1.
While examining foot blood supply a doctor checks the pulsation of a large artery running in the separate fibrous channel in front of articulatio talocruralis between the tendons of long extensor muscles of hallux and toes. What artery is it?
2.
A comminuted fracture of infraglenoid tubercle caused by shoulder joint injury has been detected during X-ray examination of a patient. What muscle tendon attached at this site has been damaged?
3.
A 42-year-old male with a lesion of the ulnar nerve is unable to flex the II and V fingers to the midline. Which muscle function is impaired in this case?
4. After a craniocerebral injury a patient is unable to recognize objects by touch. What part of brain has been damaged?
5.
As a result of a continuous chronic encephalopathy, a patient has developed spontaneous motions and a disorder of torso muscle tone. These are the symptoms of the disorder of the following conduction tract:
6.
As a result of a craniocerebral injury, a patient has a decreased skin sensitivity. What area of the cerebral cortex is likely to be damaged?
7.
A 40-year-old patient has ulcer perforation in the posterior wall of stomach. What anatomical structure will blood and stomach content leak to?
8.
Angiocardiography of a 60-year-old male patient revealed constriction of a vessel located in the left coronary sulcus of the heart. What is the pathological vessel called?
9.
A patient complains of pain in the right lateral abdomen. Palpation revealed a dense, immobile, tumor-like formation. A tumor is likely to be found in the following part of the digestive tube:
Explanation
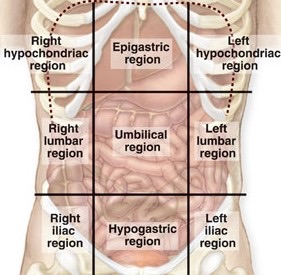

Anterolateral abdominal wall has 9 regions and 4 quadrants (RUQ, LUQ, RLQ, LLQ)
· Right lateral abdominal region: Ascending colon (colon ascendens), right kidney, right ureter and loops of small intestine.
· Umbilical region: Transverse colon (colon transversum), head of pancreas, duodenum (except superior part)
· Left lateral abdominal region: Descending colon (colon descendens), left kidney, left ureter and loops of small intestine.
· Left inguinal region: Sigmoid colon (colon sidmoideum), left ureter, left external iliac artery of artery and vein.
· Right Inguinal region: Caecum, vermiform appendix, right ureter
10.
A female patient has facial neuritis that has caused mimetic paralysis and hearing impairment. Hearing impairment results from the paralysis of the following muscle:
11. The receptors under study provide transfer of information to the cortex without thalamic involvement. Specify these receptors:
12. During an animal experiment, surgical damage of certain brain structures has caused deep prolonged sleep. What structure is most likely to cause such condition, if damaged?
13.
A patient complains of acute pain attacks in the right lumbar region. During examination the nephrolithic obturation of the right ureter in the region between its abdominal and pelvic segments has been detected. What anatomical boundary exists between those two segments?
14. As a result of past encephalitis, a male patient has developed an increase in cerebrospinal fluid pressure in the right lateral ventricle. What can be the cause of this condition?
15. A male patient complains of skin
insensitivity of inferior eyelid, external lateral surface of nose and upper lip. A doctor in the course of examination has revealed inflammation of the second branch of trigeminal nerve. What cranial foramen does this branch go through?
16.
A patient with suspected tumor of lung had been admitted to the oncological department. Examination revealed localised pathology in the inferior lobe of the left lung. How many bronchopulmonary segments does this lobe have?
17. As a result of an injury, the integrity of the anterior spinal cord root was broken. Specify the neurons and their processes that had been damaged:
18. During the air and bone conduction tests it was revealed that in the left ear the tones were louder by bone conduction. This might be associated with the disease of:
19.
In course of invasive abdominal surgery a surgeon has to locate the origin of the mesenteric root. Where is it normally localized?
20. As a result of a road accident a 37-year-old female victim developed urinary incontinence. What segments of the spinal cord had been damaged?
21. During a surgery for femoral hernia a surgeon operates within the boundaries of femoral trigone. What structure makes up its upper margin?
22.
A 19-year-old victim has been delivered to the casualty department with a cut wound of the trapezius muscle. Which of the cervical fasciae forms a sheath for this muscle?
23.
A 29-year-old male with a knife wound of neck presents with bleeding. During the initial debridement of the wound the surgeon revealed the injury of a vessel found along the lateral edge of the sternocleidomastoid muscle. Specify this vessel:
24.
A patient has been found to have a marked dilatation of saphenous veins in the region of anterior abdominal wall around the navel. This is symptomatic of pressure increase in the following vessel:
25.
As a result of an injury a patient cannot extend his arm at the elbow. This may cause abnormal functioning of the following muscle:
26.
A casualty has a fracture in the region of the inner surface of the left ankle. What is the most likely site for the fracture?
27. A patient consulted a doctor about being unable to abduct his right arm after a past trauma. Examination revealed that the passive movements were not limited. The patient was found to have the atrophy of the deltoid muscle. What nerve is damaged?
28.
After a trauma of the upper third of the anterior forearm a patient exhibits difficult pronation, weakening of palmar flexor muscles and impaired skin sensitivity of 1-3 fingers. Which nerve has been damaged?
29. On examination a patient was found to have medial strabismus, the inward deviation of the eyeball and inability to abduct the eyeball outwards. What nerve is damaged?
30.
As a result of an injury of the knee joint a patient shows a drawer sign, that is the anterior and posterior displacement of the tibia relative to the femur. What ligaments are damaged?
31.
Examination of a patient with ischemic heart disease revealed the impaired venous blood flow in the territory of the cardiac vein running in the anterior interventricular sulcus of heart. What vein is it?
32. For the direct injection of medications into the liver surgeons use the round ligament of liver. This manipulation involves bougienage (lumen dilatation) of the following vessel:
33.
After the diagnostic tests a 40-year- old male has been referred for the lymphography of the thoracic cavity. The surgeon revealed that the tumor had affected an organ whose lymphatic vessels drain directly into the thoracic duct. Specify this organ:
34. After a car accident a 23-year-old male presented to the hospital with a cut wound of the anteromedial region of shoulder and arterial bleeding. Which artery was damaged?
35.
During the operation on the small intestine the surgeon revealed an area of the mucous membrane with a single longitudinal fold among the circular folds. Which portion of the small intestine is this structure typical for?
36. A surgeon examined the patient and found the injury of the upper third of the kidney. Considering the syntopy of the left kidney, the intactness of the following organ should be checked at the same time:
37.
After resection of the middle third of the femoral artery obliterated by a thrombus the limb is supplied with blood through the bypasses. What artery plays the main part in the restoration of the blood flow?
38.
A patient has been hospitalized for a suspected tumor of the prostate. During the surgery, it was revealed that the tumor invaded the bladder. Which part of the bladder was affected?
39. A casualty with an injury of the temporal region has been diagnosed with epidural hematoma. Which of the arteries is most likely to be damaged?
40.
When examining a patient, the doctor revealed a tumor of the bronchus which borders on the aorta. Which bronchus is affected?
41.
A patient has a right-sided fracture in the region of the frontal third of mandible accompanied by a haematoma in the region of chin. It is caused by the injury of the following artery:
42.
As a result of a cold a patient has the abnormal pain and temperature sensitivity of the frontal 2/3 of his tongue. Which nerve must have been damaged?
43.
After a trauma of soft tissues in the region of the posterior surface of medial condyle of humerus a patient has got a skin prickle of medial forearm surface. Which of the listed nerves is located in the affected region?
44. A boy has fallen down from a tree. Now he finds it difficult to abduct his arm into horizontal position. Which muscle is most likely to be injured?
45.
A 28 year old woman has been diagnosed with extrauterine pregnancy complicated by the fallopian tube rupture. The blood is most likely to penetrate the following peritoneal space:
46.
A 70 year old female patient was diagnosed with fracture of left femoral neck accompanied by disruption of ligament of head of femur. The branch of the following artery is damaged:
47.
As a result of a trauma a patient has damaged anterior roots of spinal cord. What structures have been affected?
48. During cytoscopy mucous membrane of urinary bladder normally makes folds except for a single triangular area with smooth mucosa. This triangle is located in the following part of urinary bladder:
49. A surgeon has to find the common hepatic duct during the operative intervention on account of concrements in the gall ducts. The common hepatic duct is located between the leaves of:
50.
A patient complains about impaired evacuatory function of stomach (long-term retention of food in stomach). Examination revealed a tumour of initial part of duodenum. Specify localization of the tumour:
51.
In course of an operation surgeon removed a part of a lung that was ventilated by a tertiary bronchus accompanied by branches of pulmonary artery and other vessels. What part of a lung was removed?
52.
While playing a child got a punch in the presternum region. As a result of this trauma an organ located behind the presternum was damaged. Name this organ:
53.
A patient has been diagnosed with a compression fracture of a lumbar vertebra. As a result he has a considerable increase in curvature of the lumbar lordosis. Which ligament damage can induce such changes in the spine curvature?
54.
In order to prevent massive hemorrhage in the region of oral cavity floor it is required to ligate an artery which is located within Pirogov’s triangle. What artery is it?
55.
Examination of a 6-month-old child revealed a delay in closure of the occipital fontanelle. When should it normally close?
56.
A man with a stab wound in the region of the quadrilateral foramen consulted a doctor about it. Examination revealed that the injured couldn’t abduct his arm from the body. What nerve is most likely damaged?
57. A victim of an accident has bleeding from the soft tissues anteriad the mandibular angle. Which vessel should be ligated for the bleeding arrest?
58.
A 38-year-old patient came to a traumatology centre and complained about an injury of his right hand. Objectively: the patient has a cut wound in the region of the thenar eminence on the right hand; distal phalanx of the I finger cannot be flexed. What muscle was injured?
59.
An 18-year-old man was delivered to the hospital after a road accident. Examination at the traumatological department revealed multiple injuries of soft tissues of face in the region of the medial eye angle. The injuries caused massive hemorrhage. What arterial anastomosis might have been damaged in this region?
60. A weightlifter has a disruption of thoracic lymphatic duct as a result of lifting a weight. Choose the most likely site of injury:
61. A woman suffering from osteochondrosis has acute pain in her humeral articulation that gets worse when she tries to abduct her shoulder. These symptoms might be caused by damage of the following nerve:
62. A patient consulted a doctor about loss of taste sensitivity on the tongue root. The doctor revealed that it is caused by nerve affection. Which nerve is it?
63.
An older woman has been hospitalised for acute pain and edema of the right hip joint that appeared after a fall. Objectively: the hip is adduced inwards, hip joint movements are impaired. The patient is most likely to have a fracture of the following bone or bone part:
64. While performing an inguinal canal operation on account of hernia a surgeon damaged the canal\\\\\\\'s contents. What exactly was damaged?
65.
Surgical approach to the thyroid gland from the transverse (collar) approach involves opening of interaponeurotic suprasternal space. What anatomic structure localized in this space is dangerous to be damaged?
66.
An injured person was delivered to the hospital with a penetrating wound in the left lateral region of abdomen. What part of the large intestine is most likely damaged?
Explanation

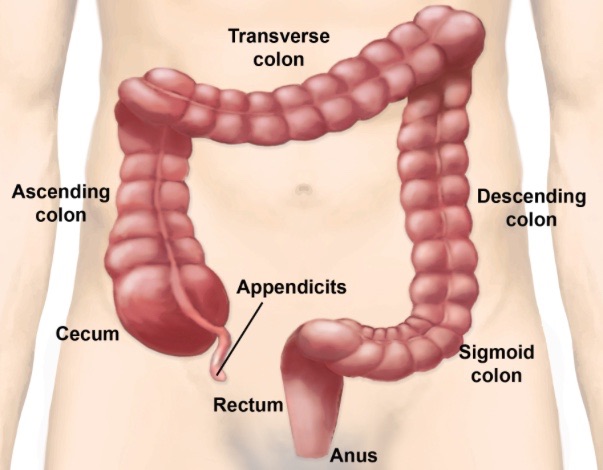
Anterolateral abdominal wall has 9 regions and 4 quadrants (RUQ, LUQ, RLQ, LLQ)
· Right lateral abdominal region: Ascending colon (colon ascendens), right kidney, right ureter and loops of small intestine.
· Umbilical region: Transverse colon (colon transversum), head of pancreas, duodenum (except superior part)
· Left lateral abdominal region: Descending colon (colon descendens), left kidney, left ureter and loops of small intestine.
· Left inguinal region: Sigmoid colon (colon sidmoideum), left ureter, left external iliac artery of artery and vein.
· Right Inguinal region: Caecum, vermiform appendix, right ureter
67. In course of laparotomy a surgeon revealed gangrenous lesion of descending colon. It was caused by thrombosis of the following artery:
68.
Inflammation of the tympanic cavity (purulent otitis media) was complicated by inflammation of mammillary process sockets. What wall of tympanic cavity did the pus penetrate into the sockets through?
69.
A patient caught a cold after which there appeared facial expression disorder. He cannot close his eyes, raise his eyebrows, bare his teeth. What nerve is damaged?
70.
A patient complained about being unable to adduct and abduct fingers in the metacarpophalangeal articulations towards and away from the 3rd finger. Which muscles’ function is impaired?
71. A patient has difficulties with hand movement. Examination revealed inflammation of common synovial sheath of flexor muscles. It is known from the patient’s anamnesis that he got a stab wound of finger a week ago. Which finger was most probably damaged?
Explanation
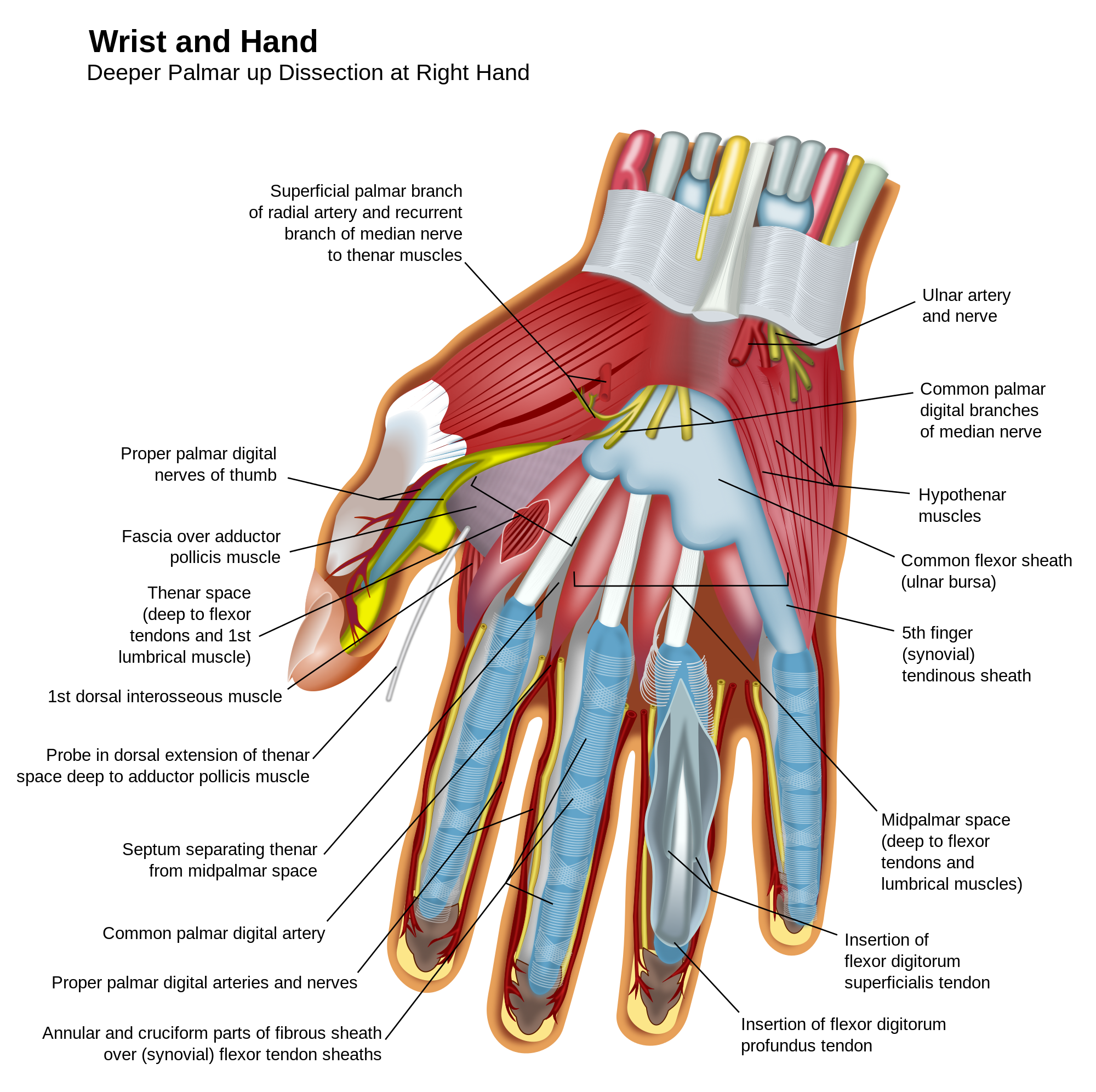
There are nine flexor tendons in the carpal tunnel. The flexor tendons of the fingers, the flexor digitorum superficialis (FDS) and flexor digitorum profundus (FDP), are arranged in the carpal tunnel, superficial and deep respectively and continue distally in pairs to each finger except the thumb. They are invested by a common tendon sheath that starts proximal to the carpal tunnel and extends to within 5mm of the insertion of the profundus tendon on the distal phalanx. A separate ulnar bursa envelops the flexor tendons of the little finger (digiti minimus). The other tendon in the carpal tunnel is the flexor tendon of the thumb, flexor pollicis longus, which has a separate synovial covering the radial bursa. There is a gap between ulnar bursa and the synovial sheaths of the index, long (digiti medius), and ring (digiti anularis) fingers in the distal palm of the hand, therefore inflammation cannot spread to this 3 fingers directly from the common synovial sheath.
The flexor pollicis longus is surrounded by the radial bursa, which extends distally. The other flexor tendons are surrounded by the ulnar bursa, which extends to the little finger (digiti minimus). Note the gap between this bursa and the synovial sheaths of the 2nd, 3rd and 4th fingers. The little finger will most probably be damaged.
72. Examination of a newborn boy’s genitalia revealed an urethral hiatus that opens on the undersite of his penis. What malformation is it?
73. A patient with cholelithiasis fell ill with mechanic jaundice. Examination revealed that the stone was in the common bile duct. What bile-excreting ducts make up the obturated duct?
74. Examination of a patient revealed hypertrophy and inflammation of lymphoid tissue, edema of mucous membrane between palatine arches (acute tonsillitis). What tonsil is normally situated in this area?
75.
Examination of a patient with impaired blood coagulation revealed thrombosis of a branch of inferior mesenteric artery. What bowel segment is damaged?
76.
Roentgenological examination of skull base bones revealed enlargement of sellar cavity, thinning of anterior clinoid processes, destruction of different parts, destruction of different parts of sella turcica. Such bone destruction might be caused by a tumour of the following endocrinous gland:
77.
A patient was admitted to the surgical department with inguinal hernia. During the operation the surgeon performs plastic surgery on posterior wall of inguinal canal. What structure forms this wall?
78.
A patient was diagnosed with paralysis of facial and masticatory muscles. The haematoma is inside the genu of internal capsule. What conduction tract is damaged?
79.
A foreign body (a button) closed space of the right superior lobar bronchus. What segments of the right lung won’t be supplied with air?
80. A patient was diagnosed with bartholinitis (inflammation of greater vulvovaginal glands). In which organ of urogenital system are these glands localized?
81.
Ultrasonic examination of a patient revealed aneurism in the area of aortic arch that caused alteration of vocal function of larynx. What nerve was constricted?
82.
In course of an experiment thalamocortical tracts of an animal were cut. What type of sensory perception remained intact?
83. Examination of a 2-year-old child revealed physical developmental lag, the child often has pneumonias. The child was diagnosed with nonclosure of ductus arteriosus. Haemodynamics disorder was caused by the intercommunication of the following vessels:
84.
It is necessary to take the cerebrospinal fluid from a patient with suspected inflammation of brain tunics. Diagnostic puncture was performed between the arches of the lumbar vertebras. During the puncture the needle went through the following ligament:
85.
A 53-year-old female patient was diagnosed with liver rupture resulting from a blunt abdominal injury. The escaped blood will be assembled in the following anatomic formation:
86.
A patient complains about edemata of legs, skin cyanosis, small ulcers on one side of the lateral condyle. Examination revealed a swelling, enlarged veins, formation of nodes. The pathological process has started in the following vein:
87. During an experiment the dorsal roots of the spinal cord of an animal have been cut. What changes will be observed in the innervation zone?
88.
A young man complains about urination disorder. Examination of the external genitals revealed that the urethra was split and urine could flow out of this orifice. What anomaly of the external genitals development is it?
89. A man suffering from osteochondrosis got acute pain in the abdominal muscles (lateral and anterior). During objective examination a physician diagnosticated increased pain sensitivity of skin in the hypogastric region. This pain might be caused by affection of the following nerve:
90.
A man with an injury in the nuchal region (regio nuchae) was admitted to the resuscitation department. What muscle occupies this region?
91. A patient has lost skin sensitivity in the region of the medial surface of his shoulder. This is the result of dysfunction of the following nerve:
92.
After a road accident a driver was delivered to the hospital with an injury of the medial epicondyle of humerus. What nerve might be damaged in this case?
93.
A woman underwent an operation on account of extrauterine (tubal) pregnancy. In course of the operation the surgeon should ligate the branches of the following arteries:
94. A 6 month old baby ill with bronchitis was taken for an X-ray of chest. Apart of changes associated with bronchi the X-ray film showed a shadow of thymus gland. What might have caused such changes?
95.
A 35 year old man with a trauma of his left hand was admitted to the traumatology department. Objectively: cut wound of palmar surface of left hand; middle phalanxes of II–V fingers don’t bend. What muscles are damaged?
96.
A patient was admitted to the surgical department with suspected inflammation of Meckel’s diverticulum. What part of bowels should be examined in order to discover the diverticulum in course of an operation?
97.
The cerebrospinal fluid is being examined for the purpose of differential meningitis diagnostics. At what site is the lumbar puncture safe?
98. A patient has a deep cut wound on the posterior surface of his shoulder in its middle third. What muscle might be injured?
99.
While performing an operation in the area of axillary crease a surgeon has to define an arterial vessel surrounded by fascicles of brachial plexus. What artery is it?
100.
In course of a small pelvis operation it became necessary to ligate an ovarian artery. What formation may be accidentally ligated together with it?
101.
A patient with a knife wound in the left lumbar part was delivered to the emergency hospital. In course of operation a surgeon found that internal organs were not damaged but the knife injured one of muscles of renal pelvis. What muscle is it?
102.
A man with cut wound of his right foot sole was admitted to the hospital ward. The patient has limited elevation of the lateral foot edge. In course of wound management the injury of a muscle tendon was revealed. What muscle is injured?
103. A patient with neuritis of femoral nerve has disturbed flexion of thigh as well as disturbed crus extension in the knee joint. What muscle’s function is disturbed?
104. An injured man has bleeding from branches of carotid artery. For a temporary arrest of bleeding it is necessary to press the carotid artery to the tubercle of a cervical vertebra. Which vertebra is it?
105.
As a result of an accident a patient has intense painfulness and edema of the anterior crus surface; dorsal flexion of foot is hindered. Function of which crus muscle is most likely to be disturbed?
106.
After a 2 y.o. child has had flu, there appeared complaints about ear ache. A doctor revealed hearing impairment and inflammation of the middle ear. How did the infection penetrate into the middle ear?
107. A patient’s knee joint doesn’t extend,
there is no knee-jerk reflex, skin sensitivity of the anterior femoral surface is disturbed. What nerve structures are damaged?
108.
A 70 y.o. man has cut an abscess off in the area of mammiform process during shaving. Two days later he was admitted to the hospital with inflammation of arachnoid membranes. How did the infection penetrate into the cavity of skull?
109. In case of a penetrating wound of
the anterior abdominal wall the wound tract went above the lesser curvature of stomach. What peritoneum formation is most likely to be injured?
110.
After a trauma a 44-year-old patient had a rupture of left palm muscle tendons and of the superficial blood vessels. After operation and removal of the most part of the necrotically changed muscle tissue the bloodstream was normalized. What vessels have helped to restore the bloodstream?