1.
A patient was brought by an ambulance to the impatient department. He was provisionally diagnosed with acute pancreatitis. To confirm this diagnosis, it is necessary to measure the activity of a certain enzyme in the patient’s blood and urine. Name the enzyme:
2.
Blood test of the patient revealed albumin content of 20 g/L and increased activity of lactate dehydrogenase isoenzyme 5(LDH5). These results indicate disorder of the following organ.
3.
A 25-year-old woman complains of deteriorating vision. Examination revealed a defect in accommodation, the pupil is dilated and unresponsive to light. What muscles are functionally disturbed in this case?
Explanation
From the question stem, you will notice that the patient has a defect in accommodation and the pupil is dilated (which means it doesn't constrict).
Accommodation is determined by the ciliary muscle, which is a circular (constrictor) smooth muscle that is attached to the lens by suspensory ligaments. The ciliary muscle has only parasympathetic innervation (mediated by acetylcholine acting through muscarinic receptors).
The iris sphincter muscle, also known as the pupillary sphincter or sphincter pupillae, is a muscle located in the colored part of the eye called the iris. The sphincter muscle fibers are located near the pupillary margin and are slightly anterior to the pigmented epithelium of the iris. It encircles the pupil of the iris and functions to constrict the pupil in bright light via the pupillary light reflex or during accommodation. By controlling the diameter of the pupil, the iris controls the amount of light that reaches the back of the eye at the retina.
The question clearly states that there is a defect in accommodation which is clearly a function of the ciliary muscle and the pupil is dilated which means the pupil does not constrict hence, this is a pathology of the Iris sphincter.
The ciliary muscle, Iris sphincter and Iris dilator muscles are the intrinsic muscles of the eye. They are involved in accommodation (ciliary muscle); dilating (Iris dilator/Dilator pupillae) and constricting the eye (Iris sphincter/Sphincter pupillae).
Extrinsic muscles of the eye: Superior oblique; Inferior oblique; Lateral rectus; Medial rectus; Superior rectus and Inferior rectus muscles. They are involved in moving the eyeball up, down, left and right.

4.
One of the causes of pernicious anemia is the disturbed synthesis of transcorrin – Castle’s intrinsic factor in the parietal cells of the stomach. What substance is called Castle’s extrinsic factor?
5.
Proliferation of connective tissue in the liver parenchyma (fibrosis) that results from chronic disorders causes of blood flow disturbance in the classical hepatic lobules. Describe the blood flow direction in these lobules:
6.
Before a surgery, the blood type of a patient is being determined according to the ABO system, using monoclonal antibodies against blood group antigens. Neither anti-A and anti-B reagents caused agglutination. What blood type is it?
7.
When checking donor blood at the blood transfusion station, antibodies to human immunodeficiency virus were found in the blood serum of one of the donors. What method is recommended for confirmation of HIV infection diagnosis?
8.
During a surgery with application of inhalation narcosis and muscle relaxants, the anesthesiologist noticed rapid increase of the patient’s body temperature to 43 degree C. What pathology developed in this patient?
Explanation
The scenario described here is classic for Malignant hyperthermia.
Malignant hyperthermia (Hyperthermic syndrome) is a severe reaction to particular anesthetic drugs that are often used during surgery and other invasive procedures. Specifically, this reaction occurs in response to some anesthetic gases (halothane, sevoflurane, desflurane), which are used to block the sensation of pain, either given alone or in combination with a muscle relaxant (succinylcholine) that is used to temporarily paralyze a person during a surgical procedure.
If given these drugs, people at risk of malignant hyperthermia may experience a rapid increase in heart rate and body temperature (hyperthermia), abnormally fast breathing, muscle rigidity, breakdown of muscle fibers (rhabdomyolysis), and increased acid levels in the blood and other tissues (acidosis).
Hyperthermia, when it occurs, is marked by increase in core temperature at a rate of 1–2°C every five minutes. Severe hyperthermia (core temperature greater than 44°C) may occur, and lead to a marked increase in oxygen consumption, carbon dioxide production, widespread vital organ dysfunction, and disseminated intravascular coagulation (DIC).
In almost all cases, the Malignant Hyperthermia susceptible patients have a defective ryanodine receptor (RYR).
9.
During the exercise testing on a training bicycle, the patient’s respiration rate increased. What is the main cause of the changed activity of respiration center in this case?
Explanation
Any type of physical activity counts as exercise. It could be planned sport such as running, swimming, tennis or bowls, an exercise training programme, or a hobby such as cycling or walking. When you exercise and your muscles work harder, your body uses more oxygen and produces more carbon dioxide.
This buildup of carbon dioxide in the blood makes the blood more acidic than usual, alerting the brain. In response, the brain signals the respiratory drive to increase in pace in an attempt to correct the imbalance. In doing so, the blood pH can return to within the normal range in acidity.
To cope with this extra demand, your breathing has to increase from about 15 times a minute (12 litres of air) when you are resting, up to about 40–60 times a minute (100 litres of air) during exercise. Your circulation also speeds up to take the oxygen to the muscles so that they can keep moving.
10.
A man was hospitalized on the 5th day after the onset of the disease. He was jaundice, myalgia, chills and nasal bleeding. During the laboratory diagnostics, the bacteriologist performed dark field microscopy of the blood drop obtained from the patient. Name the causative agent of this disease:
Explanation
Leptospirosis caused by Leptospira interrogans, commonly occurs in tropical, subtropical and temperate zones. It is acquired by direct or indirect exposure to urine of reservoir animals through contaminated soil, mud and water entering via small abrasions or breaches in the skin.
The causative organism is a spirochete. They are not visible under ordinary microscope, but can be visualized under dark field microscope and phase contrast microscope.
Leptospirosis is an acute generalized infectious disease, characterized by extensive vasculitis, that presents with flu-like symptoms, myalgias (majorly affecting the calf muscles e.g. gastrocnemius), with visible jaundice, photophobia, icteric scleras etc. The icterohemorrhagic form of leptospirosis presents with a severe form of jaundice and azotemia from the liver and kidney dysfunction coupled with anemia.
11.
A 5-year-old child presents with severe progression of bacterial diseases. During blood serum examination, a significant decrease of immunoglobin concentration and absence of B lymphocytes are observed. What immunodeficiency is it?
12.
Autopsy of the body revealed waxy degeneration of the rectus abdominis muscles. In the terminal segment of the small intestine there are ulcers 3-5 cm in diameter. The ulcer walls are covered in a crumbling grayish yellow substance. The ulcer edges are moderately raised above the mucosa. Widal test is positive. Make the diagnosis.
Explanation
The Widal test is one method that may be used to help make a diagnosis of enteric fever, also known as typhoid fever. Enteric fever is a life-threatening illness caused by infection with the bacterium Salmonella enterica serotype Typhi (S. typhi), usually transmitted through food and drinks contaminated with fecal matter. It is associated with symptoms that include high fever, fatigue, headache, abdominal pain, diarrhea or constipation, weight loss, and a rash known as "rose spots." Early diagnosis and treatment are important because serious complications, including severe intestinal bleeding or perforation, can develop within a few weeks.
Intestinal bleeding in typhoid fever usually occurs from the ulcers in the ileum or the proximal colon, and the most common colonoscopic manifestations are multiple variable-sized punched-out ulcerations.
Inflammatory bowel disease is an umbrella term used to describe Ulcerative colitis and Crohn’s disease. Dysentery is often caused by Shigella species. All these conditions will not give a positive Widal test.
13.
A 15-year-old girl complains of rapid fatigability, weakness and palpitations. Blood test: Erythrocytes – 2.5 g/L, Hb – 50 g/L, color index – 0.6, anisocytosis with the prevalence of microcytosis. Blood serum iron is 5.4 mmol. What hematologic pathology is observed in this case?
14.
After a traffic accident, the lower limb of the injured person had to be amputated. For a long time the patient was still feeling the amputated limb and intense unbearable pain in it. What type of pain developed in this patient?
15.
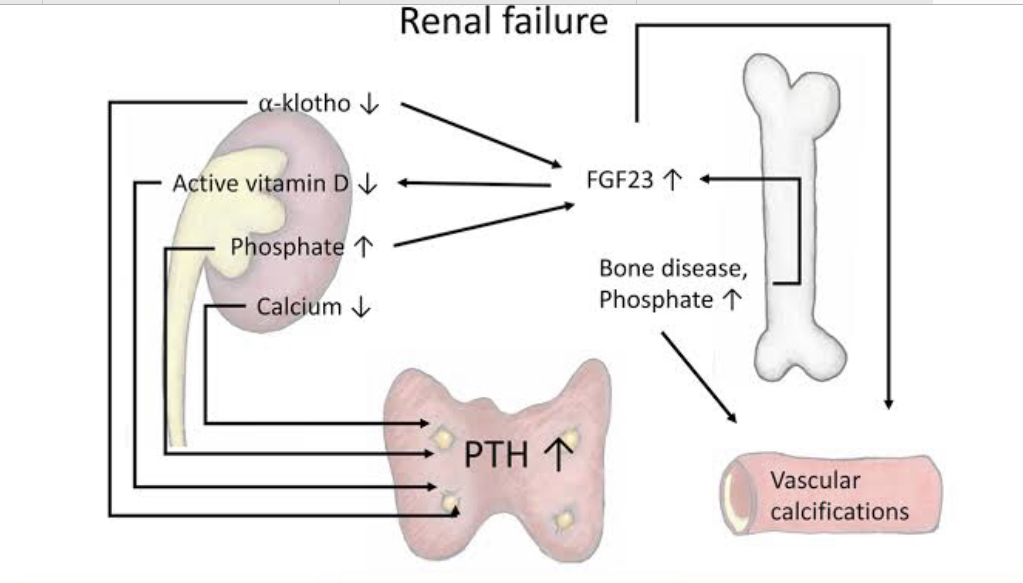
A laboratory rat with chronic kidney failure has osteoporosis, pathologic calcification of the internal organs and arterial hypertension. These disturbances are associated with increased activity of the following hormone:
Explanation
In the blood, the sensitive process of calcium and phosphate homeostasis is maintained primarily by an appropriately functioning parathyroid gland. The parathyroid gland secretes parathyroid hormone (PTH), a polypeptide, in response to low calcium levels detected in the blood. PTH facilitates the synthesis of active vitamin D, calcitriol (1,25-dihydroxycholecalciferol, or vitamin D3) in the kidneys.
Active Vitamin D (Calcitriol) helps to absorb Calcium and Phosphate from the intestine. Parathyroid hormone helps to reabsorb Calcium in the Kidney and also breaks down bone to release Calcium.
Now, a patient with Chronic Kidney disease,
-
cannot make active Vitamin D (Calcitriol is synthesized in the kidney) - which leads to decreased Calcium absorption in the intestine.
-
Cannot reabsorb Calcium in the kidney in response to Parathyroid hormone because there is Kidney failure.
These processes lead to Hypocalcemia (low calcium) which stimulates excessive Parathyroid hormone release - Hyperparathyroidism. Eventually, the excess Parathyroid hormone activates osteoclast which breaks down bone (osteoporosis) to release calcium into the bloodstream.
The calcium then leads to the calcification of internal organs and arterial hypertension (calcium aids smooth muscle contraction in blood vessels).
Calcitonin has no direct effect on the kidneys. Its effect is also minimal in calcium homeostasis. Triiodothyronine, T3 and Thyroxine, T4 - both are thyroid hormones and are not involved in calcium metabolism. Adrenaline/Epinephrine - is a neurotransmitter produced in the adrenal medulla and is not involved in calcium metabolism.
16.
A 26-year-old woman was brought into the maternity department. Considering the term of her pregnancy (40 weeks), she should have gone into labor already. Examination determined that the uterine cervix is open but uterine contraction are absent. The doctor gave her a hormone drug for intensification a labor activity. Name this drug:
17.
A test animal received electrical impulses that irritate the sympathetic nerve that innervates blood vessels of the skin. What reaction will it cause in the blood vessels?
18.
A 50-year-old man complains of a hoarse voice and difficult breathing. Examination detected a laryngeal tumor in the region of the vocal cords. In this case metastases can spread to the following regional lymph nodes:
Explanation
Lymphatic drainage is important to understand due to the aggressive metastasis of some laryngeal cancers. The lymphatics of the larynx above the vocal cords drain initially to the infrahyoid nodes or directly to the deep cervical chain. The laryngeal lymphatic vessels below the vocal cords drain to the prelaryngeal and pretracheal nodes or directly to the deep cervical chain.
The deep (cervical) lymph nodes receive all of the lymph from the head and neck – either directly or indirectly. They are numerous in number, but include the prelaryngeal, pretracheal, paratracheal, retropharyngeal, infrahyoid, jugulodigastric (tonsilar), jugulo-omohyoid and supraclavicular nodes.
The superficial cervical lymph nodes can be divided into the superficial anterior cervical nodes and the posterior lateral superficial cervical lymph nodes. The anterior nodes collect lymph from the superficial surfaces of the anterior neck. The posterior nodes collect lymph from superficial surfaces of the neck.
Submandibular nodes are located below the mandible in the submandibular triangle and collect lymph from the cheeks, the lateral aspects of the nose, upper lip, lateral parts of the lower lip, gums and the anterior tongue. They also receive lymph from the submental and facial lymph nodes.
Submental: collect lymph from the central lower lip, the floor of the mouth and the apex of the tongue.
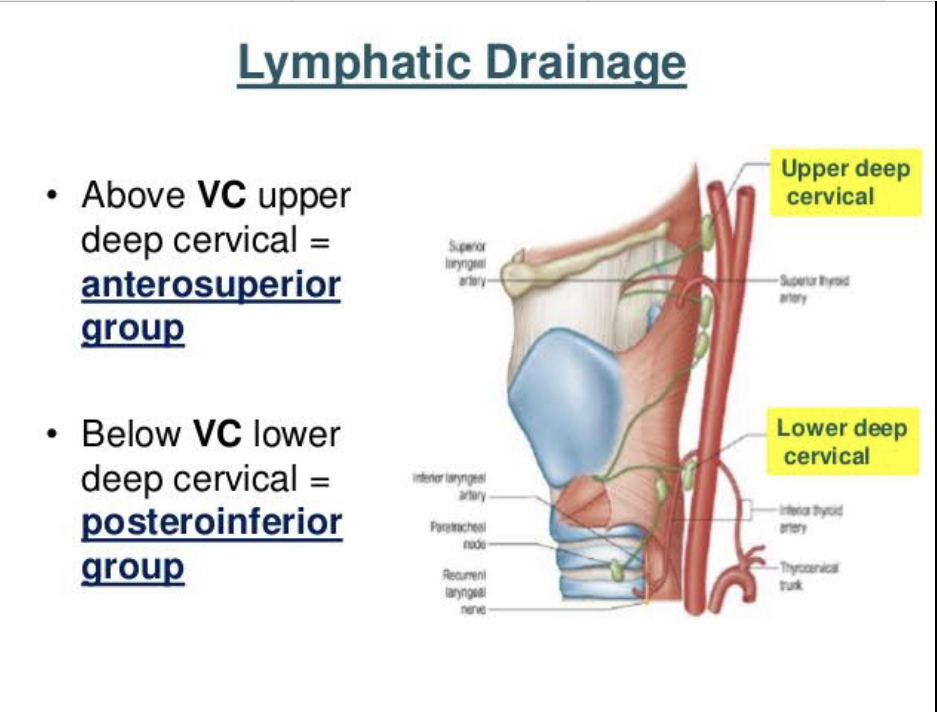 VC: Vocal Cord
VC: Vocal Cord 19.
Clinical instrumental examination of a patient allowed to provisionally diagnose him with liver cancer. What protein is indicative of this diagnosis, if it is present in the blood serum?
20.
10 days after the administration of an antitoxic anti-diphtheritic serum, a child with diphtheria developed skin rashes accompanied by severe itching, body temperature increased up to 38 degree C, the child developed pain in the joints. What likely cause of these phenomena can be suggested?
21.
Parents of a sick child came to the infectious disease specialist. The parents were working in India for a long time. The child has the following signs: a gray tint to the skin tone, loss of appetite, inertness, enlarged liver, spleen and lymph nodes. What protozoan disease can be suspected in the child?
Explanation
Leishmaniasis is due to protozoan parasites from the Leishmania species from being bitten by an infected sand fly. The sand flies that carry the parasite typically reside in tropical and subtropical environments. Fatal epidemics have occurred in areas of Asia, East Africa, and South America.
Leishmaniasis comes in three forms: cutaneous, visceral, and mucocutaneous.
Visceral leishmaniasis is sometimes known as systemic leishmaniasis or kala azar. It usually occurs two to eight months after being bitten by a sand fly. It damages internal organs, such as your spleen and liver. It also affects your bone marrow, as well as your immune system through damage to these organs.
Lambliasis is caused by Giardia lamblia, presents with diarrhea and foul smelling stool.
Toxoplasmosis caused by Toxoplasma gondii, found in cat feces, presents with muscle pain, fever and headache.
Balantidiasis, caused by Balantidium coli, commonly found in pigs and in humans, it presents with gastrointestinal symptoms like chronic diarrhea, abdominal pain etc.
Amebiasis, caused by Entamoeba histolytica, presents with loose stool, abdominal cramping, and stomach pain.
22.
ECG of the patient shows increased duration of the QRS complex. What is the most likely causes?
Explanation
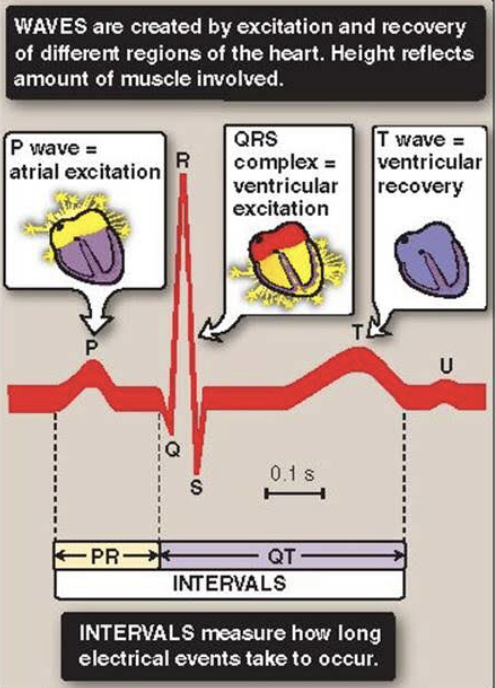
An electrocardiogram, or ECG, is a recording of the heart’s electrical activity as a graph over a period of time. A typical ECG tracing of the cardiac cycle (heartbeat) consists of a P wave (atrial depolarization), a QRS complex (ventricular depolarization), and a T wave (ventricular repolarization).
The first wave on an ECG is the P wave, indicating atrial depolarization in which the atria contract (atrial systole). The QRS complex refers to the combination of the Q, R, and S waves, and indicates ventricular depolarization and contraction (ventricular systole).The T Wave indicates ventricular repolarization, in which the ventricles relax following depolarization and contraction.
Therefore, an increased duration of the QRS complex corresponds to an Increased period of ventricular excitation.
The flat line (Isoelectric line) between the P wave and the beginning of the QRS complex indicates the conduction through the AV node.
Increased atrial and ventricular excitability will basically affect both the P wave and the QRS complex. (NB: the question only mentioned the QRS complex).
Increased period of atrial excitation = prolonged P wave
23.
Blood test shows the following: Sodium – 115 mmol/L, chlorides – 85 mmol/L, glucose – 6 mmol/L, total protein – 65 g/L. The first consequence of such changes will be the decrease of:
24.
A patient complains of frequent and excessive urination and thirst. Urinalysis revealed the following: 24 hour diuresis – 19 liters, specific gravity – 1.001. These values are characteristic of:
25.
A 16-year-old girl has no hair on the pubis and in the armpits, her mammary glands are underdeveloped, no menstruation. This condition can be caused by the following hormone imbalance:
Explanation
The period between puberty and menopause represents the reproductive window of most women. If the ovaries stop working prematurely (roughly before the age of 40) and there are subsequently no menstrual periods, this is called premature ovarian failure. When this happens, your ovaries don't produce normal amounts of the hormone estrogen or release eggs regularly. This condition often leads to infertility.
In the absence of ovarian hormones, secondary sexual characteristics like pubic hair growth and breast enlargement will be absent as well.
In females, breasts are a manifestation of higher levels of estrogen; estrogen also widens the pelvis and increases the amount of body fat in hips, thighs, buttocks, and breasts. Estrogen also induces growth of the uterus, proliferation of the endometrium, and menstruation.
Estrogen that is responsible for all these, is produced in the Ovary. When there is ovarian failure, there will be decreased or absent estrogen which will result in the manifestations seen in this patient.
Pancreatic Islet failure - Diabetes Mellitus
Hyperthyroidism - Heat intolerance, weight loss, diarrhea, tachycardia
Hypothyroidism - Cold intolerance, weight gain, constipation, bradycardia
Adrenal medulla hyperfunction - a good example of this is Pheochromocytoma - hyperfunction of the sympathetic nervous system - hypertension, excessive sweating etc.
26.
A patient has an allergic response with itching, edemas and skin redness. In the tissues there is an increased concentration of a certain biogenic amine. Name this biogenic amine:
27.
It is known that hepatitis D virus belongs to defective viruses and can reproduce in the host cells only in the presence of another hepatitis virus. Name this other hepatitis virus:
28.
Genealogical analysis of a child with myotonic dystrophy determined that this disease manifests in every generation, is in equal measure present in the relatives of both genders, the risk of inheriting this disease is equal no matter which parent is affected. If one of the parents is heterozygous for this disease and the other parent is healthy, the risk of them giving birth to a sick child is 50%. What type of disease inheritance is it?
29.
A certain vitamin is a component of glutamic acid decarboxylase as a coenzyme, takes part in the formation of gamma-aminobutyric acid and its deficiency manifests as convulsions. Name this vitamin:
30.
Histological specimen shows parenchyma of an organ that consist of lymphoid tissue that forms lymph nodules; the nodules are located diffusely and have a central artery. What anatomical structure has such morphological characteristic?
31.
A medical student was hospitalized into the infectious diseases unit on the 2nd day after the disease onset. The patient is suspected to have infectious mononucleosis. What results of laboratory analysis can confirm this diagnosis immediately on the day of the hospitalization.
32.
After a spinal trauma the patient was lost proprioceptive sensitivity in the lower half of the body and in the lower limbs. What sensory conduction pathway was likely damaged, leading to the loss of sensitivity?
33.
A patient presents with an acute attack of cholelithiasis. Laboratory examination of the patient’s feces will show the following in this case:
34.
Autopsy of the body of 72-year-old woman, who was suffering from rheumatoid arthritis and died of uremia, revealed enlarged pale gray kidneys with glossy lardaceous surface on section. Based on the macroscopic changes, the pathologist suspected:
Explanation
Secondary or reactive amyloidosis occurs as a complication of chronic infectious or noninfectious inflammatory conditions associated with tissues destruction such as Tuberculosis, Autoimmune disorders (Rheumatoid arthritis, dermatomyositis, scleroderma), Chronic Osteomyelitis, Inflammatory bowel disease (Ulcerative colitis and Crohn’s disease) etc.
Secondary amyloidosis is typically distributed in solid abdominal organs like the liver, kidney, spleen and adrenals. In renal amyloidosis, the kidneys may be normal-sized, enlarged or contracted. Cut surface is pale waxy and translucent.
From the information given in the question stem: 72 year old woman suffering from Rheumatoid arthritis (a predisposing condition for secondary amyloidosis) with an enlarged, glossy lardaceous kidney, it is safe to suspect a Renal Amyloidosis here.
35.
The patient notes frequent diarrheas, especially after eating fatty food and loss of weight. Laboratory testing detected steatorrhea and hypocholic feces. What is the likely cause of this condition?
36.
A person developed increased pulmonary ventilation due to physical exertion. What indicator of external respiration will be significantly increased compared to the resting state?
37.
A 48-year-old man is unconscious. He has a history of several syncopal episodes with convusions. ECG shows deformed QRS complexes unconnected with P waves, atrial contractions are approximately 70/min, ventricular contractions are 25-30/min. Name the type of arrhythmia in this case:
38.
An oncology patient is to undergo a surgery on the descending colon. Name the main source of the blood supply to this organ:
39.
Body fluids, especially urine, of a sick child produce a specific sweet odor. It is associated with the disturbed metabolism of such amino acids as leucine, isoleucine and valine. What diagnosis will be made by the doctor in this case?
Explanation
Elevated concentrations of branched-chain amino acids (leucine, isoleucine, and valine), as well as a generalized disturbance of amino acid concentration ratios, are present in blood and the maple syrup odor can be detected.
Maple syrup urine disease (MSUD) is caused by decreased activity of the branched-chain alpha-ketoacid dehydrogenase complex (BCKD), the second enzymatic step in the degradative pathway of the branched-chain amino acids (BCAAs), which includes leucine, isoleucine, and valine.
Alkaptonuria (ochronosis): accumulation of Homogentisic acid due to deficiency of Homogentisate dioxygenase. Patients have dark urine or urine that turns black when exposed to air.
Phenylketonuria: accumulation of Phenylalanine due to deficiency of Phenylalanine hydroxylase. It can lead to intellectual disability, seizures, behavioral problems, and mental disorders with a musty smell and lighter skin.
Fructosuria: deficiency of Fructokinase or Aldolase B, accumulation of Fructose or Fructose-1-phosphate.
Galactosemia: deficiency of Galactokinase, accumulation of Galactose.
40.
Examination of the femoral bone detected chronic suppurative inflammation of the compact substance and bone marrow, formation of bone sequestra. What disease is associated with such changes?
41.
Autopsy of the body revealed a large wedge-shaped patch of dense dark red tissue with clear margins in the upper lobe of the right lung. Histological examination detected there necrosis of the alveolar walls; the alveolar lumen is tightly packed with erythrocytes. What process occurred in the lungs?
42.
A nurse mistakenly gave nearly a double dose of insulin to a patient with diabetes mellitus, which caused hypoglycemic coma in the patient. What medicine should be administered to bring the patient out of the coma?
43.
A lab rat has subcutaneously received mercury(II) chloride in the amount of 5 mg/kg. 24 hours later the plasma creatinine concentration increased several times. What mechanism of retention azotemia is observed in this case?
44.
In the hospital a patient was diagnosed with anemia. During the anamnesis collection, it was revealed that the patient had been suffering from peptic ulcer disease of the stomach for several years already. What type of anemia is most likely in this patient?
45.
24 hours after an appendectomy the patient’s blood test shows neutrophilic leukocytosis with a regenerative shift. What is the most likely mechanism of absolute leukocytosis development in the patient’s peripheral blood?
46.
A patient with massive burns received a skin graft from a donor. On the 8th day after the grafting, the transplant became edematous and discolored. On the 11th day transplant rejection started. What cells take part in this process?
47.
A 15-year-old teenager complains of general weakness, dizziness and rapid fatigability. Examination detected deformed erythrocytes, their number is decreased. The provisional diagnosis of sickle-cell anemia was made. What amino acid replacement in hemoglobin causes the development of this pathological condition?
48.
Name the supramolecular multienzyme complex that is integrated into the lipid layer of inner mitochondrial membrane that creates conditions for redox reactions:
49.
The process of tissue respiration is accompanied by oxidation of organic compounds and synthesis of macroergic molecules. In what organelles does this process occur?
50.
A patient with ischemic heart disease has increased levels of triglycerides and low density lipoproteins in this blood plasma. What medicine should he be prescribed?
51.
A woman with enteritis accompanied by severe diarrhea presents with the loss of water in the extracellular space, increased water content in the cells and decreasing blood osmolarity. Name this type of water-electrolyte imbalance:
52.
Autopsy of the body of a person, who died after an abdominal surgery, revealed numerous thrombi in the veins of the lesser pelvis. Clinically, thromboembolism syndrome was registered. Where should the pathologist search for thromboembolis?
53.
A patient with essential hypertension developed a cough during the systematic treatment with a hypotensive drug. What drug of those listed below can cause such a side effect?
Explanation
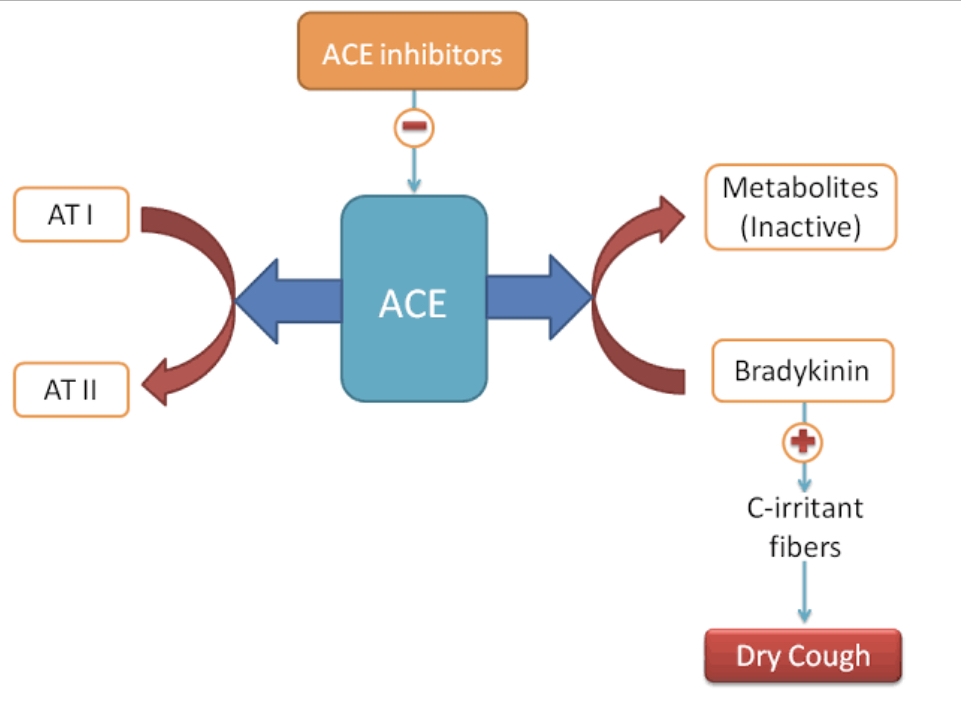
Angiotensin-converting enzyme inhibitors (ACE-I) like Lisinopril, Enalapril etc., are widely used in diseases, such as hypertension, congestive heart failure, and myocardial infarction. A dry, tickly and often bothersome cough is the most common adverse effect of ACE inhibitors.
In normal physiology, angiotensin I is converted to active angiotensin II by ACE produced by the capillaries in the lungs. Angiotensin II has many physiological effects, such as increasing the resistance of blood vessels, causing adrenal cortex aldosterone release, and stimulating vasopressin which all lead to an increased blood pressure. So, by inhibiting the ACE, we are able to bring down the blood pressure.
However, angiotensin converting enzyme (ACE) is also involved in the breakdown of bradykinin. Once ACE inhibitors are used, bradykinin accumulates. The increased bradykinin irritates the airways and produces dry cough.
Lisinopril is the only ACEI listed as an answer choice.
Verapamil: Calcium channel blocker
Prazosin: alpha 1 receptor blocker
Hydralazine: vasodilator
Dibazol: vasodilator with analgesic effect
54.
Pterin derivatives – aminopterin and methotrexate – are competitive inhibitors of dihydrofolate reductase. As a result, they suppress the regeneration of tetrahydrofolic acid from dihydrofolate. These medicines lead to the inhibition of intermolecular transport of one-carbon groups. In the process, the biosynthesis of the following polymer is suppressed:
55.
A 2 year old child presents with marked delay in psychomotor development, vision and hearing deterioration, marked enlargement of the liver and spleen. The child is diagnosed with hereditary Neimann-Pick disease. What genetic defect is the cause of this disease?
56.
The patient presents with smoothed out nasolabial fold, dilated right palpebral fissures (It cannot be closed when squinting, because of eyelids would not close), there are difficulties during speaking and eating (Food gets stuck between the cheek and teeth). What nerve is damaged in this case?
57.
A woman was hospitalized in a severe condition with the following diagnosis; hemorrhagic stroke in the region of the medial surface of the right frontal lobe. What artery is likely to be damaged, causing this condition in the patient?
58.
In an experiment, a frog neuromuscular preparation had been processed with a curare-like substance, which led to the disappearance of muscle contractions in response to electrical stimulation. What function of the muscle cell membrane is disrupted by curare-like substance?
59.
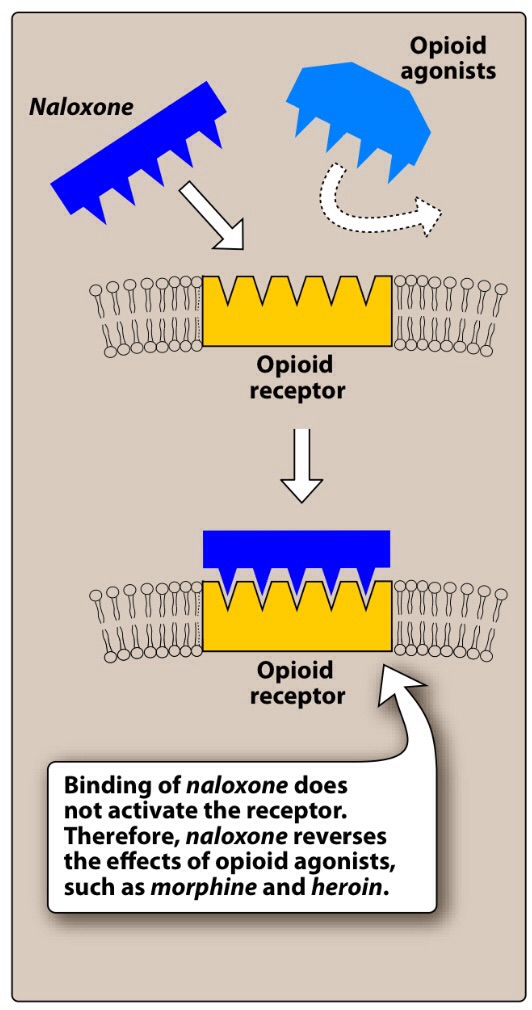
An unconscious patient was brought into the admission room. He presents with cold skin, constricted pupils, difficult respiration with Cheyne-Stokes pattern, low blood pressure, overfilled urinary bladder. He was diagnosed with morphine poisoning. What drug should the patient be given as an antagonist in this case?
Explanation
Naloxone is an opioid antagonist medication used to block or reverse the effects of opioid drugs, particularly within the setting of drug overdoses which are rapidly becoming a leading cause of death worldwide. More specifically, naloxone has a high affinity for μ-opioid receptors, where it acts as an inverse agonist, causing the rapid removal of any other drugs bound to these receptors. When taken in large quantities, opioid medications such as morphine, hydromorphone, methadone, heroin, or fentanyl are capable of causing life-threatening symptoms such as respiratory depression, reduced heart rate, slurred speech, drowsiness, and constricted pupils.
Bemegride is a central nervous system stimulant.
Unithiol is used in poisoning with mercury and mercury salts.
Sodium thiosulfate is used to treat cyanide poisoning.
Cytitone has been used as a smoking cessation treatment.
60.
A patient has developed status epilepticus. What medicine should be used in this case to stop the seizures?
Explanation
Convulsive status epilepticus is a neurological emergency in adults and children. The benzodiazepines are some of the most effective drugs in the treatment of acute seizures and status epilepticus. The benzodiazepines most commonly used to treat status epilepticus are diazepam (Valium), lorazepam (Ativan), and midazolam (Versed). All three compounds work by enhancing the inhibition of γ-aminobutyric acid (GABA) by binding to the benzodiazepine-GABA and barbiturate-receptor complex.
Sodium bromide can be used as a hypnotic, as an anticonvulsant, and as a sedative. Even though Sodium bromide can be used as an anticonvulsant, drugs in the class of Benzodiazepines (diazepam, Lorazepam) have higher efficacy and potency.
Trihexyphenidyl is used to treat symptoms of Parkinson's disease or involuntary movements due to the side effects of certain psychiatric drugs.
Promethazine is used to treat anaphylaxis (sudden, severe allergic reactions) and the symptoms of the common cold such as sneezing, cough, and runny nose. Also to treat nausea and vomiting related to certain conditions (such as before/after surgery, motion sickness).
Valerian is most commonly used for sleep disorders, especially the inability to sleep (insomnia).
61. In the process of acetylcholine interaction with muscarinic acetylcholine receptors of contractile cardiomyocytes, a bioactive substance is being produced. This bioactive substance leads to inactivation of calcium channels, decrease of calcium ions entry into the cardiomyocytes and development of negative inotropic effect. Name this substance:
62.
Examination showed that total leukocyte count in the patient’s blood is 11 x 109/L, with 80% neutrophils, among which 9% are band neutrophils. Characterize the changes in the cell composition of ‘white’ blood in this case:
63. Blood smear analysis of a blood sample obtained from a patient with inflammatory process shows a large number of round cells with segmented nucleus (three or more segments) and fine pink-violet granulation in the cytoplasm. Name the blood cells:
64. A newborn boy has dolichocephalic skull, microcephaly and defects of heart, kidneys and digestive system. The child’s karyotype is 47, XY + 18. Make the diagnosis:
65. A histological specimen demonstrates a vessel with the wall that consists of endothelium, basement membrane and loose connective tissue. What type of vessel is it?
66. Arterial blood pH is 7.4; Primary urine pH is 7.4; final urine pH is 5.8. Decreased pH of the final urine results from the secretion of a certain substance in the nephron tubules. Name the substance:
67. A patient came to the hospital complaining of abdominal distension, diarrhea and meteorism that occur after eating protein-rich food, which indicated disturbed protein metabolism and intensified protein putrefaction. What substance is the product of this process in the intestine?
68. A patient complains of acute increase in diuresis (upto 5-7 liters of urine per 24 hours). Examination of vasopressin in this patient. What cells have insufficient secretory activity in this case?
69. A 35-year-old man complains of a severe rhinitis and a loss of sense of smell for a week. Examination detected in the nasal cavity a large amount of mucus that covered the mucosa and blocked the olfactory receptors. Where in the nasal cavity are these receptors located?
70.
A 50-year-old man experienced a severe stress. His blood levels of adrenaline and noradrenaline sharply increased. What enzyme catalyze the process of noradrenaline inactivation?
71. Due to a case of diphtheria, preventive immunization of the whole contact group of students is necessary. What preparation should be used to produce artificial active immunity?
Explanation
Before we try to answer this question, let’s take a minute to know some definitions.
Passive immunity is protection from a disease provided by antibodies created outside of the body. Maternal passive immunity, or natural passive immunity, is immunity passed along from mother to child.
Active immunity is defined as immunity to a pathogen that occurs following exposure to said pathogen. Natural active Immunity is when the patient is infected naturally. Artificial active Immunity is when a vaccination is administered. In this case, the infectious agent or toxin is artificially introduced so the body can develop immunity to it.
Anatoxin is a bacterial toxin that has been weakened until it is no longer toxic but is strong enough to induce the formation of antibodies and immunity to the specific disease caused by the toxin.
Now, a diphtheria anatoxin is a weakened diphtheria toxin that is administered (artificial immunity) so that the body can develop immunity to the toxin.
Since we are introducing the pathogen or toxin - Active
Hence, we have an artificial active immunity.
Anti-diphtheria serum (antibodies), specific immunoglobulins are examples of an Artificial Passive Immunity. (mother to child is Natural Passive Immunity).
DTP (Diphtheria, Tetanus, Pertussis), since we are concerned about Diphtheria alone, then Diphtheria anatoxin is a better answer choice.
72. A woman who works as a shop assistant and suffers from phlebitis, developed a thrombus in the area of the varicose veins in her leg. What pathogenetic factor was primary in the process of thrombus formation in this case?
73.
Section shows a significantly enlargement of the patient’s right kidney. There is a nephrolith at the place of the incision. Renal pelvic lumen is distended with accumulating urine. The renal parenchyma is substantially thinned out. What is the most correct diagnosis?
Explanation
Hydronephrosis is a condition of the urinary tract where one or both kidneys swell. This happens because urine does not fully empty from the body. Symptoms may include sudden or intense pain in the back or side, vomiting, painful urination, blood in the urine, weakness and fever due to a urinary tract infection.
If only one of the kidneys is affected, the condition is called unilateral hydronephrosis. If both kidneys are affected, it is called bilateral hydronephrosis.
Hydronephrosis is caused by a blockage in the tube that connects the kidney to the bladder (ureter). Possible causes include a kidney stone, an infection, an enlarged prostate, a blood clot or a tumour.
From the question stem, we were told of a nephrolith (stone) at the incision site, this stone caused the blockage leading to the backup of urine causing right hydronephrosis.
Hydroureteronephrosis - this means the kidney and the ureter are both distended but the question only mentioned the kidney as being distended. So, hydronephrosis which is Kidney enlargement due to blockage preventing urine outflow is a better answer choice here.
Pyelectasis is a mild form of hydronephrosis. When the pelvis is stretched or enlarged, but not enlarged enough for doctors to diagnose hydronephrosis, it is considered pyelectasis. Pyelectasis also is known as renal pelvic dilatation. (Dilatation means stretching or enlargement).
Nephroblastoma is a tumor. This question clearly states the patient has a stone (nephrolith) not a tumor and also not a cyst.
74. A 46-year-old man was brought to the hospital specializing in nervous system disease. The man was provisionally diagnosed with cerebral hemorrhage. The patient presents with frequent spontaneous limb movements intermittent with the state of limb muscle hypertonia. These signs can be explained by the damage to the following brain structures:
Explanation
This patient obviously just had a stroke (cerebral hemorrhage) involving the deep structures of the brain and presents with chorea. Chorea is a movement disorder that causes involuntary, irregular, unpredictable muscle movements.
Movement disorders that manifest following a stroke are most frequently associated with lesions in the basal ganglia (44%) and the thalamus (37%). These movement disorders are primarily associated with the basal ganglia and the thalamus; therefore, movement disorders are more frequently manifest after stroke compared with neurological injuries associated with other structures of the brain.
Dystonia and chorea are commonly occurring post-stroke movement disorders in the basal ganglia circuit. Rarer movement disorders, including tic, restless leg syndrome, and blepharospasm, can also develop following a stroke.
Stroke in the brain stem will present with vertigo, dizziness, hearing loss, loss of ability to speak, weakness on one side of the body.
Stroke in the frontal cortex will present with hemiparesis or hemiplegia. This involves weakness or paralysis on one side of the body, usually the opposite side of the stroke. Speech difficulties, dysphagia, behavioural changes.
Stroke in hypophysis (pituitary gland) will present with headache and vision loss if the optic chiasm is affected.
Stroke in the hypothalamus will present with loss of sensation, memory loss, sleep disturbance etc.
75. After a boy cell from a tree, the arm abduction to the horizontal position is difficult for him. What muscle is likely to be damaged in this case?
76. A 7-year-old child developed sore throat and high body temperature. On the 2nd day after the onset of the disease, there appeared dense red rashes that look like small spots that size of a poppy seed. They cover the whole body, except the nasolabial triangle. Examination of the oral cavity revealed bright red pharynx, enlarged tonsils and raspberry-red tongue. Make the diagnosis:
Explanation
Scarlet fever is a rash most commonly associated with bacterial pharyngitis in school-age and adolescent children. It is a blanching, papular rash that is classically described as a “sandpaper” rash. The causative bacteria is Streptococcus pyogenes, Group A Strep (GAS).
The rash develops within 2 to 3 days after infection but can be delayed up to 7 days. The trunk, underarms, and groin are affected first, and then it spreads to the extremities. Usually, the palms and soles are spared. The circumoral area is also spared, making it pallor-like. The “strawberry tongue” begins with a white coating of the tongue with hyperplastic papillae. As the white coating resolves, the papules remain, giving the appearance of a strawberry.
Pharyngeal diphtheria is commonly associated with grey white coating on tonsils that are difficult to remove and if removed, it can bleed.
Adenovirus infection is associated with sore throat + conjunctivitis (red eyes). It is sometimes called Pharyngoconjunctiva fever.
Measles presents with a classic triad of coryza, cough, conjunctivitis + Koplik spots (around 2nd molar teeth on the cheek).
77. For the relief of intestinal colic a patient was prescribed atropine sulfate. What disease can be contraindication for administration of this medicine?
78. Puncture biopsy of a transplanted kidney detected there a diffuse stromal infiltration by lymphocytes, plasma cells, lymphoblasts and plasmablasts as well as necrotizing arteritis. What pathological process developed in the transplant?
79. A young woman suddenly developed cough and bronchial spasm, when she entered into a room with high concentration of tobacco smoke. What receptors activated this defensive reflex?
Explanation
Cough is an important protective mechanism that clears foreign material from the airway and aids in immune defence. Numerous environmental irritants are known to induce coughing such as air pollution, tobacco smoke, smoke from burning vegetation, and vehicle exhaust.
Chemical irritants bind to Irritant receptors, which open ion channels on the terminals of the airway sensory nerves, leading to membrane depolarisation, then send signals to the CNS in the form of action potentials. Second order neurons then relay the message to a respiratory pattern generator within the CNS, which interprets the afferent information, resulting in activation of motor neurons and ultimately initiation of coughing.
Irritant receptors detect chemical and environmental irritants.
Pleural receptors (visceral pleural receptors) detect over stretching and pain in the lungs.
Central chemoreceptors located in the medulla oblongata of the brainstem are sensitive to the level of CO2.
Pulmonary mechanoreceptor is a form of stretch receptors in the lungs. When the lung expands, the receptors initiate the Hering-Breuer reflex, which reduces the respiratory rate.
Juxtacapillary, or “J,” receptors are located in the alveolar walls in close proximity to the capillaries. Because of their location, these receptors respond readily to chemicals in the pulmonary circulation, distention of the pulmonary capillary walls, and accumulation of interstitial fluid.
80. A patient has peptic ulcer of the stomach. What medicine can decrease the secretion of hydrochloric acid and pepsin by blocking the H2 receptors?
81. A 40-year-old woman was diagnosed with bronchial asthma that manifests as periodical asphyxia attacks. What type of ventilatory insufficiency can be observed in patient during an attack?
82. A patient with an injury of the greater psoas muscle was delivered to the traumatology center. The patient has lost the ability to extend the lower leg at the knee joint. What nerve is damaged in this case?
83.
A patient complains of pain in the upper umbilical region. On palpation there is a mobile painful intestine. What intestine is being palpated by the doctor?
84. A 5-year-old child is diagnosed with Bruton’s disease (X-linked agammaglobulinemia) that manifests itself in severe clinical course of bacterial infections and absence of B lymphocytes and plasma cells. What changes in the immunoglobulin content can be observed in the blood serum of the child with immunodeficiency?
Explanation
Bruton agammaglobulinemia, also known as X-linked agammaglobulinemia (XLA) or Bruton\'s agammaglobulinemia, is an inherited immunodeficiency disorder. It is characterized by the absence of mature B cells which in turn leads to severe antibody deficiency and recurrent infections. It can manifest in an infant as soon as the protective effect of maternal immunoglobulins wanes at around six months of age.
There is a failure of B cell development in affected individuals. Immunoglobulin-secreting plasma cells also are absent, resulting in deficiency (hypogammaglobulinemia) or absent (agammaglobulinemia) immunoglobulins.
The deficiency of immunoglobulins results in absent antibody responses and increases the tendency to develop bacterial infections. Encapsulated pyogenic bacteria are usually the culprits because they are opsonized by antibodies as a defense mechanism. Thus Streptococcus pneumoniae, Haemophilus influenzae type B, Streptococcus pyogenes, and the Pseudomonas species are some of the common causative organisms.
With this background information, we can rule out the option - No changes; we can also conclude that Increased IgA, IgM and Increased IgD and IgE can be ruled out (absent antibodies, so it can’t be increased).
Note that the patient was said to have a severe bacteria infection - IgA and IgM are more involved in the eradication of bacteria. So, decreased IgA, IgM is the best choice here.
IgE - mainly involved in allergic reactions. IgD - function is not clear.
85. In a hypothetical experiment, the action of a toxic substance disrupts the mechanism of nerve impulse transmission between neurons. What structure enables this function?
86. A 45-year-old woman has breast cancer. Metastases can spread in this case to the following regional lymph nodes:
87. Due to a cerebral hemorrhage, the patient developed a disturbed speech perception (sensory aphasia). What brain structure is likely to be damaged in this case?
Explanation
Sensory aphasia is characterized by impaired auditory comprehension with intact repetition and fluent speech. Also called Receptive aphasia, Wernicke's aphasia: inability to understand spoken, written, or tactile speech symbols that results from damage (as by a brain lesion) to an area of the brain (as Wernicke's area) concerned with language.
The simplest way to describe sensory aphasia is to think of it as a form of Wernicke's aphasia in which the patient exhibits a severe comprehension deficit, but in which repetition, and thus articulation, is well preserved.
Superior temporal gyrus is responsible for processing sounds. It includes Wernicke's area, which is the major area involved in the comprehension of language.
Expressive aphasia, also known as Broca's aphasia, is a type of aphasia characterized by partial loss of the ability to produce language (spoken, manual, or written), although comprehension generally remains intact. Inferior frontal gyrus - Broca's area.

88. Acute herpetic gingivostomatitis is the most common primary infection caused by herpes simplex virus type 1. What material should be obtained by a dentist for the laboratory testing that will confirm the diagnosis?
89. The mountain climbers, who without oxygen equipment were climbing a mountain, at the altitude of 5000 meters above the sea level developed tachycardia, low blood pressure, fast respiration rate. What type of hypoxia did they develop?
Explanation
The further you move away from sea level up into higher altitudes, the lower the air pressure is. This can result in hypoxia.
Hypoxia in medicine refers to a condition of the body in which the tissues are starved of oxygen. In its extreme form, where oxygen is entirely absent, the condition is called anoxia.
Hypoxemic/Hypoxic Hypoxia, in which the oxygen pressure in the blood going to the tissues is too low to saturate the hemoglobin. Often encountered in pilots, mountain climbers, and people living at high altitudes—due to reduced partial pressure of oxygen.
The Hemic/anemic type, in which the amount of functional hemoglobin is too small, and hence the capacity of the blood to carry oxygen is too low. It can be seen in anemia or carbon monoxide poisoning and methemoglobinemia, of which the hemoglobin is so small or altered by toxic agents that it becomes unavailable for oxygen transport.
Circulatory type, in which the blood is or may be normal but the flow of blood to the tissues is reduced or unevenly distributed e.g. in heart failure. Same mechanism for Respiratory hypoxia as well, as in respiratory failure or pathologies that impairs the pulmonary function.
Tissue/histotoxic type, in which the tissue cells are poisoned and are therefore unable to make proper use of oxygen. As seen in cyanide poisoning, narcotics, alcohol and certain anesthetic agents.
90. A 9-year-old child developed a severe case of purulent destructive pneumonia, for which the child received a massive antibacterial therapy. The disease was rapidly progressing. Against the background of marked intoxication, a sharp drop in blood pressure was registered, the patient went into the state of shock, which resulted in the death of the patient. What etiopathogenetic type of shock developed in the child?
Explanation
Toxic shock syndrome (TSS) is a toxin-mediated acute life-threatening illness, usually precipitated by infection with either Staphylococcus aureus or group A Streptococcus (GAS), also called Streptococcus pyogenes. It is characterized by high fever, rash, hypotension, multiorgan failure (involving at least 3 or more organ systems), and desquamation, typically of the palms and soles, 1-2 weeks after the onset of acute illness. The clinical syndrome can also include severe myalgia, vomiting, diarrhea, headache, and nonfocal neurologic abnormalities.
Hemolytic shock will result from a massive breakdown of red blood cells in the body which could be as a result of transfusion reaction or Glucose 6-phosphate dehydrogenase deficiency.
Anaphylactic shock is an immediate hypersensitivity reaction (Type I).
Hypovolemic shock is often caused by massive hemorrhage.
Cardiogenic shock is a direct result of cardiac failure.
In this case, the patient was reported to have developed a severe case of purulent destructive pneumonia which is consistent with Toxic shock syndrome.
91. A patient suffers from the eye muscle paralysis, there are pupillary disturbances and pain along the trigeminal nerve. Aneurysm(dilation) of a certain venous sinus can be suspected. Name this venous sinus:
92. A patient has cardiac rhythm disturbance. ECG shows heart rate of 60/min, prolongation of PQ interval, periodical loss of QRS complex. What cardiac rhythm disturbances is it?
Explanation
Key point to note here: Prolongation of PQ interval; Periodical loss of QRS complex
This is the only information you need to answer this question.
Now let’s compare the answer choices.
Atrioventricular (AV) or heart block is partial or complete interruption of impulse transmission from the atria to the ventricles. We have 3 degrees of heart block.
First Degree AV block: All normal P waves are followed by QRS complexes, but the PR interval is longer than normal (>0.20 second).
Second Degree AV block: Some normal P waves are followed by QRS complexes, but some are not. Two types exist:
-
Mobitz type I
-
Mobitz type II
In Mobitz type I 2nd-degree AV block, the PR interval progressively lengthens with each beat until the atrial impulse is not conducted and the QRS complex is dropped (Wenckebach phenomenon); AV nodal conduction resumes with the next beat, and the sequence is repeated.
In Mobitz type II 2nd-degree AV block, the PR interval remains constant. Beats are intermittently nonconducted and QRS complexes dropped, usually in a repeating cycle of every 3rd (3:1 block) or 4th (4:1 block) P wave.
Third Degree AV block: Heart block is complete in 3rd-degree AV block. There is no relationship between P waves and QRS complexes (AV dissociation) in 3rd-degree AV block. The P wave rate is greater than the QRS rate. (P waves 70/min; QRS-ventricular contractions 25-30/min).
In simple and clear terms:
First degree: prolongation of PQ/PR interval but there is always a QRS complex
Second degree: Prolongation of PQ interval, and some QRS complexes are dropped or lost.
Third degree: No relationship between P wave and QRS complex.
This is a 4mins video that explains heart block in simple terms:
https://youtu.be/fEcBY5CsCPQ 93. A person has diabetes mellitus with fasting hyperglycemia of over 7.2 mmol/L. What blood plasma protein allows for retrospective assessment (4-8 weeks before the examination) of glycemia levels?
94. During a surgery for spleen injury, the surgeon needs to isolate an artery that supplies the spleen with blood. What branch of the arterial vessel is it?
Explanation
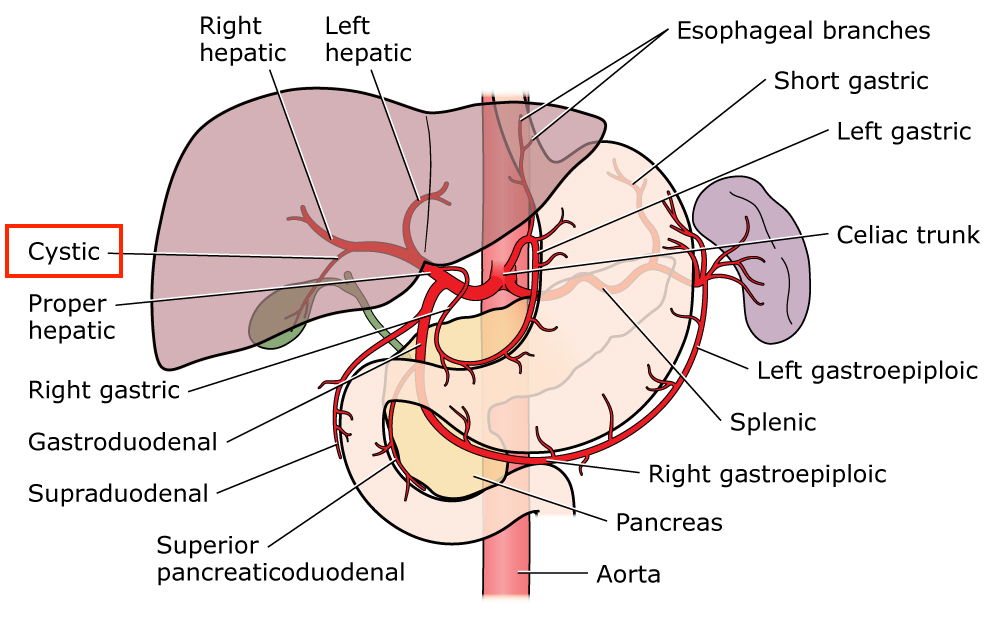
The first major branch of the abdominal aorta, the celiac trunk is responsible for supplying oxygen-rich blood to the stomach, spleen, liver, esophagus, and also parts of the pancreas and duodenum.
The celiac trunk (Truncus coeliacus) classically divides into three major branches:
-
Left gastric artery (A. gastrica sinistra): This artery is responsible for the blood supply to the lesser curvature of the stomach as well as the lower esophagus. It anastomoses with the right gastric artery.
-
Common hepatic artery (A. hepatica communis): This artery, through its many branches, supplies the liver, pylorus of the stomach, gallbladder, duodenum, and the pancreas. Proper hepatic artery (A. hepatica propria) and Gastroduodenal artery (A. gastroduodenalis) are branches of the Common hepatic artery.
-
Splenic artery: This artery offers multiple branches to the upper and middle parts of the greater curvature and fundus of the stomach as well as to the pancreas. This artery ends its course by providing oxygenated blood to the spleen.
95.
During an intense workout, the number of trophic inclusions in the cells of the athlete’s liver and skeletal muscles decreases. What substance belongs to such trophic inclusions?
Explanation
The glycogen granule is essentially an assembly of glucose units (i.e., polymers) that is formed in a branch-like structure via α-glycosidic bonds. As exercise intensity progresses from moderate to high-intensity, muscle glycogenolysis (Glycogenolysis - breakdown of glycogen), liver glycogenolysis and glucose uptake increase such that glucose metabolism predominates. In contrast, there is a reduction in whole body lipid oxidation due to a reduction in both plasma free fatty acids (FFA) and intramuscular triglyceride oxidation.
Starch granules are carbohydrate storage reserves found in plants.
Melanin found in the skin cortex, protects against UV rays. It has no role in energy production for exercise.
Lipofuscin are yellow-brown pigment granules, considered to be one of the aging or "wear-and-tear" pigments, found in the liver, kidney, heart muscle, retina, adrenals, nerve cells, and ganglion cells.
The waste from broken-down oxalate is called oxalic acid. Oxalic Acid Crystals can be dissolved in water for the effective removal of light stains. It has no role in energy production for exercise.
96. A 49-year-old woman developed a leg edema after a long time spent standing. What is the likely cause of edema development?
97. Autopsy of the body of a 40-year-old patient detected groups of enlarged follicles in the small intestine. Their surface has ridges and fissures arranged in a pattern that resembles gyri and sulci of the brain. The follicles protrude above the surface of the intestinal mucosa. On section they are gray red and juicy. Microscopy shows proliferation of monocytes, histiocytes and reticular cells, there are macrophage clusters that form granulomas, while lymphocytes are depleted. What disease can be characterized by these changes?
Explanation
Enteric/Typhoid fever is a life-threatening illness caused by infection with the bacterium Salmonella enterica serotype Typhi (S. typhi), usually transmitted through food and drinks contaminated with fecal matter. It is associated with symptoms that include high fever, fatigue, headache, abdominal pain, diarrhea or constipation, weight loss, and a rash known as \"rose spots.\" Early diagnosis and treatment are important because serious complications, including severe intestinal bleeding or perforation (due to ulcerations), can develop within a few weeks.
They exhibit ileal mucosal hypertrophy caused by a neutrophil-poor monocyte/macrophage-rich hyperplasia. Though diffuse areas were present, much of the lesional proliferation was nodular, representing macrophage infiltration and colonization by the monocytes and macrophages.
Mucosal hypertrophy was described in this question as -surface has ridges and fissures that resembles gyri and sulci of the brain; follicles protrude above the surface of the intestinal mucosa.
For differential diagnosis on microscopy findings:
S. typhi: primarily monocytes, macrophages
Salmonella - Salmonellosis (except Salmonella typhi): predominantly Neutrophils
Shigella - Dysentery: Primarily Neutrophils
Cholera: B Lymphocytes - antibody secreting cells in Peyer’s patches
Amebiasis: Neutrophils
98. General catabolism pathway of biological macromolecules includes besides tricarbonic acid cycle and mitochondrial respiratory chain, the process of pyruvate oxidative decarboxylation. What is the product of pyruvate oxidative decarboxylation?
99. A mountain climber was climbing a mountain for several days. At the altitude of 5000 meters he developed tachypnea, tachycardia and bursting headache. What is the likely cause of these signs?
100. A patient has heart rhythm disturbances. To restore the rhythm, the doctors prescribed the patient calcium antagonists. What effect do calcium ions have on the myocardium?
101. Regional lymph nodes surrounding an infected wound are enlarged. Histological examination shows increased number of macrophages, lymphocytes and lymphatic follicles in the cortical layer of the lymph nodes, as well as large amount of plasma cells. What process in the lymph nodes is indicated by these histologic changes?
102. Autopsy of the body of 6 month old child, who died of sepsis, revealed the absence of thymus and diminished size and weight of the spleen. Microscopy of the spleen detected the absence of periarterial T dependent zones of the follicles and red pulp depletion; In the lymph nodes there is no paracortical zone that is represented mainly by T lymphocytes. B zones in the peripheral immune organs are developed normally. What pathological process is it?
103. A patient was hospitalized into an infectious diseases department. His skin is dry, with low turgor, stool resembles rice water. The patient was diagnosed with cholera. What water-electrolyte imbalance is likely to occur during this disease?
Explanation
Dehydration (hypohydration, hypohydria, exicosis): in dehydration, the extracellular fluid (ECF) and sodium ions are lost.
*Isoosmolar dehydration: based on proportional volume decrease of fluids and electrolytes. Characterised by isotonic loss of both water and solutes from the extracellular fluid e.g. acute renal failure (stage of polyuria), Diarrhea (especially in cholera - there is equal loss of water and electrolytes), blood loss, burns etc.
*Hypoosmolar dehydration (salt deficit) develops due to diarrhea, vomiting, sweating, adrenal insufficiency etc.
*Hyperosmolar dehydration (water deficit) develops due to the loss of the fluid which lacks electrolytes e.g. in diabetes insipidus, hyperventilation
104. In the enlarged cervical lymph node of a 14 year old girl microscopy detected the following: tissue structure of the lymph node is disturbed, no lymphoid follicles, there are sclerotic areas and necrotic foci, cellular composition of the lymph node is polymorphous, there are lymphocytes, eosinophils, large atypical cells with multilobular nuclei (Berezovsky-Reed_sternberg cells) and large mononuclear cells. Make the diagnosis:
105. A 7-year-old girl has signs of anemia. Laboratory testing determined the deficiency of pyruvate kinase in her erythrocytes. In this case the main role in anemia development belongs to the disturbance of a certain process. What process is disturbed in this girl?
106. Biopsy material of a 67-year-old man, who for 17 years has been suffering from chronic bronchitis, shows cylindrical bronchiectasis, the mucous glands have cystic changes, there are patches, where cuboidal epithelium is replaced with stratified squamous epithelium. What pathological process was detected in the bronchial mucosa?
107. A 59-year-old man in a severe condition was hospitalized into the cardiology department with the following diagnosis; acute myocardial infarction in the region of the posterior wall of the left ventricle and septum, initial pulmonary edema development is primary in this patient?
108. A patient developed a purulent inflammatory process in the periodontal tissues. The process was caused by activation of the microorganisms inherent in the body, which are a part of oral mucosal microflora. What type of infection is it?
Explanation
Autoinfection is an infection by a pathogenic agent already within the body or infection transferred from one part of the body to another. With this definition, we can break down the question and arrive at an answer.
The purulent inflammatory process in the periodontal tissues was caused by a microorganism which is a part of the normal oral mucosa. Periodontal disease, also known as gum disease, is a set of inflammatory conditions affecting the tissues surrounding the teeth. So, the pathogenic agent is already within the body, in the oral cavity.
In short, the microorganism didn’t come from outside the body, its part of the normal oral microflora. So, it is a case of self-infection.
Superinfection is infection occurring after or on top of an earlier infection e.g. Hepatitis B patient superinfected by Hepatitis D.
Reinfection: infection by the same organism following an earlier infection.
Relapse is a case of deterioration in someone's state of health after a temporary improvement.
Exogenous (outside): Exogenous infections involve a pathogen entering a patient's body from their environment. These pathogens can be introduced through a contaminated device, healthcare worker, surface, or other vector.
109. A patient suffers from disturbed renal function. To check the filtration ability of the kidneys, he was referred for clearance measurement of the following substance:
110. During emotional excitation the heart rate of a 30-year-old person reached 112/min. The increased heart rate was caused by a change that occurred in a certain structure of the cardiac conduction system. Name this structure:
111.
A 40-year-old man with pulmonary tuberculosis was prescribed isoniazid. Prolonged taking of this drug can result in the development of the following vitamin deficiency:
112. A patient with suppurative bronchitis was hospitalized into the pulmonology department. As a part of complex therapy, he was prescribed a medicine that liquefies sputum and facilitates expectoration. Name this medicine:
113. In an experiment on an isolated squid giant axon submerged in a salt solution, the extracellular potassium ions concentration was increased to the level of the intracellular potassium ions concentration. What changes in the membrane potential will occur in this case?
114. A patient with essential hypertension was prescribed hydrochlorothiazide as a part of complex therapy. What mechanism of drug action facilitates a decrease in blood pressure in this case?
115. A patient is diagnosed with glucocerebroside lipidosis (Gaucher’s disease) that manifests as splenomegaly, liver enlargement, affected bone tissue and neuropathies. What enzyme of complex lipid catabolism is deficient, causing this disease?
116. A patient with Parkinson’s disease made an appointment with the doctor. The doctor prescribed him a medicine that is a dopamine precursor in the central nervous system. What medicine of those listed below has such mechanism of action?
117. During gastric resection the patient received mixed anesthesia with tubocurarine chloride muscle relaxant. To restore unassisted respiration in the patient, the patient was given proserin. What pharmacological group does this drug belong to?
118. A patient has a trauma of the knee joint with crushed patella. With such injury, it is likely that the tendon of a certain thigh muscle is damaged. Name this muscle:
119. Mitochondrial destruction is observed in some hereditary diseases (for example, Kearns-Sayre syndrome). What processes can be disturbed, as a result, in the cell?
120. A 36-year-old man developed angina pectoris attacks immediately after a past case of staphylococcal sepsis. Coronarography detected mural thrombosis without signs of atherosclerosis in the left coronary artery. Thrombus formation occurred in the result of damage to the vascular endothelium and release of:
121. T lymphocytes were affected by HIV. In the process, viral enzyme reverse transcriptase (RNA-dependent DNA-polymerase) catalyzed the synthesis of:
122. There is a large amount of glucose oxidation metabolites dissolved in the cytoplasm of myocytes. Name one such metabolite that converts directly into lactate:
123. From the feces of a patient with acute gastroenteritis a pure culture of microorganisms was obtained. The microorganisms are small mobile slightly curved gram-negative bacilli that within 6 hours grow into a light blue film on the 1% alkaline peptone water. Such properties are characteristic of the following microorganisms:
124. A bioterrorist mailed an envelope with a powder that is suspected to contain anthrax causative agent. This envelope can remain dangerous for a long time, because anthrax causative agent:
125.
A 65-year-old woman against the background of chronic heart failure developed secondary hyperaldosteronism. What medicine should be prescribed to increase the patient’s diuresis?
126. When examining a biopsy material obtained from the thyroid gland, the pathologist discovered lymphocyte infiltration of the thyroid tissues and destruction of the parenchymal elements. Diffuse lymphocyte infiltration with lymphoid follicles was detected in the stroma. What is the most likely diagnosis?
127. A patient used an indirect-acting adrenergic agonist to treat rhinitis. After the patient has been putting in the nose drops for several days, the casoconstrictive effect of the drug gradually diminished. Name this phenomenon:
128. A 40-year-old woman on examination presents with intensified basal metabolic rate. What hormone present in excess leads to such condition?
129. Among lymphocytes there is a population of cells that have membrane receptors to IgM, activate in response to certain antigens, reproduce mitotically, differentiate into plasma cells that product antibodies (immunoglobulins). Name these cells:
Explanation
Immune responses have been classified as cellular or humoral. Cellular responses are mediated by T lymphocytes, which recognize and attack their targets directly or indirectly by enlisting the help of other immune cells, while humoral responses are characterized by the production of antibodies by B lymphocytes and their progeny, plasma cells.
When B cells are stimulated, B cells differentiate into plasma cells that produce antibody molecules closely modeled after the receptors of the precursor B cell. Once released into the blood and lymph, these antibody molecules bind to the target antigen (foreign substance) and initiate its neutralization or destruction.
Antibodies, also known as immunoglobulins, are glycosylated protein molecules present on the surface of B cells (surface immunoglobulins) serving as antigen receptors (BCR), or are secreted into the extracellular space where they can bind and neutralize their target antigens. Five isotypes, or classes, of antibodies (IgM, IgD, IgG, IgA, and IgE) exist.
130. The ophthalmologist noticed a purulent discharge from the conjunctiva of a newborn. Microscopy of the smear obtained from the conjunctiva found three a large number of leukocytes, as well as gram-negative bean-shaped diplococci located inside the leukocytes. What is the causative agent of this disease?
131.
A biopsy material was obtained from the arches of the patient’s soft palate due to a suspected tumor (Macroscopy detected an ulcer with the dense floor). In the biopsy material the following was detected: necrosis of the mucosa with infiltration of the submucosal layer by lymphocytes, epithelioid cells, plasma cells and single neutrophils. Notable is the presence of marked endovasculitis and perivasculitis. The described changes are characteristic of:
132. When examining a child, the pediatrician noted that the child presents with delayed physical and mental development. Urinalysis showed an acute increase in the levels of a keto acid that produce qualitative color reaction with ferric chloride. What metabolic disturbance was detected in this case?
Explanation
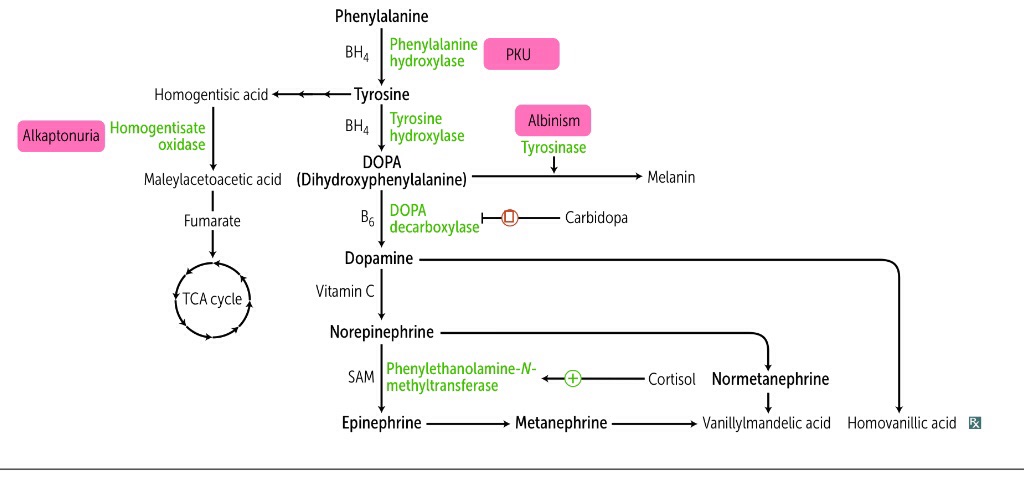
Phenylketonuria (PKU) is an autosomal recessive inborn error of phenylalanine metabolism resulting from deficiency of phenylalanine hydroxylase. Untreated PKU is associated with an abnormal phenotype which includes growth failure, poor skin pigmentation, microcephaly, seizures, global developmental delay and severe intellectual impairment.
When this enzyme is deficient, abnormally high levels of phenylalanine accumulate in the blood and other tissue fluids, and it is the excess of phenylalanine which is held to be responsible, directly or indirectly, for the progressive cerebral damage in the untreated patient. Some of the phenylalanine is excreted unchanged in the urine and the remainder as a variety of breakdown products. Among them is phenylpyruvic acid, and this causes the characteristic greenish-blue colour reaction when a few drops of a solution of ferric chloride are added to the urine.
Alkaptonuria: enzyme deficiency is homogentisic dioxygenase (HGD), which is used to break down a toxic substance called homogentisic acid. When there is a deficiency of this enzyme, homogentisic acid builds up in your body. Affected individuals may have dark urine or urine that turns black when exposed to air - this is not a ferric chloride reaction. (Phenylketonuria is involved in colour change on exposure to ferric chloride, not Alkaptonuria).
Albinism: Enzyme deficiency is Tyrosinase, which synthesizes melanin from the amino acid tyrosine.
Tyrosinemia: enzyme deficiency is fumarylacetoacetate hydrolase (FAH), which is needed for the final breakdown of the amino acid tyrosine.
Cystinuria is an inherited disease that causes stones made of the amino acid cystine to form in the kidneys, bladder, and ureters. The mutations result in the abnormal transport of cystine in the kidney and this leads to the symptoms of cystinuria.
133. The patient’s ECG shows that in the second standard lead from the extremities the P waves are positive, their amplitude is 0.1 mV (norm is 0.05-0.25 mV), duration – 0.1 seconds (norm is 0.07-0.10 seconds). It can be concluded that the following process occurs normally in the cardiac atria:
134.
Some adults develop signs of dyspepsia after drinking milk. What enzyme deficiency is associated with milk intolerance?
135. A young woman, a foreign student from Tehran, has made an appointment with the urologist. She complains of the sensation of heaviness in her lower abdomen and a small amount of blood being excreted with urine at the end of each urination. Microscopy of urine detects the presence of parasite eggs, approximately 140×70 micron in size, with a terminal spike. What diagnosis can be made by the infectious disease specialist?
136. Examination of a patient, who for a long time was taking glucocorticoids, detected lymphopenia. How can the functional state of the patient’s immune system be characterized?
Explanation
Secondary immunodeficiencies are far more common than primary immunodeficiencies. Primary immunodeficiencies are caused by genetic defects affecting cells of the immune system. Secondary or acquired immunodeficiencies arise from a number of conditions, such as treatment with glucocorticoids and immunomodulatory drugs, surgery and trauma, extreme environmental conditions, and chronic infections, such as those caused by HIV.
Glucocorticoids have a strong immunosuppressive, anti-inflammatory and anti-allergic effects on immune cells, tissues and organs. In general, glucocorticoids inhibit leukocyte traffic and thereby the access of leukocytes to the site of inflammation. Furthermore, glucocorticoids interfere with immune cell function and suppress the production and actions of humoral factors involved in the inflammatory process.
Lymphopenia occurs in response to endogenous or exogenous glucocorticoids. This appears to result in part from the sequestration of lymphocytes in lymphoid organs, including bone marrow. Glucocorticoids also potentiate apoptosis of sensitive lymphocytes.
137.
Autopsy of the body of a 1.5 year old child revealed hemorrhagic skin rashes, moderate hyperemia and edema of the nasopharyngeal mucosa, small hemorrhages in the mucosa and internal organs, markedly dystrophic changes in the liver and myocardium, acute necrotic nephrosis and massive hemorrhages in the adrenal glands. These changes are characteristic of the following disease:
Explanation
Meningococcal infection is an acute infectious process which has three main forms: nasopharyngitis, purulent meningitis and meningococcemia. This is characterized by periodic epidemics, the disease is more common in children under 5 years, but the disease may occur in persons of any age.
Meningococcal nasopharyngitis is characterized by catarrhal inflammation of the mucosa with marked hyperemia, edema of the posterior wall of the pharynx and hyperplasia of lymphatic follicles.
Meningococcemia: Changes on the organs are characterized by generalized damage of microcirculation, skin rash, changes in the joints, vascular membrane of the eyes, pericardium, adrenal glands and kidneys. The rash is hemorrhagic, star-like, located mainly on the buttocks and lower extremities. Focal necrosis and hemorrhages or bilateral massive hemorrhages with the development of acute adrenal insufficiency (Waterhouse Friderichsen syndrome) are noted in the adrenals. Necrosis of nephrothelium of the tubules (necrotic nephrosis) is observed in the kidneys. The death of the patients is caused by bacterial shock, its severity is aggravated by hemorrhages to the adrenals; acute renal insufficiency is not so common (in the adults).
138.
Immediately after moving from horizontal to vertical position, the heart rate of a 23-year-old man increased by 15 beats per minute, his systolic pressure remained unchanged, while his diastolic pressure increased by 10 mmHg. What reflex response of the executive structures caused this increase in the diastolic pressure?
139. The patient’s ECG was obtained. What element of ECG allows the doctor to assess the spread of atrial depolarization processes?
Explanation
An electrocardiogram, or ECG, is a recording of the heart’s electrical activity as a graph over a period of time. A typical ECG tracing of the cardiac cycle (heartbeat) consists of a P wave (atrial depolarization), a QRS complex (ventricular depolarization), and a T wave (ventricular repolarization).
The first wave on an ECG is the P wave, indicating atrial depolarization in which the atria contract (atrial systole). The QRS complex refers to the combination of the Q, R, and S waves, and indicates ventricular depolarization and contraction (ventricular systole).The T Wave indicates ventricular repolarization, in which the ventricles relax following depolarization and contraction.
[caption id="attachment_1118" align="aligncenter" width="728"]

P-wave indicates Atrial depolarization, QRS complex- ventricular depolarization, T-wave- ventricular repolarization.[/caption]
140. A 32-year-old man has tall stature, gynecomastia, female pattern of hair distribution, high pitched voice, delayed mental development and sterility. He was provisionally diagnosed with Klinefelter syndrome. To clarify this diagnosis, it is necessary to analyze the patient’s:
141. A patient with myocardial infarction has acute heart failure. Among the drugs that increases the force of heart contractions the least dangerous in this case will be:
Explanation
Dobutamine is a catecholamine with β-1 and β-2 adrenergic agonist properties which help improve myocardial contractility. In patients with cardiogenic shock due to decompensated heart failure, dobutamine decreases left ventricular end-diastolic pressure and raises blood pressure by increasing cardiac output. It does all these with little effect on heart rate or systemic arterial pressure.
Adrenaline (Epinephrine) can increase the heart rate, contractility and increase blood flow to the heart. However, it also causes constriction of small blood vessels which can reduce blood flow to other organs, including the brain, and may lead to neurological damage.
Caffeine can act on enzymes in the heart that stimulate the intensity of the heart's contractions. Caffeine can facilitate the release of natural hormones that act on the heart to release norepinephrine, which can produce a stimulated effect similar to that of adrenaline.
Aminophylline can cause increased or rapid heart rate, irregular heartbeat, seizures, and skin rash.
Isoprenaline has been shown to cause impairment in perfusion of the subendocardial myocardium resulting in isoprenaline-induced myocardial necrosis.
Of all the answer choices given, Dobutamine is the best and the drug with the least adverse effect profile. Epinephrine and other vasoconstrictors (caffeine, Isoprenaline) are strictly contraindicated for patients recovering from myocardial infarction supported by the fact that after a myocardial infarction, higher risk of reinfarction is reported.
142. To treat the burns, a patient was prescribed a drug with antiseptic properties that are based on formation of atomic oxygen in the presence of organic substances. This drug has also an astringent(anti-inflammatory) effect due to formation of albuminates. Name this drug:
143. A man with caisson disease died with the signs of acute disturbances of cerebral circulation in the basin of a. meningea media in the left-brain hemisphere. Autopsy detected in this area a focus of gray cerebral softening 6x7x3.4 cm in size. What is the character of the process that caused the death of the patient?
144.
A patient with essential hypertension, who is taking hypothiazide (hydrochlorothiazide) treatment, complains of general weakness, loss of appetite and palpitations. He has muscle hypotonia, flaccid paralyses and decreased intestinal peristalsis. What can be the cause of this condition?
Explanation
Most widely recognized, the first adverse effect of thiazide diuretics is hypokalemia. Hypokalemia can be life-threatening and requires monitoring during the first 2-3 weeks of Hydrochlorothiazide therapy.
Thiazide diuretics reduces potassium concentration in blood through two indirect mechanisms: inhibition of sodium-chloride symporter at distal convoluted tubule of a nephron and stimulation of aldosterone that activates Na+/K+-ATPase at collecting duct.
A low potassium level can make muscles feel weak (muscle hypotonia), cramp, twitch, or even become paralyzed, and abnormal heart rhythms may develop; Digestive Problems, Weakness and Fatigue.
Thiazide diuretics can also cause hyponatremia, hyperuricemia, hypercalcemia and hyperglycemia. However, it doesn’t cause hyperkalemia.
Hyponatremia: seizures, confusion, headache, irritability.
Hyperuricemia: can eventually lead to gout.
Hypercalcemia: frequent urination, thirst, lethargy, depression, memory loss or irritability.
145. Mother of a 2-year-old child made an appointment with the dentist. She complains of teeth destruction in her child. Examination shows that the milk teeth of the child are deformed, carious and have a brown border at their cervices. Medical history of the mother revealed that during her pregnancy she had been taking antibiotics without the doctor’s prescription. What group of antibiotics with the most marked teratogenic effect was likely taken by the mother?
146. A patient has disturbed vision in the lateral visual fields of both eyes (bilateral hemianopsia). What nerve structure is affected?
147. A 28-year-old woman came to a polyclinic with complaints of a headache. The doctor offered her paracetamol, taking into consideration that the woman has a somatic disease. What concomitant disease made it necessary to prescribe her specifically paracetamol?
148. Due to a trauma, the posterior roots of the spinal cord of a 40-year-old man were destroyed. What disorders will be observed in the innervation region of these roots?
149. A 16-year-old young man complains of itching between the fingers and on his abdomen that intensifies at night. Examination detects thin gray streaks and fine rash on his skin. What is the most likely causative agent of this disease?
150. A 35-year-old woman has a history of 2 strokes. Her biochemical blood analysis shows increased levels of antiphospholipid autoantibodies. Target phospholipids in this case include:
Explanation
The antiphospholipid syndrome is a disorder of the immune system that is characterized by excessive clotting of blood and/or certain complications of pregnancy (premature miscarriages, unexplained fetal death, or premature birth) and the presence of antiphospholipid antibodies (such as anti-cardiolipin or lupus anticoagulant antibodies) in the blood. Clotting disorders associated with antiphospholipid syndrome include stroke, blood clots deep within the legs (deep venous thrombosis) and clots in the lungs (pulmonary embolism).
Antiphospholipid syndrome (APS) is an autoimmune disorder. Signs and symptoms vary, but may include blood clots, miscarriage, rash, chronic headaches, dementia, and seizures. APS occurs when your body's immune system makes antibodies that attack phospholipids.
Due to the increased incidence of blood clot formation in patients with Antiphospholipid syndrome, they are at increased risk of having stroke. Antiphospholipid antibody was considered to be a risk factor of stroke, especially in SLE and/or young female patients.