat glands.
12. A 65-year-old man with acute anterior myocardial infarction developed an asphyxia attack. Examination detected diffuse cyanosis. In the lungs there are numerous heterogeneous wet crackles. Heart rate is 100/min. Blood pressure is 120/100 mm Hg. What complication occurred in this patient?
13. A 13-year-old girl for a month has been complaining of fatigability dull pain in her right subcostal area, abdominal distension, and constipations. Abdominal palpation reveals positive Kehr, Murphy and Ortner signs, while Desjardins and Mayo-Robson points are painless. Ibtal bilirubin is 14.7 mcmol/L, predominantly indirect, ALT- 20 U/L, AST- 40 U/L, amylase - 6.3 mmol/L. Echocholecystography shows practically no contraction of the gallbladder. Make the provisional diagnosis:
14. A 48-year-old woman has been hospitalized due to development of tachysystolic atrial fibrillation. She has lost 5 kg of body weight within 2 months. On palpation there is a node in the left lobe of the thyroid gland. What pathology resulted in the development of this condition?
15. A 58-year-old man complains of weakness and tumor-like formations that appeared on the anterior surface of his neck and in the inguinal region. Palpation detects soft painless mobile cervical and inguinal lymph nodes up to 2 cm in diameter. The liver protrudes by 2 cm from the edge of the costal margin, the lower splenic pole is at the umbilical level. In blood: erythrocytes -3.5 • 1012 /L, Hb- 88 g/L, leukocytes -86 ■ 109 /L, band neutrophils - 1%, segmented neutrophils -10%, lymphocytes -85%, eosinophils - 2%, basophils - 0%, monocytes-2%, erythrocyte sedimentation rate - 15 mm/hour, Gumprecht shadows. What is the most likely diagnosis?
16. A newborn has a round red formation in the suprapubic region. Examination shows that urine is being discharged in pulses from the two orifices located in the lower part of this formation. Name this developmental anomaly:
17. A 28-year-old man, a teacher, after an emotional stress developed painful muscle spasms in his right hand that occur during writing; now he has to hold the pen between the second and third fingers. He has no problems with typing or writing on the blackboard; no other motor disturbances or neurological pathologies are detected. What is the most likely diagnosis?
18. A 45-year-old woman was hospitalized with complaints of periodical severe headaches against the background of elevated blood pressure up to 180/90 mm Hg, muscle weakness, and frequent urination (at night as well). Her anamnesis states that despite combining various antihypertensive drugs and adjusting their dosage her arterial hypertension cannot be corrected with drugs. The patient\'s blood serum potassium levels are 2.0 mmol/L, blood serum sodium levels are 160.0 mmol/L. Ultrasound imaging detects three- dimensional formations approximately 1.0 cm in diameter in the both adrenal glands. Selective endovascular blood sampling from the suprarenal veins was performed, which revealed significant increase of cortisol and aldosterone levels. Make the diagnosis:
19. A pregnant woman at 32 weeks of gestation with the risk of preterm labor undergoes a treatment to prevent fetal respiratory distress syndrome. What medicine was she prescribed?
20. A 45-year-old man underwent a cardiac surgery one week ago. His general state has been deteriorating since then: dyspnea at rest, retrosternal pain that irradiates to the neck, marked weakness. Objectively his body temperature is hectic. His cardiac borders are expanded, apical beat is weakened. Auscultation detects pericardial friction rub. What is the most likely diagnosis?
21. The director of a medical facility draws up a financial plan for the next year. To improve the economic well-being of his establishment, he decided to increase the amount of medical services provided. How will it change the fixed cost per unit of service?
22. A woman with the pregnancy term of 8 weeks complains of elevated temperature up to 37.6°C, skin rash that can be characterized as macular exanthema, enlargement of posterior cervical and occipital lymph nodes, small amount of bloody discharge from the genital tracts. She was examined by the infectious diseases specialist and diagnosed with rubella. What tactics should the obstetrician-gynecologist choose?
23. A surgery unit received a person with an incised stab wound on the upper third of the right thigh. Examination detects an incised stab wound 3.0x0.5x2.0 cm in size on the inner surface of the upper third of the right thigh. Bright-red blood flows from deep within the woixnd in a pulsing stream. Characterize this type of bleeding:
24. A 23-year-old woman without visible cause developed a conflicting behavior at her workplace. She accused the management of underestimating her, claimed that she can be a deputy director, because she speaks four languages, is very attractive, and can make useful connections for the company She has been dressing extravagantly flirting with her colleagues, and singing loudly in her office. In fact, she has only the training of a computer operator and speaks no foreign languages. What is the likely clinical diagnosis?
25. A 45-year-old woman undergoes an inpatient treatment. She complains of elevated body temperature up to 39.0°C, pain in her right lumbar area, turbid urine with blood. CT scan shows an area of low density within the parenchyma, no difference between the cortical and medullary layers, and increased density of the perinephric fat due to edema. What is the diagnosis?
26. A 25-year-old man was hospitalized with complaints of pain in his lower abdomen and right lumbar area that appeared one hour ago. The patienfs general state is moderately severe. Body temperature - 38.2°C, heart rate - 102/min. The tongue is dry The abdomen is painful on deep palpation in the right iliac area and in the Petit triangle. Aure-Rozanov and Gabay signs are positive. Make the provisional diagnosis:
27. A 56-year-old woman was diagnosed with stage 2 hypertension of the 2nd degree. She belongs to the group of moderate risk and has bronchial asthma. What group of drugs is CONTRAINDICATED to this patient?
28. A 68-year-old woman with congestive heart failure and left ventricular ejection fraction of <40.% receives the following pharmacotherapy scheme: ramipril, torasemide, bisoprolol, clopidogrel, and digoxin. During one of her regular examinations, frequent polymorphic ventricular extrasystoles were detected in the patient. What medicine should be removed from her therapy scheme?
29. A 35-year-old woman had acute onset of the disease that started with fever up to 39.0°C and cough. 3 days later her dyspnea at rest increased up to 35/min. Downward from her right shoulder-blade angle, percussion detects a dull sound. No vocal fremitus, respiratory sounds cannot be auscultated. What is the treatment tactics?
30. After playing with ’’mosaics’ : a 2- year-old child suddenly developed cough, stridorous respirations, urges to vomit, and cyanosis against the background of relative somatic health. What should the doctor suspect first when examining this child?
31. 40% of the workers, who polish the art glass, using an abrasive disk, and have a long record of employment, are diagnosed with ulnar neuritis, 21% - with vegetative polyneuritis, and 12% - with vegetomyofascitis of the upper limbs. These pathologies are associated with the following harmful factor:
32. After a long drive with the window open a man developed a facial asymmetry; he cannot close his right eye, his right nasolabial fold is smoothed out, movements of expression are absent on the right, there is a disturbance of taste sensation in the tongue on the right. No other neurological abnormalities were detected. What disease can be provisionally diagnosed in this case?
33. A 6-year-old girl complains of body temperature up to 39°C, rhinitis, dry cough, dyspnea. She has been presenting with these signs for 5 days already On examination her condition is of moderate severity Her dyspnea is of mixed genesis. Respirations are 28/min., pulse is 120/min. Percussion produces a dull sound in the right lower segments; in the same area auscultation detects weakened respiration and fine vesicular wet crackles; coarse respiration can be detected on the left. Make the provisional diagnosis:
34. A full-term newborn (born with the body weight of 3900 g at gestational age of 39 weeks) on the first day of his life developed respiratory disturbances: dyspnea, arrhythmic respiration, cyanosis attacks. On examination there is* paradoxical respiration observed and left side of the chest lags behind in the act of breathing. On auscultation the respiration is weakened in the lungs on the left. Neurologist diagnosed the patient with leftsided Erb-Duchenne palsy Complete blood count shows no changes. What is the most likely diagnosis?
35. A 30-year-old woman made an appointment with the family doctor for scheduled vaccination of her 2-year-old child. What type of healthcare provides such medical services?
Explanation
According to levels of specialization, types of medical care include: Emergency, Primary, Secondary, Tertiary, palliative, medical rehabilitation and dentistry.
Primary medical care: involves care given by nurses, midwives, general physicians, family doctors, in polyclinics etc. One major aspect of primary health care is preventive medicine - these include vaccination, teaching on methods for good living etc.
Secondary medical care: When your primary care provider refers you to a specialist, you are then in secondary care. Secondary care simply means you will be taken care of by someone who has more specific expertise eg cardiologist, endocrinologist etc
Tertiary Medical Care: Once a patient is hospitalized and needs a higher level of specialty care within the hospital, he may be referred to tertiary care. Tertiary care requires highly specialized equipment and expertise. 36. A 3-year-old child has been brought to a hospital with complaints of pain in the legs, fever, and loss of appetite. Objectively: pale skin and mucosa, hemorrhagic rash. Lymph nodes are enlarged, painless, dense and elastic, not matted together. Bones, joints, and abdomen are painful. The liver and spleen are enlarged. Hemogram: Hb- 88 g/L, color index -1.3, platelets - 80 . 109 /L, leukocytes - 25.8 • 109 /L, lymphoblasts -70%, ESR- 52 mm/hour. Make the provisional diagnosis:
37. After semolina was introduced into the diet, a 1-year-old child for 2 months has been presenting with loss of appetite, irritability loss of body mass, and loss of previously learned skills. The feces are copious and foul-smelling. The skin is pale and dry, the hair is brittle. The abdomen is distended, while the limbs are thin. Stool test shows high levels of fatty acids. What is the most likely diagnosis?
Explanation
Notice that these symptoms begin to take place after the introduction of Semolina; a food product rich in gluten. Celiac disease, also referred to as celiac sprue or nontropical sprue, is a common condition characterized by a maladaptive immune response to gluten, a protein found in many grains (e.g., wheat). The underlying pathophysiology is believed to be a combination of gluten intolerance, which triggers an autoimmune reaction, and production of autoantibodies that target tissue transglutaminase, specifically within the proximal small intestine. Typical findings include changes in bowel habits and symptoms associated with malabsorption (e.g., fatigue, weight loss, vitamin deficiencies).
Irritable bowel syndrome is a functional disorder that affects mainly the large intestine and is characterized by bloating, abdominal cramps, diarrhea etc
Mucoviscidosis refers to cystic fibrosis of the pancreas.
38. A 73-year-old woman came to the family physician for one of her regular follow-up examinations. Three months ago she was found to have type 2 diabetes mellitus. She was keeping to her diet and exercise plan and taking phytopreparations. On examination her fasting glucose was within the range of 78-8.6 mmol/L, HbAlc _ 79%. Height - 164 cm, weight - 83 kg. What blood glucose-controlling medicine should she be prescribed first in the course of her pharmacological therapy?
39. A patient, has gradually lost his consciousness. The skin is pale and dry There is smell of ammonia from the mouth. Respirations are deep and noisy Heart sounds are muffled, pericardial friction rub is present. Blood pressure is 180/130 mm Hg. Blood test: Hb- 80 g/L, leukocytes - 12 ■ 109 /L, blood glucose - 6.4 mmol/L, urea -50 mmol/L, creatinine - 1200 mcmol/L, blood osmolarity - 350 mOsmol/kg H2O. No urinary excretion. Make the diagnosis:
40. A 10-year-old boy came to the polyclinic with complaints of stuffy nose. It is known that these signs occur in the child periodically (in spring and autumn). He has a history of atopic dermatitis. The father of the child has bronchial asthma. Objectively the boy’s face is pale and slightly swollen. Respirations are 22/min. Auscultation detects vesicular respiration over the lungs. Rhinoscopy shows swollen and pale nasal mucosa. What disease can be suspected?
41. Disease onset was acute. A child developed general weakness, pain in the joints, and fever Later these signs became accompanied by itching skin rash manifested as erythematous spots 2-5 mm in size. The rash gradually turned hemorrhagic. Large joints are painful and swollen; pain attacks periodically occur in the paraumbilical area; there are signs of intestinal hemorrhage. What is the most likely diagnosis?
42. A 34-year-old multipara was brought to the labor ward with regular labor activity. Her pelvic size is 26-29-32-22 cm. Vaginal examination shows 6 cm cervical dilation, the amniotic sac is unbroken. The fetus is in the breech presentation, with buttocks pressed to the entrance into the lesser pelvis. The promontory cannot be reached, no exostoses. Fetal heart rate is 140/min., expected fetal weight is 2800 g. What labor tactics should be chosen?
43. A 54-year-old woman complains of a fogged vision in her right eye, rainbow circles in her vision, headache, and nausea. Within the last month she twice experienced a similar condition, but back then all the signs eventually disappeared and her sight was restored. Currently all the signs have been persisting for over 2 days. Objectively the patient has eyelid edema, congestive injection of the eyeball, corneal opacity shallow anterior chamber of the eye, and dilated pupil that is unresponsive to the light. Her intraocular pressure is 48 mm Hg. Make the diagnosis:,
44. A 3-month-old child with signs of rickets presents with positive Chvostek, Trousseau, and Maslov signs. One day ago the parents witnessed a cyanotic attack in their child - the child broke into a cold sweat, the eyes bulged, and respiratory arrest occurred. One minute later the child drew in a loud breath and the child’s condition normalized again. What is the cause of the described signs of the disease?
45. After eating shrimps, a 25-year-old man suddenly developed skin itching, some areas of his skin became hyperemic or erupted into vesicles. Make the diagnosis:
46. A 35-year-old woman came to the family doctor with complaints of profuse menstruations that last up to 10 days. Gynecological examination shows that the uterine cervix is without changes, the uterus is in anterflexio, has normal size, is mobile and painless. The uterine appendages on the both sides are without peculiarities. The family doctor made the provisional\' diagnosis of abnormal uterine bleeding. What instrumental method of examination needs to be performed first to diagnose this pathology?
47. A 19-year-old young man was diving and hit his head on the bottom of the pool. He complains of pain in the neck, his head movements are limited and painful. During examination his head is bowed forward and to the right and the patient supports it with his hands. Palpation detects tense neck muscles and protruding spinous process of the IV cervical vertebra (C4). When pressure is applied to this process and to the head (axial load), the pain intensifies. Make the provisional diagnosis:
48. A patient is 45 years old. He was referred for a consultation with a psychiatrist due to complaints of abdominal pain and discomfort that occur in emotionally straining situations. Objectively no changes of the gastrointestinal tract were detected. The complaints emerged over 10 years ago against the background of severe alcohol poisoning. The patient has been repeatedly visiting gastroenterologists, who were unable to find any significant changes in the patient. The prescribed therapy was* ineffective. What is the likely conclusion?
Explanation
In Somatoform Autonomic dysfunction, the symptoms are presented by the patient as if they were due to a physical disorder of a system or organ that is largely or completely under autonomic innervation and control, i.e. the cardiovascular, gastrointestinal, respiratory, and urogenital systems. Clinical and instrumental examination revealed no organic alterations in any system therefore indicating a somatoform autonomic dysfunction.
Organic brain syndrome is defined as a state of diffuse cerebral dysfunction associated with a disturbance in consciousness, cognition, mood, affect, and behavior in the absence of drugs, infection, or a metabolic cause
49. A 21-year-old man was hospitalized on the 2nd day of the disease. His general condition is severe, body temperature is 39°(7, On his skin there are numerous irregular-shaped hemorrhagic elements. The diagnosis of meningococcemia was made. The next day his body temperature suddenly decreased, blood pressure was 80/40 mm Hg, pulse was 120/min. Acrocyanosis was detected. What complication did the patient develop?
50. Forensic autopsy of the body of a 59-year-old man, who died suddenly at home without signs of violent death, shows pink skin and mucosa, liquid bright-red blood, and bright-red plethoric internal organs. Forensic toxicology testing detected 1.44°/00 of ethanol in the blood and carboxyhemoglobin levels of 55%. What is the cause of death?
51. A 45-year-old man with a history of myocardial infarction developed a brief attack of palpitations, accompanied by the sensations of lack of air, fear, and vertigo. His blood pressure is 90/60 mm Hg. ECG during the attack shows extended QRS complex (0.13 seconds) with heart rate of 160/min., discordant shift of ST segment and T wave, dissociation of atrial and ventricular rhythm. What disturbance of cardiac rhythm is it?
52. For 20 years the role of excessive weight in ischemic heart disease development among the working age male population over 40 was studied. It was determined that overweight men developed ischemic heart disease more often. What type of epidemiological study is it?
53. A 20-year-old woman complains of headaches, vertigo, tearfulness, vomiting, pain in the area of the heart, and tachycardia. The signs appear 6-7 days before menstruation and disappear in the first days of menstruation. Make the diagnosis:
Explanation
Premenstrual syndrome refers to a group of symptoms women experience a week or two weeks before menstruation. These symptoms may include; mood swings, abdominal pain , headaches, vomiting, vertigo, insomnia, changes in appetite and sex drive etc. Commonly prescribed medications for its management include; antidepressants, contraceptives, NSAIDs etc.
Polycystic ovarian syndrome is a disorder found in women of reproductive age commonly due to hormonal disorder (high level of androgens). This disorder is characterised by infrequent menstrual cycle, pelvic pain, weight gain etc. The ovaries mostly develop follicles (collection of fluids).
Algodysmennhorhea is characterised by painful menstruation or menstrual cramps.
54. A woman came to the gynecologist to plan her pregnancy She was advised to increase her intake of the products rich in folic acid, particularly soy beans, bread made of coarsely ground flour, fruits, leafy green vegetables. Such changes in her diet will work toward the prevention of:
55. A 48-year-old woman complains of disturbed menstrual cycle: her periods last for 7-9 days and are excessively profuse throughout the last half-year. She notes occasional hot flashes in her head, insomnia, irritability and headaches. Her skin is of normal color. Blood pressure _ 150/90 mm Hg, pulse - 90/min., rhythmic. The abdomen is soft and painless. Bimanual examination shows no uterine enlargement, the appendages cannot be detected. The vaginal fornices are free. What is the most likely diagnosis?
Explanation
Cimacteric syndrome is seen in women in Perimenopausal or postmenopausal age; they experience a decrease in ovarian function and decrease in female haormones. Climacteric syndrome is defined as gradual changes of ovarian function that start before menopause. Notable signs include; insomnia, dizziness, anxiousness and nervousness, poor sleep quality, hot flashes etc,
Polycystic ovarian syndrome is a disorder found in women of reproductive age commonly due to hormonal disorder (high level of androgens). This disorder is characterised by infrequent menstrual cycle, pelvic pain, weight gain etc. The ovaries mostly develop follicles (collection of fluids).
Premenstrual syndrome refers to a group of symptoms women experience a week or two weeks before menstruation. These symptoms may include; mood swings, abdominal pain , headaches, vomitting, vertigo, insomnia, changes in appetite and sex drive etc.
Adrenogenital syndrome is also known as congenital adrenal hyperplasia.
56. A pregnant woman at 34 weeks of gestation underwent dopplerometry of umbilical circulation, which revealed a reverse diastolic component. Objectively the height of the uterus is 27 cm above the pubic bone, the head of the fetus is mobile and located above the entrance to the lesser pelvis. Fetal heartbeat is 136/min. Vaginal examination shows that the uterine cervix is closed, its length is 3 cm. What tactics should the obstetrician choose?
57. A 26-year-old woman was hospitalized into the gynecological department with complaints of body temperature up to 38.2°C, fever, general weakness, and dirty- red blood discharge from her genital tracts. She is hemodynamically stable. Two days ago she underwent a medical abortion on the 8th week of pregnancy Ultrasound detects the remains of the fertilized egg in her uterine cavity What are the tactics of the patient management in this case?
58. A 23-year-old woman with type 1 diabetes mellitus during the 2nd week of community-acquired pneumonia developed 筹 nausea and vomiting. In the evening she has lost her consciousness and was hospitalized. Objectively the patient\'s skin is pale and dry Her respiration is loud, the tongue is dry with brown deposit. Her heart rate is 129/min., blood pressure is 85/50 mm Hg. Palpation of the patients abdomen provokes no response. The liver is +3 cm. Acetone test is markedly positive, blood glucose is 26 mmol/L. Make the provisional diagnosis:
59. On the 5th day after giving birth a postparturient woman complains of a pain in her left mammary gland and body temperature up to 38.1°(7. Examination shows that her mammary gland is enlarged and painful on palpation, the nipple is edematous and has fissures, the upper external quadrant of the gland is hyperemic. Name the measures that would have prevented the development of this complication in the patient:
Explanation
Mastitis is inflammation of the breast tissue and can be broken down into lactational and non-lactational mastitis. Lactational mastitis is the most common form of mastitis. Lactational mastitis, also known as puerperal mastitis, is typically due to prolonged engorgement of milk ducts, with infectious components from the entry of bacteria through skin breaks. Patients can develop a focal area of erythema, pain, and swelling, and can have associated systemic symptoms, including fever. This occurs most commonly in the first six weeks of breastfeeding but can occur at any time during lactation, with most cases falling off after 3 months. Lactational mastitis is most commonly caused by bacteria that colonize the skin, with Staphylococcus aureus being the most common, in this case an antibiotic may be administered to fight the infection.
The first line of treatment is self-help remedies, such as ensuring that the breast is drained properly during feeds by breastfeeding regularly or expressing the milk. And after a feed, gently express any leftover milk.
Every newborn should be fed on demand. No schedule should be followed. Whenever the baby wants the milk, breastfeeding should be allowed. Breastfeeding should not be stopped because of cracks or pain in the breast.
60. On ultrasound of the thyroid gland, a 47-year-old woman presents with a hypoechoic node 1.6 cm in diameter with blurred margins and intranodular hypervascularization. The doctor suspects thyroid carcinoma. What method should be used to verify the diagnosis?
61. In a pediatric clinic, located in a rural area, there are 9 children, who simultaneously fell ill. The following signs were detected: low physical activity, acrocyanosis of the nasolabial triangle and fingertips, mucosal cyanosis, tachycardia, dyspnea. It was determined that all the sick children were fed with a formula that was dissolved in the water taken from a dug well. Laboratory analysis revealed high levels of methemoglobin in the blood of the children. These signs can be caused by increased content of a certain element in the water. Name this element:
62. A 20-year-old man suffers from headache,。general weakness, and face edema that appears in the morning. 18 days earlier he had a case of tonsillitis. Objectively his skin is pale, there are edema under his eyes. Heart rate is 60/min., blood pressure is 185/100 mm Hg, The sign of costovertebral angle tenderness (punch sign in the lumbar region) is negative. Urinalysis: color of ’’meat slops? protein - 4.5 g/L, altered erythrocytes - 40-45 in the vision field, leukocytes - 5-6 in the vision field. 24- hour diuresis is 400 mL. What is the most likely diagnosis?
63. An 18-year-old patient always obeys others and adapts his needs to the demands of the people on whom he depends. He excessively defers to their wishes and makes them responsible for his wellbeing, cannot defend his interests and needs support from other people. Such psychic profile has been formed in the childhood, remains unchanged, and hinders adaptation. What psychic disorder is observed, in this patient?
64. A 35-year-old woman complains of a pain in her right axillary region. She has been suffering from this condition for a week. Her body temperature is 38°C. In the right axillary region there are 2 formations, 2r cm in size each. The skin over the formations is dark red and thin. Palpation produces a yellow-white discharge from the fistular openings. What is the most likely diagnosis?
65. During a regular examination, an 8- year-old girl with type I diabetes mellitus presents with a swelling on the anterior surface of her hip. The swelling is 3 cm in diameter; dense, painless on palpation. The skin over this formation has normal color and temperature. Localization of the swelling matches the place where the girl usually receives her insulin injections. What is the most likely cause of this clinical presentation?
Explanation
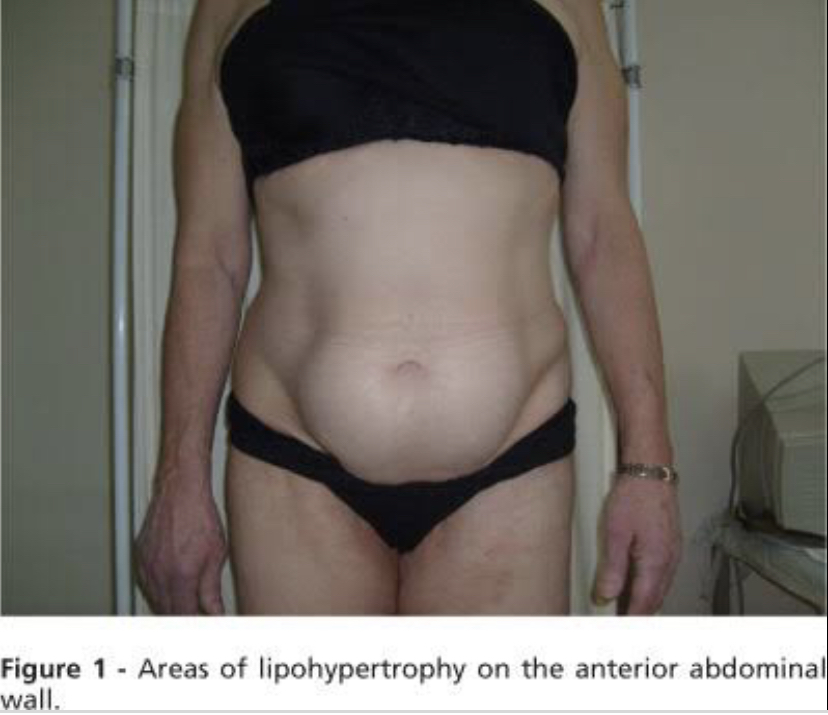

The background information here is that - this young lady with Type I Diabetes Mellitus presents with a 3cm swelling on the anterior surface of the hip.
Abnormal reaction in subcutaneous fat to insulin is called lipodystrophy which can be either hypertrophic or atrophic. Lipodystrophy is an exclusive complication of lean children and young Type 1 diabetic, although rarely can be seen in Type 2 diabetic.
Insulin lipohypertrophy denotes a benign tumor like swelling of fatty tissue at the injection site secondary to lipogenic effect of insulin, whereas lipoatrophy is considered an adverse immunological side effect of insulin therapy. Since the advent of recombinant human insulin and analogue, lipoatrophy, has virtually disappeared, whereas, lipohypertrophy still remains a serious local problem of insulin therapy.
With a swelling of 3cm, the best answer choice is development of hypertrophic lipodystrophy. Atrophic lipodystrophy will not have associated swelling, instead a depression should be observed.
Prevention, to avoid lipodystrophy, should take first place as there is little cure to it, and the best way is to educate the patient about rotating injection sites.
66. A 52-year-old woman has been suffering for 2 years from dull, occasionally exacerbating pain in her right subcostal area, occurring after eating high-fat foods, bitter taste in her mouth in the morning, constipations, and flatulence. Objectively she is obese, her body temperature is 36.9°C; there is a coating on the root of her tongue; the abdomen is moderately distended and painful in the area of gallbladder projection. What examination would be the most helpful for diagnosis making? ,
67. A family doctor performed an external obsterical examination of a pregnant woman and determined that her uterine fundus is located at the level of the navel. What is the most likely term of pregnancy in this woman?
68. What should be prescribed as secondary prevention drugs for a patient with atrial fibrillation after an ischemic stroke caused by cardiac embolism?
69. A 55-year-old woman complains of thyroid gland enlargement that can be observed throughouth the last 2 years and a discomfort during swallowing. Objectively she has signs of hypothyroidism. The thyroid gland on palpation is dense, nonfused with the surrounding tissues and mobile on swallowing. The regional lymph nodes are not enlarged. In the serum there are antithyroid antibodies detected. What is the most likely diagnosis?
70. A 12-year-old girl after a case of respiratory infection developed dyspnea at rest, paleness of skin. Heart rate is 110/min., BP is 90/55 mm Hg. Heart sounds are muffled. Borders of relative heart dullness: right - the parasternal line, upper - the III rib, left - 1,0 cm outwards from the midclavicular line. Make the provisional diagnosis:
71. A 19-year-old young man complains of cough with expectoration of purulent sputum in amount of 100 mL per day, hemoptysis, dyspnea, increased body temperature up to 37.8°C, general weakness, weight loss. The patient\'s condition lasts for 4 years. Exacerbations occur 2-3 times a year. The patient presents with malnutrition, pale skin, cyanosis of the lips, drumstick (clubbed) fingers. Tympanic percussion sound in the lungs, weakened respiration, and various numerous moist crackles in the lower pulmonary segments on the left can be observed in this patient. In blood: erythrocytes - 3.2 • 1012 /L leukocytes -8.4 • 109 /L,ESR- 56 mm/hour. On X- ray: lung fields are emphysematous, the left pulmonary root is deformed and dilated. What is the most likely diagnosis?
72. A patient 1 year ago had a Q wave myocardial infarction of the posterior wall of the left ventricle. For the last 2 weeks he has been suffering from daily attacks of atrial fibrillation and bradycardia episodes, accompanied by bouts of vertigo. What tactics is the most advisable in this case?
73. A 58-year-old woman has type 2 diabetes mellitus that is compensated with diet and metformin. She prepares for cholecystectomy. Objectively: her height is 164 cm, weight is 90 kg, heart rate is 72/min., blood pressure is 130/80 mm Hg. Her abdomen is soft, painful in the right subcostal region. The liver is not enlarged. Fasting glucose - 6.2 mmol/L. Glycated hemoglobin - 6.5%. What further tactics of sugar-lowering therapy should be chosen in this case?
74. A 23-year-old woman came to the gynecological clinic. She complains of pain, itching, and burning in her vulva, general weakness, indisposition, elevated body temperature up to 31.2°C, and headache. On examination in the vulva there are multiple vesicles up to 2-3 mm in diameter with clear contents against the background of hyperemia and mucosal edema. Make the provisional diagnosis:
75. A 5-year-old child had acute onset of the disease that manifested in body temperature up to 39.5°C, marked chills,, weakness, inertness, skin pallor, and headache. 8 hours later a hemorrhagic rash developed on the skin of the buttocks and legs. The child is sluggish, the body temperature has dropped, blood pressure is 80/40 mm Hg, respirations are 28-30/min., diuresis is decreased. Make the provisional diagnosis:
Explanation
Meningococcemia is defined as dissemination/spread of meningococci (Neisseria meningitidis) into the bloodstream. Patients with acute meningococcemia may present with (1) meningitis (2) meningitis with meningococcemia, or (3) meningococcemia without clinically apparent meningitis. This patient appears to have the third presentation, Clinical presentation include; petechial/hemorrhagic skin rash usually located on the trunk and legs and may rapidly evolve into purpura, malaise, weakness, myalgias, headache, nausea, vomiting, and arthralgias.
Henoch-schonlein purpura ( hemorrhagic/ IgA vasculitis) is a condition in which small blood vessels are inflamed. It is an acute immune complex-mediated small vessel vasculitis that most commonly occurs in children. typically presents with a tetrad of symptoms: palpable purpura, arthritis/arthralgia, abdominal pain, and renal disease; although not all patients show the complete four symptoms.
Thrombotic thrombocytopenic purpura (TTP) is a thrombotic microangiopathy, a condition in which microthrombi, consisting primarily of platelets, form and occlude the microvasculature (i.e., the arterioles and capillaries).
76. A 75-year-old man in a severe condition suffers from dyspnea at rest, marked weakness, and arrhythmia. Abdominal aortic pulsation is observed, further on there is a systolic murmur detected. Palpation reveals a volumetric formation in the mesogastrium. Blood pressure is 70/40 mm Hg. There is no pulsation over the femoral arteries. Oliguria is detected. Which diagnosis is the correct one?
77. When planning treatment of a patient, it was decided to use a medicine with evidence level A. What trials produce the evidence that allows to classify the medicine as level A?
Explanation
As the name suggests, evidence-based medicine (EBM), is about finding evidence and using that evidence to make clinical decisions. A cornerstone of EBM is the hierarchical system of classifying evidence. This hierarchy is known as the levels of evidence.
Randomized Clinical or Controlled Trials: Include a randomized group of patients in an experimental group and a control group. These groups are followed up for the variables/outcomes of interest. Randomized controlled trials (RCTs) are considered the gold standard in modern medicine for determining the efficacy of a treatment. Individual RCTs are level 1b evidence. Systematic reviews of homogenous RCTs are regarded as the highest level of evidence—level 1a. These systematic reviews consist of information synthesized from individual, well-designed RCTs where participants are similar and have equal chances of being assigned to an intervention group, a control group, or a placebo group.
|
Grade of
Recommendation
|
Level of
Evidence
|
Type of Study
|
|
A
|
1a
|
Systematic review of (homogeneous) randomized
controlled trials
|
|
A
|
1b
|
Individual randomized controlled trials (with narrow
confidence intervals)
|
|
B
|
2a
|
Systematic review of (homogeneous) cohort studies
of "exposed" and "unexposed" subjects
|
|
B
|
2b
|
Individual cohort study / low-quality randomized
control studies
|
|
B
|
3a
|
Systematic review of (homogeneous) case-control studies
|
|
B
|
3b
|
Individual case-control studies
|
|
C
|
4
|
Case series, low-quality cohort or case-control studies
|
|
D
|
5
|
Expert opinions based on non-systematic reviews of
results or mechanistic studies
|
Two things to remember:
1. Studies in which randomization occurs represent a higher level of evidence than those in which subject selection is not random.
2. Controlled studies carry a higher level of evidence than those in which control groups are not used.
Expert Consensus - Level D
Case Control studies - Level B
78. After the pregnant woman’s waters broke, it was noted that they are significantly contaminated with meconium. Upon birth, the baby is not breathing, remains inert, the skin is cyanotic and covered in meconium, heart rate is 98/min. What resuscitation measures should be taken after the baby is born?
79. The 5-year-old child has been ill for 2 weeks. Cough attacks developed first and were then followed by reprises. During coughing the child’s face turns red and cervical veins bulge. The cough attacks induce vomiting. X-ray shows intensified bronchial pattern. Blood test: leukocytes - 16.109 /L , lymphocytes - 72%, erythrocyte sedimentation rate - 4 mm/hour. What is the most likely diagnosis?
80. A 48-year-old woman was delivered into the surgical unit with wounds in her thigh. On examination the wound surface has a dirty-gray coating with unpleasant sweet smell. The wound content resembles a raspberry jelly. Skin tissues around the wound are glossy and turgid. palpation reveals moderate crepitation in the tissues. What bacteria is most likely to cause such inflammation?
81. A patient underwent suture plication of the perforated duodenal ulcer. On the 3rd day after the operation he started producing a large amount of discharge from the abdominal drain tube. The discharge contains bile and has high amylase levels. What complication occurred in the patient?
Explanation
At the end of the operation (suture plication), a drainage tube is inserted into the abdomen for two purposes: firstly, the detection of any fluid collections within the abdomen (intra‐abdominal collections), usually resulting from intestinal secretions; and secondly, as the treatment of intra‐abdominal collections, so that fluid collection decreases or, at least, does not worsen within the abdomen. The fluids from the drain can be tested for enzymes like amylase (one of the contents of the pancreatic juice which digests carbohydrates), bile secretions or intestinal juice to find out whether the fluid in the drain is because of a suture leak. A case of suture leaks often presents as a sequelae to suture incompetence.
If there is a high suspicion of a pancreatic/bile leak (as seen in this patient), further scans are performed to confirm it or to rule it out. If the leak is major and the patient is unwell, urgent reoperation may be required.
82. A 40-year-old victim of a traffic accident sustained the following injuries: closed diaphyseal femur fracture, brain concussion, multiple rib fractures, hemopneumothorax, degloving skin injuries. What injuries require the most urgent attention?
Explanation
In resuscitating a patient, C-A-B sequence is very important.
C is to help maintain blood circulation; A - airway and B - Breathing.
Hemopneumothorax can be considered under these 3.
Hemo - active internal hemorrhage into the pleural cavity.
Pneumo - ongoing air leakage into the pleural cavity (rib fractures).
If these are not attended to first, eventually, the lungs will not be able to expand, hence, no gaseous exchange compromising both A- airway and B- breathing. If no action is taken, and the hemorrhage and air leakage into the pleural cavity continues, it will eventually lead to hypovolemia and the accumulated blood will compress the mediastinum which houses the heart thereby preventing the heart from contracting as well and eventually compromises C- circulation. Once this is attended to, the other injuries can receive proper care as well but hemopneumothorax comes first.
Now, considering this patient, there is no active external bleeding going on. Closed diaphyseal femur fracture just needs immobilization as first aid. It is not open and the question did not state that there is an injury to a major blood vessel. In Degloving shin injuries, if there is an active bleeding, the vessel can be ligated and the wound dressed.
The most common and least serious type of traumatic brain injury is called a concussion. A concussion is most often caused by a sudden direct blow or bump to the head.
83. A 20-year-old woman, gravida 2, para 1 has been in labor for 4 hours. Her condition is satisfactory Moderately painful contractions occur every 3 minutes and last for 35-40 seconds. The waters have not burst yet. The fetus is in longitudinal position. Fetal heartbeats are 136/min., clear and rhythmic. Major segment of the fetal head is engaged to the pelvic inlet. Vaginal examination shows smooth cervix of 6 cm, amniotic sac is intact, sagittal suture is in the left oblique diameter, occipital fontanel is on the right near the symphysis pubis. What stage of the labor is it?
84. A 22-day-old infant developed subcutaneous red nodes from 1.0 to 1.5 cm in size on the scalp; later the nodes suppurated. lemperature increased up to 377°C, intoxication symptoms appeared, regional lymph nodes enlarged. Complete blood count: anemia, leukocytosis, neutrocytosis, raised ESR. What diagnosis will you make?
85. A 26-year-old man complains of chills, rhinitis, dry cough, and fever up to 38°C. Examination shows him to be in a moderately severe condition; there are small pale pink non-merging spots on the skin of his back, abdomen, and extremities. Palpation reveals enlarged occipital and axillary lymph nodes. No information about vaccination history could be obtained. What is the likely etiology of this disease?
Explanation
Rubella ( accused by rubella virus) is an acute viral infection characterised by a short prodromal period, Exanthema ( rash) during three days and lymphadenopathy. The type of rash found is roseola and small macula-papula. Note that the rash elements do not merge ( non-merging spots) and are usually concentrated on the extensor surface of extremities, back, buttocks and outer surface of thigh.
Epstein-barr virus is one of the causative agents of Infectious mononucleosis- a disease characterised by prolonged fever, systemic lymphadenopathy, acute tonsillitis, acute adenoiditis, hepatosplenomegaly, along with typical blood changes such as lymphocytosis, monocytosis, presence of specific cells called atypical mononuclear cells or virocytes.
Mumps infection is a systemic disease characterised by hyperthermic syndrome, symmetrical or unilateral swelling of parotid glands, epididymo-orchitis etc
86. A 38-year-old patient has been delivered by an ambulance to a surgical department with complaints of general weakness, indisposition, black stool. On examination the patient is pale, there are dotted hemorrhages on the skin of his torso and extremities. On digital investigation there are black feces on the glove. Blood test: Hb-108 g/L, thrombocytopenia. Anamnesis states that similar condition was observed 1 year ago. Make the diagnosis:
87. The body of a citizen was found at the place of his dwelling. On his face, neck, and hands there were detected irregular-shaped wounds, varying from 2x3 cm to 4x5 cm in size. The skin and underlying tissues are absent in the wounds. The margins of the wounds are uneven, with major and minor scalloping along the edges and no signs of bleeding. What is the initiating mechanism of these wounds?
88. A multigravida, labor II, 36-37 weeks of gestation, has gone into labor Her waters broke 8 hours ago, the labor activity continues for the last 4 hours, it is regular, with contractions that last 35 seconds and occur every 3-4. minutes. The child is in the cephalic presentation, with the head pressed to the entrance into the lesser pelvis. The parturient woman complains of a sudden sharp abdominal pain. Her pulse is 100/min., blood pressure is 110/70 - 100/70 mm Hg. The uterus is tense and does not relax between the contractions. Fetal heartbeat is muffled - 100/min. The amniotic fluid is blood-colored and continues to leak. What is the most likely diagnosis?
89. A 45-year-old woman complains of increasing body weight throughout the last year. Examination revealed moon face syndrome, brittle hair; hirsutism, stretch marks on the abdomen, and disproportionally thin limbs. The patients height is 162 cm, her body weight is 94 kg, her body mass index is 35.8 kg/m2 . What type of obesity is it?
90. A 2.5-year-old child is ill for the second day The onset of the disease was associated with the temperature up to 378°C, a single bout of vomiting, and watery diarrhea up to 5 times per day During the second day vomiting occurred twice, body temperature is 38.0°C, the child has low appetite, watery diarrhea continues. .The treatment of the child should start with the following:
91. On the 3rd day after the artificial abortion the woman was hospitalized into the gynecological department in a severe condition with signs of intoxication, abdominal pain, and purulent discharge from the vagina. Objectively the patients condition is severe, her body temperature is 38.8°C, pulse is 100/min., blood pressure is 110/70 mm Hg? the uterus is soft, the uterine fundus is located at the level of the navel, there are positive signs of peritoneal irritation. What is the most likely diagnosis?
92. You witnessed a car accident. When examining the place of the accident you noticed a man of about 30 years, who was hit by the car. He is unconscious. On his neck on the left there is a profuse hemorrhage with bright-red blood. How to stop this hemorrhage? 1
93. A 27-year-old man complains of pain in his leg joints, purulent discharge from the eyes, and painful burning sensations during urination. The disease onset was acute. He has a history of influenza. The patient smokes and drinks alcohol in excess. In his line of work he is often away on business trips. What is the most likely etiological factor of this disease?
94. A 57-year-old man, a miner, complains of a pain in his chest, dyspnea on physical exertion, excessive sweating, constant subfebrile tempeature, and cough that produces blood-streaked sputum. He has been smoking for approximately 40 years (2 packs a day) and frequently has ’’pneumonias? Survey chest X-ray shows a triangular shadow in the middle lobe of the right lung. One of the apices of the shadow points to the lung root. Cardiac and mediastinal shadows are displaced toward the affected area. Make the provisional diagnosis:
95. A district doctor has diagnosed one of his patients with dysentery. What accounting document reflects this type of morbidity?
96. A 31-year-old drug-addicted person complains of a cough with bloody expectorations, dyspnea, persistent fever, and leg edemas. The jugular veins are distended. There is a coarse pansystolic murmur detected above the base of the xiphoid process and in the second intercostal space on the left, close to the edge of the sternum. Heart sounds are clear; arrhythmia is detected, heart rate is 128/min” pulse - 82/min., blood pressure is 100/70 mm Hg. What is the most likely diagnosis?
97. A 7-year-old boy after a fall from a height presents with rapid and shallow breathing and cyanotic face. The right half of his thorax is distended and takes no part in the respiration. Percussion detects tympanitis in the affected area, while auscultation detects no breathing there. What pathology is the most likely cause of this clinical presentation? What instrumental examination would be the most informative in this case?
98. A 55-year-old woman came to a gynecologist with complaints of leukorrhea and bloody discharge from the vagina after • 5 years of menopause. Anamnesis states no pregnancies. Bimanual examination: the uterus and uterine appendages are without changes. During diagnostic curettage of the uterine cavity the physician scraped off a sample of enchephaloid matter What is the most likely diagnosis in this case?
99. What modern organizational method can provide the patients in the remote settlements with timely access to quality medical aid and such medical services as consulting, diagnostics, and treatment, especially in the situations when time and distance are crucial?
100. A 17-year-old girl has been suffering from hepatic cirrhosis for 3 years. Lately her periods of excitation have been intermittent with depression, she does not sleep enough. Objectively her condition is severe, the girl is sluggish, gives one-word responses, has tremor in her extremities, her skin is icteric, with single hemorrhagic rashes. Name the likely complication of her disease:
101. A man works in casting of nonferrous metals and alloys for 12 years. In the air of working area there was registered high content of heavy metals, carbon monoxide, and nitrogen. During periodic health examination the patient presents with asthenovegetative syndrome, sharp abdominal pains, constipations, pain in the hepatic area. In urine: aminolevulinic acid and coproporphyrin are detected. In blood: reticulocytosis, low hemoglobin level. Such intoxication is caused by:
102. During regular examination of a 2- year-old boy he presents with enlarged left kidney painless on palpation. The right kidney was undetectable on palpation. Excretory urography shows no contrast on the right. Cytoscopy detected hemiatrophy of the urinary bladder trigone, the right ureteral orifice is not detected. What pathology is it?
103. A 34-year-old woman after rapidly changing her position from horizontal to vertical suddenly paled, fell down, her skin became moist, her limbs are cold, her pupils are dilated. The pulse is rapid and thready blood pressure is 50/25 mm Hg. What condition has likely developed in the patient?
104. On laboratory investigation of a pork sample there is 1 dead trichinella detected in 24 sections. This meat should be:
105. Employees work in conditions of high dust concentration. Certain chemical (silicon dioxide content) and physical properties of dust aerosols contribute to the development of occupational dust-induced diseases. What is the main physical property of dust aerosols?
106. A woman complains of a severe pain in her throat on the left, difficult swallowing and mouth opening, elevated body temperature, and general malaise. The onset of the disease was 4 days ago after a case of tonsillitis. Examination detects a trismus of the masticatory muscles, the left tonsil is displaced toward the midline, the anterior palatal arch is infiltrated and protruding. The regional lymph nodes on the right are enlarged and painful on palpation. Make the diagnosis:
107. During winter epidemics of influenza caused predominantly by virus A/California/04/2009 (H1N1), on the 2nd day after the disease onset a 30-year-old hospitalized man presented with high fever, dry cough, myalgia, headache, and general weakness. What should be prescribed as an. etiotropic treatment in this case?
108. A 30-year-old woman complains of itching skin, predominantly in the evening and at night. The condition lasts for 2 weeks already On the skin of the interdigital folds, mammary glands, abdomen, buttocks, and thighs there are numerous fine papular and papulovesicular rashes located in pairs, excoriations. There is no rash on the face and neck. Similar rash is observed in the husband of the patient. What is the most likely diagnosis?
Explanation
Scabies is a parasitic skin infestation caused by the Sarcoptes scabiei. It is characterised by intense pruritus ( itching) at night; this characteristic and the location of the rashes helps us to diagnose scabies. The primary lesion found are usually papules, vesicles or burrows ( accompanied by excoriations and pustules) which are commonly seen in interdigital folds, flexor surfaces of the wrist, axillary folds, buttocks ( closed areas of the body). Additionally in children, elderly persons, and immunosuppressed patients: scalp, face, neck, under the nail, palms of hands, and soles of feet.
Neurodermatitis is also referred to as Lichen simplex chronicus; it is chracterised by chronic itching and scaling localised on the wrist, neck, forearm, legs and anal region.
Epidermophytosis is referred to as ‘Athlete’s foot’. 109. A 20-year-old patient complains of a severe headache, double vision, weakness, fever; irritability Objectively: body temperature is 38.1°(7, the patient is reluctant to contact, sensitive to stimuli. There are ptosis of the left eyelid, exotropia, anisocoria S 〉 D , and pronounced meningeal syndrome. On lumbar puncture the cerebrospinal fluid flowed out under a pressure of 300 mm Hg, the fluid is clear, slightly opalescent. 24 hours later there appeared a fibrin film. Protein - 1.4 g/L, lymphocytes - 600 per mm3 , glucose - 0.3 mmol/L. What is the provisional diagnosis?
110. 3 hours after a trauma, a young man developed bradycardia of 46/min., anisocoria D>S, hemi-hyperreflexia S〉D, hemihypesthesia on the left, and a convulsive disorder The character of this process needs to be clarified. What method of examination will be the most accurate for this purpose?
111. A dweller of the northern Dnieper area, a fisherman, for the last several days has been complaining of a discomfort in his right subcostal region, periodical episodes of diarrhea, intermittent with constipations, frequent skin rashes. Abdominal ultrasound shows enlarged liver and pancreatic head. Make the provisional diagnosis:
112. A 25-year-old woman was brought into the gynecological department with profuse bloody discharge from her genital tracts. She is 12 weeks pregnant, the pregnancy is planned. Within the last 3 days she was experiencing pains in her lower abdomen that eventually started resembling cramps, she developed bleeding. Her skin is pale, pulse - 88/min., blood pressure - 100/60 mm Hg, body temperature - 36.8°C. Vaginal examination: the uterus size corresponds to 11 weeks of gestation, the cervical canal allows inserting 1 finger and contains fragments of the fertilized ovum, the discharge is bloody and profuse. What is the most likely diagnosis?
113. A 39-year-old man, a battery attendant, suddenly developed weakness, loss of appetite, nonlocalized colicky abdominal pains, and nausea. Objectively his skin is gray; there is a pink-gray stripe on his gums; the abdomen is soft and sharply painful. Blood test detected erythrocytes with basophilic stippling and anemia. The patient has a history of peptic ulcer disease of the stomach. Constipations occur each 3-4 days. What is the most likely provisional diagnosis?
114. An 18-year-old patient complains of skin rash. The patient has been suffering from this condition for 5 years. The first instance of this disease occurred after a car accident. Objectively: the patient presents with a papular rash covered in silvery scales, ’’thimble” sign (small pits on the nails), affected joints. What is the most likely diagnosis?
115. During regular medical examination a lyceum student presents with signs of cheilitis that manifests as epithelial maceration in the area of lip seal. The lips are bright-red, with single vertical cracks covered with brown-red scabs. These clinical signs are most likely caused by insufficient content of the following in the diet:
116. Children from a certain township present with brittle teeth, malocclusion, dental enamel erosions, and dental pigmentation that looks like yellow-brown spots. What is the likely cause of this presentation?
117. An 8-day-old boy was delivered to the hospital on the second day after the onset of the disease, His parents complain of his fussiness, regurgitation, body temperature to 38.5°C, red skin with infiltration in lumbar area. His medical history has no peculiarities. The child is in the severe condition, inert, pale, suckles poorly In the lumbar area, on the sacrum and buttocks there is a tense infiltration with hyperemic and cyanotic areas and with a soft spot 8x7 cm in its center. The stool is 10 times in 24 hours, with green and mucous admixtures. What is the most likely diagnosis?
118. A 72-year-old man with pneumonia complains of marked dyspnea, chest pain, severe cough with expectoration, t° is 39.5-40°C, no urination for the last 24 hours. Objectively the patient is conscious. Respiratory rate is 36/min. Percussion sound is dull over the right lower pulmonary lobe; on auscultation there is bronchial respiration and numerous moist crackles. Blood pressure is 80/60 mm Hg, Heart rate is 120/min. Heart sounds are muffled, there is tachycardia. What tactics should the family doctor choose for the management of this patient?
119. A 48-year-old man came to a doctor with complaints of vomiting that brings no relief and a burning pain in his left subcostal region that irradiates to the left lumbar region. These signs appeared after a meal. The Ortner’s and Mayo-Robson’s signs are positive. In the blood: leukocytosis and increased ESR. In the urine: elevated diastase levels. Make the diagnosis:
120. A 32-year-old woman complains of general weakness, low-grade fever persisting for 4 months, lumbar pain, and dysuria. Anamnesis includes frequent acute respiratory diseases, overexposure to cold, low-calorie diet, a case of pulmonary tuberculosis in childhood. Clinical urine analysis: pH- 4.8, leukocyturia, hematuria. Complete blood count: leukocytosis, lymphocytosis, raised ESR. Urography concludes: dilatation of renal pelvis and calyceal system of both kidneys, foci of calcification in the projection of right kidney parenchyma. What is the most likely diagnosis?
121. An unconscious patient was delivered to a hospital by an ambulance. Objectively his body temperature is 39°C, he presents with convulsions and red dry skin. It is known that the patient works as a stoker in the boiler room. What is the likely diagnosis?
122. A child was born at 40 weeks of gestation with the weight of 3700 g. The child’s Apgar score is 7/9. The baby was put to breast immediately after birth and suckled actively. On the 3rd day of life the child’s weight decreased to 3600 g. What transitory condition is observed in this child?
123. 2 hours after eating unknown mushrooms, a 28-year-old man sensed a decrease in his mobility and deterioration of his ability to focus. This condition was then followed by a state of agitation and aggression. On examination he is disoriented and his speech is illegible. 4 hours later he developed fetor hepaticus and lost his consciousness. What syndrome can be observed in this patient?
124. A 17-year-old girl complains of a pain in her knee and ankle joints and body temperature up to 39*C. 2 weeks ago she had a case of acute tonsillitis. Objectively, her joints are swollen, sharply painful, and their mobility is reduced. On the skin of her trunk and limbs there are barely visible circle-shaped pale pink spots. Heart rate is 95/min, blood pressure is 90/60 mm Hg, heart sounds are weakened, there is a soft systolic noise over the apex. Make the provisional diagnosis:
Explanation
Acute rheumatic fever typically occurs 2-3 weeks after Group A streptococcal pharyngitis. Diagnosis depends on a set of clinical signs that result from this infection ( Jones criteria)- these include chorea, carditis, subcutaneous nodules, erythema marginatum, and migratory polyarthritis. For biochemical analysis, certain key markers are used in diagnosis; these include C reactive protein ( an inflammatory marker), antistreptolysin O titer ( a marker that indicates a group A streptococcal infection ), ESR ( a marker from general blood analysis). Using these criterias, we can observe that this patient has arthritis, carditis and results from the biochemical analysis all appear positive for an acute rheumatic fever.
Reactive arthritis is also known as reiter’s syndrome and refers to the inflammation of joints as a result of a urogenital, intestinal or respiratory infection.
125. A 19-year-old girl complains of moderate itching and hair loss on her head. Objectively on the skin of her occipital region there is a single round erythematous focus 3 cm in diameter with clear margins. Asbestos-like scales can be observed on the surface of the lesion. The hair in the focus of the lesion is broken off at the length of 6-8 mm. What is the most likely diagnosis?
126. A woman complains of frequent watery stool (up to 9-10 times per day) with mucus and blood admixtures, dull pain in the hypogastrium, weight loss of 4 kg within the last year. Objectively: malnutrition, dry skin, low turgor, aphthous stomatitis. The abdomen is soft, the sigmoid colon is spastic and painful on palpation. Occult blood test is positive. Fibrocolonoscopy: edema, hyperemia, mucosal granulation, pseudopolyps, small ulcers with irregular edges. Make the diagnosis:
Explanation
-
Distinguishing Ulcerative Colitis from Crohn Disease
|
Ulcerative Colitis
|
Crohn Disease
|
|
Only colon involved
|
Panintestinal
|
|
Continuous inflammation extending proximally
from rectum
|
Skip-lesions with intervening normal mucosa
|
|
Inflammation in mucosa and submucosa only
|
Transmural inflammation
|
|
No granulomas
|
Noncaseating granulomas
|
|
Perinuclear ANCA (pANCA) positive
|
ASCA positive
|
|
Bleeding (common)
|
Bleeding (uncommon)
|
|
Fistulae (rare)
|
Fistulae (common)
|
Cathartic colon
Occult blood in stool is indicative of a hemorrhagic process from the colon, while the results from the colonoscopy indicates the pathology is located in the colon.
Irritable bowel syndrome is an inflammatory bowel disease characterised by recurrent abdominal cramps (pain), change in form (consistency) and frequency of stool, constipation etc. . This condition is common in middle aged women and is associated with underlying conditions such as stress, anxiety, depression or a previous case of intestinal infection.
127. A 9-year-old boy fell off a tree and hit the back of his head. A brief loss of consciousness was observed. The child\'s condition is satisfactory, he has a headache and vertigo. Skull X-ray scans show a depressed fracture of the occipital bone in the area of the external occipital protuberance. What treatment tactics is indicated for this patient?
128. A 16-year-old boy developed dizziness. His heart rate is 35/min, blood pressure is 85/45mmHg. Heart borders are not enlarged. Heart sounds are loud and clear. ECG shows P waves disconnected from QRS complexes, dissociation and different rhythm of the atria and ventricles is accompanied by varying location of P wave in relation to QRST complex. This presentation is the most characteristic of the following disease:
129. A 56-year-old woman has been working as a disinfector for 19 years. She complains of general weakness, nausea, bitter taste in her mouth, heavy sensation. In her right subcostal area, and rapid fatigability. Objectively, her body temperature is 37.1 C, the sclerae are icteric and the liver is enlarged. Total Bilirubin is 40 mcmol/L. What is the likely diagnosis?
Explanation
The liver is the main organ responsible for the metabolism of drugs and toxic chemicals, and so is the primary target organ for many organic solvents. Work activities with hepatotoxins exposures are numerous and, moreover, organic solvents are used in various industrial processes. Organic solvents used in different industrial processes may be associated with hepatotoxicity.
Work activities with hepatotoxin exposure are numerous and include chemists, dry cleaners, farm workers, painters, health care workers, nurses, and printers. Exposure to hepatotoxins can occur through intentional or accidental ingestion in food or absorption of toxic contaminants through the skin.
The patient in question who works as a disinfector for 19 years and presented with signs of liver pathology (liver is enlarged, jaundice) most probably works in the farming industry or health care setting. Farmers and many workers in the agro-food chain are exposed to these substances as well as consumers who eat agri-cultural products that are not properly cleaned and decontaminated.
Among these substances, 1,1,1-trichloro-2,2-bis (p-chlorophenyl)-ethane (DDT) and its metabolite 1,1-dichloro-2,2-bis (p-chlorophenyl)-ethylene (DDE) have been extensively studied. DDT was used both in agriculture and for environmental disinfection until its use was later forbidden in both America and Europe because of its toxic effects on humans. In humans, DDT contamination occurs through con-tact with the skin, mucous membranes and inha-lation.
130. A 43-year-old man complains of facial edema, dyspnea, and difficult swallowing that appeared 3 hours after he was stung by an insect. Objectively the skin of his eyelids, cheeks, and lips is acutely hyperemic and edematous. What medicines should he be prescribed for emergency aid?