1. A 32-year-old welder complains of weakness and fever. His illness initially presented as tonsillitis one month earlier. On examination: body temperature - 38,9oC, RR24/min., HR- 100/min., BP- 100/70 mm Hg, hemorrhages on the legs, enlargement of the lymph nodes. Complete blood count: Hb- 70 g/l, RBC- 2, 2 · 1012/l, WBC- 3, 0 · 109/l with 32% of blasts, 1% of eosinophils, 3% of band neutrophils, 36% of segments, 20% of lymphocytes, and 8% of monocytes, ESR- 47 mm/hour. What is the cause of anemia?
2. A 54-year-old woman takes antihypertensive drugs for hypertension. Having discovered that her son was arrested and is under investigation, became agitated and extremely anxious. She lost her orientation in place, stopped recognizing her relatives, started hearing ”voices” threatening her and her son with violence. She had opened her window (on the 8th floor) and tried to jump out, resisted the people, who were holding her back. What drugs should be administered to terminate such condition of the patient?
3. A 43-year-old man, who has been abusing alcohol and suffering from pulmonary tuberculosis, in the course of two weeks gradually developed general weakness, headache, diplopia, vomiting. Objectively: ptosis on the left, anisocoria S>D, exotropia of the left eye, neck stiffness; Kernig’s and Brudzinski’s signs are positive. In cerebrospinal fluid: lymphocytic pleocytosis, low glucose, precipitation of cerebrospinal fluid resulted in production of fibrin film. What is the most likely diagnosis?
4. A 32-year-old woman complains of episodes of intense fear that occur without visible cause and last for 10-20 minutes; the episodes are characterized by rapid pulse, sweating, labored breathing, and vertigo. Specify the likely diagnosis:
5. A resuscitation unit received a 46-yearold woman, who has been suffering from diabetes mellitus type 1 for approximately 30 years. Objectively: the skin is pale, heart sounds are weakened, BP is 170/100 mm Hg, lower limbs are markedly swollen. Blood creatinine - 1125 mcmol/l, urea - 49,6 mmol/l, potassium - 6.3 mmol/l, glucose - 7,6 mmol/l, glomerular filtration rate - 5 ml/min. What treatment is indicated for the patient in the first place?
6. A woman is on the 32nd week of her second pregnancy. She complains of fever, chills, nausea, vomiting, lumbar pain, and dysuria. Costovertebral angle tenderness is present on both sides. Urine analysis: pyuria, bacteriuria. Blood test: leukocytosis. What is the most likely diagnosis?
7. A 19-year-old young man complains of cough with expectoration of purulent sputum in amount of 100 ml per day, hemoptysis, dyspnea, increased body temperature up to 37,8oC, general weakness, weight loss. The patient’s condition lasts for 4 years. Exacerbations occur 2-3 times a year. The patient presents with malnutrition, pale skin, cyanosis of the lips, drumstick (clubbed) fingers. Tympanic percussion sound in the lungs, weakened respiration, various numerous moist crackles in the lower pulmonary segments on the left can be observed. In blood: erythrocytes - 3, 2 · 1012/l, leukocytes - 8, 4 · 109/l, ESR- 56 mm/hour. On X-ray: lung fields are emphysematous, the left pulmonary root is deformed and dilated. What is the most likely diagnosis?
8. A 37-year-old man working as a typesetter in a print shop complains of rapid fatigability, paroxysmal attacks of stomachache, weak drooping hands. Examination of neurological status revealed hypotrophy of the forearm muscles. Carporadial reflexes are sharply weakened. Sensitivity is not disturbed. Gums present with dark blue border. What neurological pathology is it?
9. A 48-year-old woman has been hospitalized due to development of tachysystolic atrial fibrillation. She has lost 5 kg of body weight within 2 months. On palpation there is a node in the left lobe of the thyroid gland. What pathology resulted in the development of this condition?
10. On the 9th day after childbirth the obstetric patient developed high fever up to 38oC. She complains of pain in the right mammary gland. On examination a sharply painful infiltrate can be palpated in the right mammary gland, the skin over the infiltrate is red, subareolar area and nipple are swollen and painful. What is your diagnosis?
11. A 36-year-old woman complains of pain in her lumbar area, which irradiates to her lower right limb and increases during movements, and sensation of numbness in her limb. Objectively: palpation of the shin and thigh muscles is painful, positive stretch symptom on the right. MRI scan: herniation of intervertebral disk L5-S1 4 mm in size. What is the most likely diagnosis?
12. During routine medical examination a 35-year-old woman presents with enlarged cervical and mediastinal lymph nodes. Her overall health is satisfactory. ESR is 30 mm/hour. Cervical node biopsy was performed. In the specimen there are granulomas composed of epithelial and giant cells, no caseous necrosis detected. What is the most likely diagnosis?
13. A 39-year-old woman complains of violent pain in her left lumbar area with irradiation to the right iliac area. Several years ago she was diagnosed with cholelithiasis and urolithiasis. The patient’s condition is moderately severe, the skin is dry. Ortner’s symptom is negative; costovertebral angle tenderness is observed on the right. The most reasonable treatment tactics would be:
14. An 18-year-old patient complains of skin rash. The patient has been suffering from this condition for 5 years. The first instance of this disease occurred after a car accident. Objectively: the patient presents with papular rash covered in silvery scales, ”thimble” symptom (small pits on the nails), affected joints. What is the most likely diagnosis?
15. A woman complains of frequent, liquid stool (up to 9-10 times per day) with mucus and blood admixtures, dull pain in the hypogastrium, weight loss of 4 kg within the last year. Objectively: malnutrition, dry skin, low turgor, aphthous stomatitis. The stomach is soft, the sigmoid colon is spastic and painful on palpation. Occult blood test is positive. Fibrocolonoscopy: edema, hyperemia, mucosal granulation, pseudopolyps, small ulcers with irregular edges. Make the diagnosis:
Explanation
Occult blood in stool is indicative of a hemorrhagic process from the colon, while the results from the colonoscopy indicates the pathology is located in the colon.
Irritable bowel syndrome is an inflammatory bowel disease characterised by recurrent abdominal cramps (pain), change in form (consistency) and frequency of stool, constipation etc. . This condition is common in middle aged women and is associated with underlying conditions such as stress, anxiety, depression or a previous case of intestinal infection.
Distinguishing Ulcerative Colitis from Crohn Disease
|
Ulcerative Colitis
|
Crohn Disease
|
|
Only colon involved
|
Panintestinal
|
|
Continuous inflammation extending proximally
from rectum
|
Skip-lesions with intervening normal mucosa
|
|
Inflammation in mucosa and submucosa only
|
Transmural inflammation
|
|
No granulomas
|
Noncaseating granulomas
|
|
Perinuclear ANCA (pANCA) positive
|
ASCA positive
|
|
Bleeding (common)
|
Bleeding (uncommon)
|
|
Fistulae (rare)
|
Fistulae (common)
|
16. A 26-year-old woman came to a gynecologist for a regular check-up. She has no complaints. Per vaginum: the uterus lies in anteflexion, not enlarged, dense, mobile, painless. On the left from the uterus in the area of uterine appendages there is a mobile painless outgrowth that can be moved independently from the uterus. On the right the appendages cannot be detected. What additional investigation would be informative for diagnosis clarification?
17. A 57-year-old patient complains of dyspnea at rest. The patient presents with orthopnea, acrocyanosis, bulging cervical veins. On percussion: dull sound over the lower lung segments; on auscultation: no respiratory murmurs. Heart rate is 92/min. Right-sided cardiac dilatation is observed. The liver is enlarged by 7 cm. Shins are swollen. Pleural effusion is suspected. What indicator would confirm the presence of transudate in this case?
18. A 28-year-old woman complains of girdle pain in her epigastric and left subcostal areas with irradiation to the back, nausea, and vomiting without relief. On examination a surgeon observes stomach distension and meteorism. There are positive Mondor’s, Mayo-Robson’s, and Cullen’s symptoms. What is the most likely diagnosis?
19. A 57-year-old patient complains of sensation of dryness and pain during swallowing, frequent unbearable cough, the voice is hoarse. Disease onset was abrupt. On laryngoscopy: laryngeal mucosa is hyperemic, vocal folds are swollen, laryngeal lumen contains viscous secretion. What diagnosis is it?
Explanation
Acute laryngitis is catarrhal inflammation of mucous membrane, sub mucous layer and internal muscles of larynx. Clinical picture involves Feeling of dryness, burning, tickling sensation, A dry, then moist cough, Hoarse voice. The above patient presents with a dry sensation, pain while swallowing, a hyperemic larynx and viscous (purulent ) secretion which confirms an acute laryngitis ( chronic form typically lasts more than 3 weeks).
Acute laryngotracheitis (croup) is a common viral infection which generally affects children younger than 5 years of age. Causative agents include Parainfluenza, influenza, rhinovirus etc. Stridor and steeple sign ( subglottic narrowing) are common signs.
Laryngeal diphtheria is characterised by a thick, gray green, plaque-like membranous exudate over the tonsils, pharynx, and larynx; the exudate is difficult to dislodge, and it bleeds when it is removed. 20. A 24-year-old pregnant woman on her 37th week of pregnancy has been delivered to a maternity obstetric service with complaints of weak fetal movements. Fetal heartbeats are 95/min. On vaginal examination the uterine cervix is tilted backwards, 2 cm long, external orifice allows inserting a fingertip. Biophysical profile of the fetus equals 4 points. What tactics of pregnancy management should be chosen?
21. During regular preventive gynecological examination a 30-year-old woman was detected to have dark blue punctulated ”perforations” on the vaginal portion of the uterine cervix. The doctor suspects endometriosis of the vaginal portion of the uterine cervix. What investigation method would be most informative for diagnosis confirmation?
22. A 55-year-old woman came to a gynecologist with complaints of leukorrhea and bloody discharge from the vagina after 5 years of menopause. Anamnesis states no pregnancies. Bimanual examination: the uterus and uterine appendages are without changes. During diagnostic curettage of the uterine cavity the physician scraped off enchephaloid matter. What is the most likely diagnosis in this case?
23. A 10-year-old boy is delivered into a polytrauma unit after he received a blunt trauma of the thorax, having fallen from the bicycle. Upon hospitalization his blood pressure is 110/80 mm Hg, heart rate is 96/min. Chest X-ray is noncontributive to the diagnosis. Echocardiogram shows free liquid in the pericardial cavity, in the amount of up to 100 ml. In an hour after the hospitalization the patient started to develop increasing signs of heart failure: jugular venous distention, decreased blood pressure down to 90/70 mm Hg, tachycardia up to 120/min. On auscultation muffled heart sounds. What would be the primary tactics of a physician?
24. After the celebratory feast that took place the day before, a 35-year-old man was hospitalized with complaints of marked pain within the I metatarsophalangeal articulation on the right, which developed late in the night, and impaired walking. Objectively: the metatarsophalangeal articulation is swollen, hyperemic, hot to touch, painful on movement. In blood: erythrocytes - 5, 1·1012/l, Нb- 155 g/l, leukocytes- 13, 0·109/l, ESR- 50 mm/hour, CRP- 46 mg/dl, uric acid - 720 mcmol/l. X-ray of feet articulations: osteoporosis, narrowing of interarticular spaces, numerous punched-out erosions. Make the preliminary diagnosis:
25. A woman in her early- to mid-thirties has lost her consciousness 3-5 minutes ago. On examination: the skin is pale, no pulse over the carotid arteries, no spontaneous respiration, pupils are dilated; the patient is nonresponsive, presents with atony. The patient’s condition can be determined as:
26. A 32-year-old woman complains of body weight loss despite her increased appetite, nervousness, and tremor of the extremities. Objectively: the skin is moist; the thyroid gland is diffusely enlarged, painless, soft, and mobile. Blood test: increased level of T3, T4, and thyroid-stimulating hormone (THS). What is the most likely diagnosis?
27. A 74-year-old man visited an urologist with complaints of pain above the pubis and inability to urinate for 8 hours. At home he had taken antispasmodics and had a warm bath but no improvement occurred. Objectively: the abdomen is soft and painful above the pubis; dullness of percussion sound is observed above the pubis. Murphy’s punch sign (costovertebral angle tenderness) is negative on both sides. What condition does the patient have?
28. During preventive examination a 58-yearold man on chest X-ray presents with multiple globular pale shadows 3 cm in diameter within parenchyma of the both lungs. Examination in the oncologic hospital: the primary focus is not found; transbronchial biopsy with cytologic investigation detected cells of glandular neoplasm. What tactics should the physician choose?
29. A 36-year-old man developed a disease with acute onset 6 hours ago. The patient presents with pain in the epigastric, ileocecal, and paraumbilical areas, vomiting, weakness, nausea, and body temperature of 38,5oC. Stool is liquid, profuse, frequent, retains fecal nature, foul-smelling, frothy, colored dark green. The stomach is moderately distended and painful on palpation. The patient attributes his disease to eating raw chicken eggs one day before the clinical signs of the disease appeared. What is the most likely diagnosis?
30. A 14-year-old girl came to a general practitioner with complaints of weakness, loss of appetite, headache, rapid fatigability. Her last menstruation was profuse and lasted for 14 days after previous delay of 2 months. Objectively: the skin is pale, heart rate is 90/min., BP is 110/70 mm Hg, Hb is 88 g/l. Rectal examination: the uterus and its appendages are without changes, no discharge from the genital tracts. What complication occurred in the patient?
31. A postpartum woman on the 12th day after the normal delivery complains of pain localized in her left gastrocnemius muscle. Body temperature is 37,2oC; pulse is 85/min, rhythmic; blood pressure is 128/80 mm Hg. Mammary glands are soft and painless. The uterus is behind the pubis. The left leg in the area of gastrocnemius muscle is by 3 cm larger than the right leg in the diameter. Internal organs present no pathologies. What complication can be suspected?
32. Examination of a Rh-negative pregnant woman at 32 weeks of gestation revealed a four-time rise of Rh-antibody titer within 2 last weeks; the titer is 1:64. The first two pregnancies resulted in antenatal fetal death due to hemolytic disease. What is the optimal tactics of pregnancy management?
33. During last several weeks an 11-yearold girl has been complaining of dyspnea and edema of shins and feet after physical exercise. After a long rest or sleep through the night her edemas diminish significantly. On clinical examination there are enlarged liver and rasping systolic murmur over the cardiac area. Blood and urine analyses are without changes. What is the most likely cause of the child’s edema?
34. A 60-year-old man has a diet consisting of unvaried food staples: mostly cereals, potato, pasta; few vegetables and little fats (especially animal fats). During medical examination he complains of deterioration of his twilight vision. This condition can be caused by lack of:
35. A full-term newborn (born with the body weight of 3900 g at gestational age of 39 weeks) on the first day of his life developed respiratory disturbances: dyspnea, arrhythmic respiration, cyanosis attacks. On examination there is paradoxical respiration observed and left side of the chest lags behind in the act of breathing. On auscultation the respiration is weakened in the lungs on the left. Neurologist diagnosed the patient with left-sided ErbDuchenne palsy. Complete blood count shows no changes. What is the most likely diagnosis?
36. A 12-year-old child had three attacks of acute rheumatic fever accompanied by carditis. Examination revealed the symptoms of chronic tonsillitis, mitral insufficiency, and carious teeth. What is the optimal method of secondary prophylaxis?
Explanation
Primary prophylaxis involves the treatment of streptococcal pharyngitis with antimicrobial therapy.
Secondary prophylaxis involves Continuous prophylaxis in patients with well-documented histories of rheumatic fever and in those with evidence of rheumatic heart disease. The table below gives the guideline:
|
Type
|
Duration after last attack
|
Evidence rating*
|
|
Rheumatic fever with carditis and residual heart disease (persistent valvular disease†)
|
10 years or until age 40 years (whichever is longer); lifetime prophylaxis may be needed
|
1C
|
|
Rheumatic fever with carditis but no residual heart disease (no valvular disease†)
|
10 years or until age 21 years (whichever is longer)
|
1C
|
|
Rheumatic fever without carditis
|
5 years or until age 21 years (whichever is longer)
|
1C
|
37. A 24-year-old patient had been delivered to a thoracic department with a chest injury, fracture of the IV, V, VI ribs on the right. Plan radiography showed the fluid level in the pleural cavity to be reaching the III rib on the right. Puncture contained blood clots. What is the optimal treatment tactics?
38. A 3-year-old child has been delivered to a hospital with complaints of pain in the legs, fever, loss of appetite. Objectively: pale skin and mucosa, hemorrhagic rash. Lymph nodes are enlarged, painless, dense and elastic, not matted together. Bones, joints, and abdomen are painful. The liver and spleen are enlarged. Hemogram: Hb- 88 g/l, color index - 1,3, platelets - 80 · 109/l, leukocytes - 25, 8 · 109/l, lymphoblasts - 70%, ESR- 52 mm/hour. Make the provisional diagnosis:
39. Heart X-ray of a 31-year-old man has revealed the following: with tightly filled opacified esophagus there is a marginal filling defect in its middle third on the posterior wall; the defect is 1,8x1,3 cm in size with clear oval border. Mucosal folds are retained and envelop the defect; wall peristalsis and elasticity are not affected. There are no complaints regarding the condition of the patient’s alimentary canal. Make the provisional diagnosis:
40. A patient with signs of general overexposure to cold presenting with local frostbites of fingers has been delivered into an admission room. Objectively: conscious, inert, speech is slow, the skin of the face is cold, body temperature is 34oC, heart rate is 68/min. What would be the actions of a doctor on call?
41. A 22-day-old infant developed subcutaneous red nodes from 1,0 to 1,5 cm in size on the scalp; later the nodes suppurated. Temperature increased up to 37,7oC, intoxication symptoms appeared, regional lymph nodes enlarged. Complete blood count: anemia, leukocytosis, neutrocytosis, increased ESR. What diagnosis will you make?
42. During examination of a healthy infant, the child takes a toy into his hands, turns from the back to the side; when lying on the stomach he can firmly prop himself up on his forearms; the child laughs and makes joyful exclamations. The age of the child is:
43. After significant physical exertion a 66- year-old man with deep vein thrombosis of the extremities developed shortness of breath, intense pain in the chest on the left, marked palpitations. The patient’s condition is grave, his face is cyanotic, the cervical veins are swollen, BP is 60/40 mm Hg. What investigation method would be the most advisable in this case?
44. A 32-year-old woman complains of general fatigue, low-grade fever persisting for 4 months, lumbar pain, and dysuria. Anamnesis includes frequent acute respiratory diseases, overexposure to cold, lowcalorie diet, a case of pulmonary tuberculosis in childhood. Clinical urine analysis: pH4,8, leukocyturia, hematuria. Complete blood count: leukocytosis, lymphocytosis, increased ESR. Urography concludes: dilatation of renal pelvis and calyceal system of both kidneys, foci of calcification in the projection of right kidney parenchyma. What is the most likely diagnosis?
45. An 9-year-old child was hospitalized for fever up to 39,8oC, inertness, moderate headache, vomiting. Examination revealed meningeal symptoms. Lumbar puncture was performed. The obtained fluid was characterised by increased opening pressure, was transparent, with the cell count of 450 cells per 1 mcL (mainly lymphocytes - 90%), glucose level of 3,6 mmol/l. What agent could have caused the disease in the child?
46. A 25-year-old woman has a self-detected tumor in the upper outer quadrant of her right breast. On palpation there is a painless firm mobile lump up to 2 cm in diameter, peripheral lymph nodes are without alterations. In the upper outer quadrant of the right breast ultrasound revealed a massive neoplasm with increased echogenicity sized 21x18 mm. What is the most likely diagnosis?
47. A 68-year-old man complains of inability to urinate for a day. On attempt of urinary bladder catheterization there was detected a rough stricture in the membranous portion of the urethra. What first aid tactics should be applied in this case?
48. A 3-month-old child presents with saffron-yellow coloring of the skin, sclera, and mucous membranes. The abdomen is enlarged, hepatomegaly and splenomegaly are observed. In blood there is conjugated bilirubin-induced hyperbilirubinemia. On intravenous cholangiocholecystography: opacified bile is discharged into the intestine. Transaminase activity is normal. What is the most likely diagnosis?
49. A 51-year-old woman complains of headache, trembling, paresthesiae, palpitations, increased blood pressure up to 280/160 mm Hg. The day before she experienced exhausting headache, vascular pulsation, palpitations, asphyxia, stomachache, unbearable fear of coming death. The patient paled and broke out in cold sweat. In urine there is increased content of vanillylmandelic acid. What disease causes such clinical presentation in the patient?
50. A 52-year-old patient suffers from marked dyspnea during physical exertion, non-productive cough. The patient’s condition has been persisting for 8 months. The patient has been a smoker for 30 years. In the lungs there are cellophane-type crackles auscultated on both sides. Respiration rate is 26/min., oxygen saturation of blood is 92%. On spirometry: moderate restrictive-type disturbance of external respiration. What is the most likely diagnosis
51. A 26-year-old patient with affective bipolar disorder has developed a condition manifested by mood improvement, behavioural and sexual hyperactivity, verbosity, active body language, reduced need for sleep. Which of the following drugs would be most effective in this case?
52. A 19-year-old patient complains of dyspnea on exertion. He often has bronchitis and pneumonia. Since childhood the patient presents with cardiac murmur. Auscultation revealed splitting of the II sound above the pulmonary artery, systolic murmur in the 3rd intercostal space at the left sternal border. ECG detected right bundle branch block. What is the provisional diagnosis?
53. A 30-year-old patient was in a car accident. He is unconscious, pale, has thready pulse. In the middle third of the right thigh there is an extensive laceration with ongoing profuse external arterial bleeding. What urgent actions must be taken to save the life of the patient?
54. A 25-year-old patient has been admitted to the hospital with the following problems: weakness, sweating, itching, weight loss, enlarged submandibular, cervical, axillary, inguinal lymph nodes. Objectively: hepatomegaly. Lymph node biopsy revealed giant Berezovsky-Reed-Sternberg cells, polymorphocellular granuloma composed of lymphocytes, reticular cells, neutrophils, eosinophils, fibrous tissue, and plasma cells. What is the most likely diagnosis?
55. A 22-year-old man suddenly developed extreme weakness, nausea, vomiting with traces of blood. The patient is known to suffer from peptiv ulcer disease of duodenum and hemophilia A. Objectively: heart rate - 102/min., BP- 100/60 mm Hg. Complete blood count: erythrocytes - 3, 2 · 1012/l, Hb- 98 g/l, color index - 0,92, leukocytes - 7, 4 · 109/l, platelets - 240 · 109/l, ESR- 11 mm/hour. What measure would most effectively decrease hemorrhaging in this case?
56. A 22-year-old woman complains of amenorrhea for 8 months. Anamnesis states that menarche occured at the age of 12,5. Since the age of 18 the patient has a history of irregular menstruation. The patient is nulligravida. The mammary glands are developed properly, nipples discharge drops of milk when pressed. Hormone test: prolactin level is 2 times higher than normal. CT reveals a bulky formation with diameter of 4 mm in the region of sella. What is the most likely diagnosis?
57. A 13-year-old girl complains of fatigability, frequent headaches, cardialgia. Eight years ago she had a case of pyelonephritis. Urine analyses periodically revealed leukocyturia. The child has undergone no further treatment. On examination: increased BP up to 150/100 mm Hg. Ultrasound investigation revealed significant reduction of the right kidney. What process is leading in arterial hypertension pathogenesis in this case?
58. ECG revealed the following in a 10- year-old child: sharp acceleration of the heart rate - 240/min., P wave overlaps with T wave and deforms it, moderate lengthening of PQ interval, QRS complex is without alterations. What pathology does this child have?
59. A 54-year-old patient complains of weakness, jaundice, itching skin. Disease onset was 1,5 months ago: fever up to 39oC appeared at first, with progressive jaundice developed 2 weeks later. On hospitalization jaundice was severely progressed. Liver cannot be palpated. Gallbladder is enlarged and painless. Blood bilirubin is 190 mcmol/l (accounting for direct bilirubin). Stool is acholic. What is the most likely jaundice genesis in this patient?
60. During hemotransfusion the patient developed nausea, tremor, lumbar and retrosternal pain. On examination the skin is hyperemic, later developed pallor; the patient presents with hyperhidrosis, labored respiration, pulse is 110/min., BP is 70/40 mm Hg. Urine is black colored. What complication developed in the patient?
61. A 25-year-old patient is not married and has sexual relations with several partners. During the last 3 months he noticed a small amount of mucoserous discharge from the urethra. Subjectively: periodical itching or burning pain in the urethra. Two months ago pain in the knee joint developed. Possibility of trauma or exposure to cold is denied by the patient. During the last week eye discomfort is noted - lacrimation and itching. What provisional diagnosis can be made?
62. A 19-year-old woman complains of severe pain in the axillary crease. Condition onset occurred a week ago after her swimming in a cold river and epilation. The next day a painful ”boil” appeared. The ”boil” was increasing in size every day and became a plum-sized tumor. Upon examination there are nodular conical growths joined together detected, the skin covering them is bluish-red in color. Some nodules have fistulous openings producing thick purulent mass. Body temperature is 38, 5oC, general malaise. What is the most likely diagnosis?
63. A woman complains of weight gain, chills, edema, xeroderma, somnolence, diffi- culties with focusing. Objectively: height is 165 cm; weight is 90 kg; body proportions are of female type, to- 35,8oC, heart rate - 58/min, BP- 105/60 mm Hg. Heart sounds are weakened, bradycardia is observed. Other internal organs have no alterations. Thyroid gland cannot be palpated. Milk secretion from mammary glands is observed. Hormone test revealed increased levels of thyroidstimulating hormone (TSH) and prolactin, and decreased level of thyroxine (�4). What is the cause of obesity?
64. A 37-year-old patient complains of pain in the spinal column, reduced mobility. The condition persists for 7 years. ”Sway back” is observed, there is no movement in all spinal regions. On X-ray: ”bamboo spine” is detected. What is the most likely diagnosis?
65. A 15-year-old teenager has undergone medical examination in military recruitment center. The following was revealed: interval systolic murmur at the cardiac apex, accent of the II heart sound over the pulmonary artery, tachycardia. What additional examination method will be the most informative for determining diagnosis?
66. A 64-year-old patient has been hospitalized with complaints of progressive jaundice that developed over 3 weeks without pain syndrome and is accompanied by general weakness and loss of appetite. Objectively: temperature is 36,8oC, heart rate is 78/min, abdomen is soft and painless, peritoneum irritation symptoms are not detected, palpation reveals sharply enlarged tense gallbladder. What disease can be characterised by these symptoms?
67. A 6-year-old girl came to a general practitioner with her mother. The child complains of burning pain and itching in her external genitalia. The girl was taking antibiotics the day before due to her suffering from acute bronchitis. On examination: external genitalia are swollen, hyperemic, there is white deposit accumulated in the folds. The most likely diagnosis is:
68. Anamnesis of a 30-year-old patient includes closed thoracic injury. Lately the patient has been suffering from increasing dyspnea, sensation of heaviness in the right subcostal area, and heart rate disturbances. Objectively: acrocyanosis, bulging cervical veins, ascites, edema of the lower extremities. Heart auscultation reveals muffled heart sounds, additional III heart sound is detected. Provisional diagnosis of constrictive pericarditis was made. What diagnostic technique would NOT confirm the diagnosis?
69. A 72-year-old woman suffers from diabetes mellitus type 2, concomitant diseases are stage 2 hypertension and stage 2B heart failure. She takes metformin. Hypertensic crisis had occurred the day before, after which the patient developed extreme weakness, myalgias, thirst, dry mouth, polyuria. BP is 140/95 mm Hg, heart rate is 98/min., no edemas or smell of acetone detected. What measures should be taken to prevent development of comatose state in the patient?
70. The body of a 24-year-old woman with probable signs of poisoning has been found on the street. Forensic medical examination was requested by an investigator during examination of the site and the body. According to the Criminal Procedure Code currently in force in Ukraine, forensic medical examination is required when it is necessary to determine the:
71. It is the 3rd day after the normal term labor; the infant is rooming-in with the mother and is on breastfeeding. Objectively: the mother’s general condition is satisfactory. Temperature is 36,4oC, heart rate is 80/min., BP is 120/80 mm Hg. Mammary glands are soft and painless; lactation is moderate, unrestricted milk flow. The uterus is dense, the uterine fundus is located by 3 fingers width below the navel. Lochia are sanguino-serous, moderate in volume. Assess the dynamics of uterine involution:
72. Survey radiograph of a 52-year-old worker of an agglomeration plant (28-yearlong record of service, the concentration of metal dust is 22-37 mg/m3) shows mildly pronounced interstitial fibrosis with diffused contrasting well-defined small nodular shadows. The patient has no complaints. Pulmonary function is not compromised. What is the provisional diagnosis?
73. A 53-year-old woman complains of weight loss up to 10 kg within the last 2 years, liquid foul-smelling stool two times a day that poorly washes off the toilet, periodic bouts of nausea, girdle pain in the upper abdomen. Objectively: pain in Gubergrits zone (on the right from navel) and at Mayo-Robson’s point. Biochemical blood analysis: glucose - 3,2 mmol/l, bilirubin - 16,5 mcmol/l, crude protein - 56,4 g/l. Urine diastase/amylase - 426 g/h/l. D-xylose test (oral administration of 25 g of d-xylose) after 5 hours reveals 3 g of xylose in urine. The most likely diagnosis is:
74. A multigravida at 39 weeks of gestation presenting with regular labour activity for 8 hours has been delivered to a hospital; the waters broke an hour ago. She complains of headache, seeing spots. BP is 180/100 mm Hg. Urine test results: protein - 3,3 g/l, hyaline cylinders. Fetal heart rate is 140/min, rhythmical. Vaginal examination reveals complete cervical dilatation, the fetal head is on the pelvic floor, sagittal suture is in line with obstetric conjugate, the occipital fontanel is under the pubis. What is the optimal tactics of labour management?
75. After the contact with chemicals a plant worker has suddenly developed stridor, voice hoarseness, barking cough, progressing dyspnea. Objective examination reveals acrocyanosis. What is the provisional diagnosis?
76. An 18-year-old woman complains of pain in her lower abdomen, profuse purulent discharge from the vagina, temperature rise up to 37,8oC. Anamnesis states that she had a random sexual contact the day before the signs appeared. She was diagnosed with acute bilateral adnexitis. On additional examination: leukocytes are present throughout all vision field, bacteria, diplococci with intracellular and extracellular position. What is the most likely agent in the given case?
77. A 58-year-old man complains of general weakness, loss of 10 kg of weight within 1,5 months, progressive pain in the lumbar region, increased blood pressure up to 220/160 mm Hg, low grade fever. Objectively: in the right hypochondrium deep palpation reveals a formation with uneven surface and low mobility; veins of the spermatic cord and scrotum are dilated. Blood test results: Hb- 86 g/l, ESR- 44 mm/h. Urine test results: specific gravity - 1020, protein - 0,99 g/l, RBC cover the whole field of vision, WBC- 4-6 in the field of vision. What is the provisional diagnosis?
78. A 12-year-old girl after a case of respiratory infection developed dyspnea at rest, paleness of skin. Heart rate is 110/min., BP is 90/55 mm Hg. Heart sounds are muffled. Borders of relative heart dullness: right - the parasternal line, upper - the III rib, left - 1,0 cm outwards from the midclavicular line. Make the provisional diagnosis:
Explanation
Myocarditis is an inflammation of the myocardium, it presents with a disruption in heart conduction and abnormal heart rhythms (arrhythmia). Notice that the above patient experiences an arrhythmia and the results from auscultation and percussion indicates an inflamed portion of the heart. From anamnesis, the patient has a respiratory infection; many infectious, metabolic, toxic, inflammatory processes can lead to a myocarditis- the infectious form is mostly caused by a viral infection.
Hypertrophic cardiomyopathy (HCM) is a disease in which the heart muscle becomes abnormally thick (hypertrophied). The thickened heart muscle can make it harder for the heart to pump blood.
In Somatoform Autonomic dysfunction, the symptoms are presented by the patient as if they were due to a physical disorder of a system or organ that is largely or completely under autonomic innervation and control, i.e. the cardiovascular, gastrointestinal, respiratory, and urogenital systems.
79. A 48-year-old man complains of fatigue, excessive sweating, severe skin itching, undulant fever, enlarged cervical and supraclavicular lymph nodes. Objectively: paleness of skin and mucosa, cervical lymph nodes are mobile, dense, elastic, walnut-sized, painless, not attached to the skin. Complete blood count: erythrocytes - 3, 0 · 1012/l, Hb100 g/l, leukocytes - 14 · 109/l, eosinophils - 6%, basophils - 3%, band neutrophils - 11%, segmented neutrophils - 69%, lymphocytes - 7, monocytes - 4%, platelets - 280 · 109/l, ESR 37 mm/hour. What method should be applied to verify the diagnosis?
80. A patient after a blow to the head developed general symptoms of cerebral disturbance, nausea, vomiting, focal signs - hemi-hyperreflexia S>D, hemihyperesthesia on the left, marked meningeal syndrome. Neither cranial X-ray nor computer tomography revealed any pathologies. What examination method would allow making and clarification of the diagnosis?
81. A 72-year-old man complains of lower extremity edema, sensation of heaviness in the right subcostal area, dyspnea of rest. For over 25 years he has been suffering from COPD. Objectively: orthopnea, jugular venous distention, diffuse cyanosis, acrocyanosis. Barrel chest is observed, on percussion there is vesiculotympanitic (bandbox) resonance, sharply weakened vesicular respiration on both sides, moist crepitant crackles in the lower segments of the lungs. Heart sounds are weakened, the II heart sound is accentuated over the pulmonary artery. The liver is +3 cm. What complicated the clinical course of COPD in this patient?
82. A patient complains of painless ”sores” on his penis and inguinal lymph nodes enlargement. Synthomycin emulsion that the patient have been applying to the ”sores” was ineffective. Objectively: on the inner leaf of the foreskin there are three closely situated rounded erosions, 0,5 cm in diameter, with dense infiltration that can be palpated at their bases. Make the preliminary diagnosis:
Explanation
Syphilis is a sexually transmitted disease caused by the spirochete Treponema Pallidum. It has three stages namely:
-
Primary
-
Secondary
-
Tertiary
Primary stage is characterised by the presence of Hard Chancre which are firm, painless genital ulcers/ sores. Lymphadenitis and Lymphagitis are also seen in this stage.
Herpes simplex viruses are enveloped double stranded linear viruses. HSV-1 is also known as oral herpes ( gingivostomatitis, keratoconjunctivitis etc) while HSV-2 is known as genital or neonatal herpes. The clinical presentation of genital herpes include pain, itching, dysuria, vaginal and urethral discharge, tender lymphadenopathy, appearance of herpes vesicles on the external genitalia, labia majora, labia minora, vaginal vestibule - for women and glans penis, the prepuce, the shaft of the penis, and sometimes on the scrotum, thighs, and buttocks- for men.
Candidiasis is also known as vaginal thrush or vaginal yeast infection. It is characterised by very severe vaginal itching, burning sensation while urinating, pain during sex, hyperemic vagina and a thick white vaginal discharge
83. A 1,5-month-old child on breasfeeding presents from birth with daily vomiting, irregular liquid foamy feces, and meteorism, which are resistant to antibacterial and probiotic therapy; no increase of body mass is observed. The child’s condition improved, when breastmilk was substituted with ”NAN low lactose” formula. What pathology is it?
84. A young woman suffering from seborrhea oleosa has numerous light-brown and white spots on the skin of her torso and shoulders. The spots have clear margins, branny desquamation, no itching. What provisional diagnosis can be made?
85. 10 days after birth a newborn developed sudden fever up to 38,1oC. Objectively: the skin in the region of navel, abdomen and chest is erythematous; there are multiple peasized blisters with no infiltration at the base; isolated bright red moist erosions with epidermal fragments are observed on the periphery. What is the provisional diagnosis?
86. A man came to an urologist with complains of painful urination, discharge from urethra. The patient has been suffering from this condition for a week. Objectively: hyperemic urinary meatus, edema, purulent discharge. Microscopy of smears detected gram-negative bacteria. Specify the diagnosis:
87. A patient is 28 years old. He has been suffering from mental disorder since he was 22. His current condition has changed acutely: for 3 days the patient has been refusing to leave his home. He claims that there is a ”telepathy” occurring between him and the other people, through which he receives ”thoughts of strangers” and transmits his own thoughts for everyone to hear. He is convinced that his thoughts and actions are being manipulated through this ”telepathy”. Make the preliminary diagnosis:
88. A 35-year-old woman has gained 20 kg weight within a year with the normal diet. She complains of chills, sleepiness, shortness of breath. The patient’s mother and sister are corpulent. Objectively: height - 160 cm, weight - 92 kg, BMI- 35,9. Obesity is uniform, there are no striae. The face is amimic. The skin is dry. The tongue is thickened. Heart sounds are muffled. HR- 56/min, BP- 140/100 mm Hg. The patient has been suffering from amenorrhea for 5 months, has constipations. TSH- 28 mcIU/l (norm is 0,32-5). Craniogram shows no pathology. What is the etiology of obesity?
89. A 23-year-old woman has been suffering from a mental disease since the age of 18, the course of disease has no remission periods. At a hospital the patient mostly presents with non-purposeful foolish excitation: she makes stereotypic grimaces, exposes herself, publicly masturbates with a loud laughter, repeates stereotypical abusive shouts. The patient should be prescribed:
90. A 14-year-old patient complains of alopecia foci on his scalp. The patient has been presenting with this condition for 2 weeks. Objectively: on the scalp there are several small oval foci with blurred margins. The skin in the foci is pink-red, the hairs are broken off at 4-5 mm length or at skin level. Under Wood’s lamp there are no foci of green luminescence detected. What disease is it?
91. A 38-year-old patient has been delivered by an ambulance to a surgical department with complaints of general weakness, indisposition, black stool. On examination the patient is pale, there are dotted hemorrhages on the skin of his torso and extremities. On digital investigation there are black feces on the glove. Blood test: Hb- 108 g/l, thrombocytopenia. Anamnesis states that similar condition was observed 1 year ago. Make the diagnosis:
92. A 35-year-old patient developed an epileptic attack with tonoclonic spasms that lasted for 3 minutes. After the attack the patient fell asleep but in 5 minutes the second attack occurred. The first step of emergency aid would be to:
93. A 14-year-old girl has been delivered to a gynecological department with complaints of profuse blood discharge from her genital tract for 2 weeks. Anamnesis: menstruation since 13, irregular, painful, profuse; the last one was 2 months ago. Objectively: pale skin and mucosa, BP- 100/60 mm Hg, Hb- 108 g/l. The abdomen is soft and painless on palpation. Rectal examination revealed no pathologies of reproductive organs. What condition is it?
94. An infant cries during urination, the foreskin swells and urine is excreted in drops. What approach to treatment should be chosen?
95. A 20-year-old patient complains of pain in the left lumbar region, arterial pressure rise up to 160/110 mm Hg. US revealed that the structure and size of the right kidney were within age norms, there were signs of the 3rd degree hydronephrotic transformation of the left kidney. Doppler examination revealed an additional artery running to the lower pole of the kidney. Excretory urogram shows a narrowing in the region of ureteropelvic junction. Specify the treatment tactics:
96. A 49-year-old patient consulted a doctor about difficult swallowing, voice hoarseness, weight loss. These symptoms have been gradually progressing for the last 3 months. Objectively: the patient is exhausted, there are enlarged supraclavicular lymph nodes. Esophagoscopy revealed no esophageal pathology. Which of the following investigations is the most appropriate in this case?
97. A 15-year-old girl complains of dizziness and sensation of lack of air that she develops in emotionally straining situations. Relief occurs after she takes corvalol. Objectively: hyperhidrosis and marble-like pattern of the skin of her palms and feet. Clinical and instrumental examination revealed no organic alterations of the central nervous, cardiovascular, and respiratory systems. What provisional diagnosis can be made?
98. A patient with chronic pancreatitis complains of diarrhea occurring up to 5 times per day (no blood traces), loss of body weight, abdominal distention, dryness of skin, loss of hair, thirst, bleeding gums, convulsions. Complete blood count: leukocytes - 5, 8 · 109/l; Hb- 86 g/l; ESR- 15 mm/g; Blood protein test: protein - 48 g/l; albumins - 28 g/l. What indicators of coprological analysis would accompany this syndrom?
99. A 35-year-old patient complains of heartburn, gasseous and sour eructation, burning constricting pain behind the sternum and along the esophagus, developing when bowing the torso to the front. No previous examination; the patient takes almagel at his own discretion, after which he notes improvement of his general state. Make the provisional diagnosis:
Explanation
Heartburn, gaseous and sour eructation, burning constricting pain behind the sternum and along the esophagus are signs of a reflux disease, these symptoms are observed due to the backflow of gastric acidic content into the esophagus. One main reason is the inefficient constriction/closing of the lower esophageal sphincter or an overproduction of gastric acid. Note that the patient takes Amagel, an antacid which helps in neutralizing the acidic content.
ulcers occur when the acid in the digestive tract eats away at the lining of the stomach or small intestine, creating irritated or raw spots that can become painful open, bleeding sores. Some of the symptoms of peptic ulcer disease include burning stomach pain, feeling full quickly, bloating, intolerance to fatty foods, heartburn, and nausea.
100. The left hand of a newborn is extended in all its joints, stretched along the torso, and pronated in the forearm. Active movements of the shoulder joint are retained. The hand is flattened, atrophied, cold to touch, hangs passively. Grasping and Babkin’s reflexes are absent at the affected side. Hemogram indicators are normal. Make the most likely diagnosis:
101. A 34-year-old man is being treated for schizophrenia exacerbation in a psychiatric unit. Objectively: the patient remains in bed, is sluggishly mobile, unresponsive, does not react to questions. His position is unvaried, hypomimic, snout reflex and Dupre’s symptom are present, muscles exhibit waxy flexibility. He has been remaining in this state for approximately a week. Feeding is parenteral. Determine the neuromotor disturbance:
Explanation
Schizophrenia is a mental disorder characterised by disturbances in thought and verbal behaviour,perception, motor behaviour and relationship to the external world. The different clinical types include; Paranoid, disorganised/ hebephrenic, Catatonic, residual or latent, undifferentiated schizophrenia. Catatonic schizophrenia is further divided into an excited form and stuporous form. The patient above is said to have a catatonic stupor; this state is characterised by inability to speak, rigidity, maintenance of weird postures; maintained for a long period of time metc. Snout reflex involves puckering or protrusion of the lips with percussion.
In depressive stupor, the patient will mostly be in a sleepy state, motionless, quiet and have no appetite.
102. A 43-year-old man has undergone a surgery for osteomyelitis of the left thigh. On the 6th day the patient’s condition was complicated with sepsis. Despite complex therapy of sepsis on the 9th day the patient persistently presents with temperature up to 40oC, heart rate is 110/min., respiration rate is 23/min., BP is 100/60 mm Hg. Blood test: leukocytes - 16 · 109/l, band neutrophils - 16%. What phase of clinical course is it?
103. A 23-year-old woman presents with diabetes mellitus type 1. She complains of weakness, headache, nausea, and vomiting. Objectively: temperature is 37,6oC, heart rate is 98/min., BP is 95/65 mm Hg, respiration rate is 32/min., loud. Smell of acetone is detected, heart sounds are muffled, pulse is rhythmic. The stomach is sensitive in the epigastrium. Costovertebral angle tenderness (Murphy’s punch sign) is present. Blood glucose is 28,5 mmol/l; blood leukocytes - 16, 5 · 109/l. In urine: acetone ++, leukocytes - 25-40 in the vision field. Blood pH is 7,1. What correction method would be the most advisable?
104. A 57-year-old woman complains of a sensation of esophageal compression, palpitations, difficult breathing when eating solid food, occasional vomiting with a full mouth, ”wet pillow” sign at night for the last 6 months. Objectively: body tempearture - 39oC, height - 168 cm, weight - 72 kg, Ps76/min, BP- 120/80 mm Hg. X-ray study revealed considerable dilation of esophagus and its constriction in the cardial part. What pathology is the most likely to have caused dysphagia in this patient?
105. A 47-year-old man is employed at the weaving workshop, has 15-year-long record of service at this factory; his work conditions are associated with high-frequency and high-intensity noise. During periodical examination he was diagnosed with occupational deafness. What are the grounds for making such a diagnosis?
106. A 37-year-old woman complains of acute pain in the genital area, swelling of the labia, pain when walking. Objectively: body temperature is 38,7oC, Ps- 98/min. In the interior of the right labia there is a dense, painful tumor-like formation 5,0x4,5 cm in size, the skin and mucous membrane of genitals are hyperemic, there is profuse foul-smelling discharge. What is the most likely diagnosis?
107. A woman undergoing in-patient treatment for viral hepatitis type B developed headache, nausea, recurrent vomiting, memory lapses, flapping tremor of her hands, rapid pulse. Sweet smell from the mouth is detected. Body temperature is 37,6oC, heart rate is 89/min. What complication developed in the patient?
Explanation
Acute liver failure is a state of hepatic cells dysfunction, caused by unknown earlier liver disease, resulting in general intoxication, coagulation violations, neurological and mental disorders. Its etiology is usually connected with: viral hepatitis (hepatitis B virus, hepatitis A virus), poisonings (mushrooms, dichloroethane, phosphorus, carbon tetrachloride, arsenic), eclampsia, burn disease, anaesthetic gas, antibiotics, sulfanilamides, massive bacterial pneumonia, cirrhosis, hepatic tumours and metastasis.
Advanced liver failure manifests as coma due to the effects of accumulated metabolites on the brain. The patient in question presents with viral hepatitis B ( the probable cause of the liver failure) and a list of other symptoms which indicate neurological and intoxication disorder.
108. A 42-year-old man was delivered to a surgical in-patient department with complaints of icteric skin, pain in the right subcostal area. Biochemical blood analysis: total bilirubin - 140 mcmol/l, direct bilirubin - 112 mcmol/l. On US: choledoch duct - 1,4 cm, a concrement is detected in the distal area. Gallbladder is 40 cm, no concrements. What treatment tactics should be chosen?
109. 4 weeks after myocardial infarction a 56- year-old patient developed acute heart pain, marked dyspnea. Objectively: the patient’s condition is extremely grave, there is marked cyanosis of face, swelling and throbbing of neck veins, peripheral pulse is absent, the carotid artery pulse is rhythmic, 130/min., BP is 60/20 mm Hg. Auscultation of the heart reveals extremely muffled sounds, percussion reveals heart border extension in both directions. What is the optimal treatment tactics for this patient?
110. A 44-year-old patient with postinfarction cardiosclerosis presents with frequent heart rate disorders and lower extremity edema. Objectively: Ps- 95/min., irregular, 10-12 extrasystoles per minute. BP- 135/90 mm Hg. The 1st heart sound at the apex is weakened. Pulmonary respiration is rough. The liver is enlarged +2 cm. ECG: irregular sinus rhythm, heart rate - 95/min, frequent polytopic ventricular extrasystoles.What antiarrhythmic drug is advisable in this case for treatment and prevention of extrasystole?
111. A 60 year-old woman has been suffering from weakness, dizziness, and fatigue over the last year. Recently she has also developed dyspnea, paresthesia. Objectively: the skin and mucous membranes are pale and slightly icteric. The tongue is smooth due to the loss of lingual papillae. Liver and spleen are located at the costal margin. Blood count: Hb- 70 g/l, RBC- 1, 7·1012/l, color index - 1,2, macrocytes. Administer the patient a pathogenetically justified drug:
112. After excessive consumption of fatty food a 60-year-old woman suddenly developed pain in her right subcostal area, nausea, bile vomiting, sharp bitter taste in her mouth. In 2 days she developed jaundice, her urine darkened. Objectively: sclera and skin are icteric, the abdomen is distended, the liver is enlarged by 3 cm, soft and painful on palpation, Ortner’s, Murphy’s, Kehr’s, Zakharyin’s, Mayo-Robson’s signs are positive. What diagnostic technique should be used in the first place?
113. A 42-year-old woman working at a poultry farm complains of dyspnea, thoracic pain on the left, increased body temperature up to 38- 39oC in the evening, and cough. The patient suffers from essential hypertension. Objectively: vesicular respiration in the lungs, vesicular resonance without alterations. X-ray of both lungs reveals numerous small lowintensity foci, 2-3 mm in size, located in a row along the blood vessels. ESR- 32 mm/hour. What is the most likely diagnosis?
114. A 65-year-old patient has been suffering from liver cirrhosis associated with hepatitis C virus for 7 years. During the last 3 weeks the patient developed severe edema of the lower extremities, the abdomen is significantly distended with fluid. Ultrasound: signs of liver cirrhosis, portal hypertension, lymph nodes are in the area of hepatic portal. Concentration of α-fetoprotein in blood serum is 285 ng/ml. What complication could have developed in this case?
115. A 46-year-old woman has been hospitalized with open fracture of the left thigh in its middle third. She underwent the surgery - fixation with extraosseous osteosynthesis plates. On the 4th day after the surgery she developed pain in the wound, body temperature rose over 39oC. What measures should be taken in this case?
116. A multigravida on the 38th week of her pregnancy complains of increased BP up to 140/90 mm Hg, edema of the shins for 2 weeks. In the last month she gained 3,5 kg of weight. Urine analysis: protein - 0,033 g/l. Make the diagnosis:
ExplanationPreeclampsia, a pregnancy-specific condition in which hypertension develops after 20 weeks of gestation in a previously normotensive woman. It is characterized by hemoconcentration, hypertension, and proteinuria. The following are the differences between a mild and severe Preeclampsia:
|
MIld Preeclampsia
|
Severe Preeclampsia
|
|
BP reading of 140/90 mm Hg twice, 4-6 hr apart
Proteinuria of 0.3 g/L in a 24 hr specimen or >0.1 g/L in a random day-time specimen on two or more occasions 6 hr apart
Dependent edema, some puffiness of eyes, face, fingers; pulmonary edema absent
Output matching intake, ≥30 ml/hr or <650 ml/24 hr
|
Rise to >160/110 mm Hg on two separate occasions 4-6 hr apart with pregnant woman on bed rest
Proteinuria of >0.5 g/L in 24 hr
Generalized edema, noticeable puffiness; eyes, face, fingers; pulmonary edema possibly present
<20 ml/hr or <400 ml to 500 ml/24 hr
|
117. A 28-year-old woman complains of increased intervals between menstruations, up to 2 months, and hirsutism. Gynecological examination revealed the following: ovaries are enlarged, painless, and dense; no alterations of the uterus. US of the lesser pelvis: ovaries are 4-5 cm in diameter, with numerous enlarged follicles on the periphery. X-ray of the skull base: sellar region is widened. What is the most likely diagnosis?
118. Posture of an 11-year-old boy was determined during preventive examination. The child presents with curled forward rounded shoulders, the head is bowed forward, the thorax is flattened, the stomach is bulging. In the vertebral column there are deepened cervical and lumbar flexures. What posture does the child have?
119. A patient has the second and third degree burns of the 15% of the body surface. On the 20th day after the trauma the patient presents with sharp increase of body temperature, general weakness, rapid vesicular respiration; facial features are sharpened, BP is 90/50 mm Hg, heart rate is 112/min. What complication is it?
120. A 30-year-old woman complains of amenorrhea that lasts for 2 years after she has given birth, loss of hair and body weight. The labor was complicated with hemorrhage caused by uterine hypotonia. Objectively the patient is of asthenic type, her external genitalia are hypoplastic, the uterine body is small in size and painless. No uterine appendages can be detected. What is the most likely diagnosis?
121. On laboratory investigation of a pork
sample there is 1 dead trichinella detected
in 24 sections. This meat should be:
122. Examination of a 43-year-old man objectively revealed pallor of skin and mucous membranes, loss of tongue papillae, transverse striation of fingernails, cracks in the mouth corners, tachycardia. Blood test results: Hb- 90 g/l, anisocytosis, poikilocytosis. The most likely causative factor of this condition is the inadequate intake of:
123. A 52-year-old woman presents with affected mucosa in the mouth angles where fissures, erosions, and ulcers develop; vertical fissures appear on the lips during their closing (cheilosis); there are tongue alterations (glossitis), angular stomatitis, seborrheic dermatitis around the mouth and wings of the nose, and pericorneal injection. The listed symptoms are characteristic of:
124. Two days ago a woman fell from the height of 1,5 m. She complains of severe thoracic pain on the left and dyspnea. Chest X-ray reveals hydropneumothorax on the left with fluid level at the 7th rib and the lung collapsed by 1/3. The 6th-7th ribs are fractured along the scapular line. Serohemorrhagic fluid was obtained during thoracic puncture. What treatment tactics should be chosen?
125. A patient complains of suppuration from the ear and impaired hearing of the left ear, which have been observed for the past 6 years. The patient had periodical headaches, general indisposition, fever. Objectively: otoscopy of the external auditory meatus revealed mucopurulent odorless substance. The eardrum is of normal color, with central perforation. What is the most likely diagnosis?
126. In 2 hours after a traffic accident a 28-yearold man in grave condition was delivered to a hospital. The patient complains of abdominal pain. He received a blow to the abdomen with the steering wheel. Objective examination revealed the following: the abdomen does not participate in respiration, is tense and acutely painful on palpation; the abdominal muscles are defensively tense, peritoneal irritation signs are positive, hepatic dullness is absent. BP is 90/60 mm Hg, heart rate is 120/min. What further treatment tactics should be chosen?
127. From urine of a 14-year-old boy with the exacerbation of secondary obstructive pyelonephritis Pseudomonas aeruginosa was isolated with a titer of 1000000 microbes per 1 ml. What antibiotic is the most advisable in this case?
128. A 20-year-old woman on the 10th day after her discharge from the maternity ward developed fever up to 39oC and pain in her left mammary gland. On examination the mammary gland is enlarged, in its upper outer quadrant there is a hyperemic area. In this area a dense spot with blurred margins can be palpated. The patient presents with lactostasis and no fluctuation. Lymph nodes in the right axillary crease are enlarged and painful. Specify the correct diagnosis:
129. A 3-year-old girl is being treated at a resuscitation unit with diagnosis ”acute kidney failure, oligoanuric stage”. ECG: high T wave, extended QRS complex, displacement of S-T interval downwards below the isoline. What electrolyte imbalance is it?
130. Mother of an 8-year-old girl complains that the child is too short and has excessive body weight. Objectively: obesity with fat deposits on the torso and face (round moonlike face), acne, striae on the thighs and lower abdomen, hirsutism. What hormone can cause such symptoms, when in excess?
131. A 9-year-old girl complains of fever up to 37,5oC, headache, inertness, weakness, loss of appetite, stomachache, and frequent painful urination. Provisional diagnosis of acute pyelonephritis is made. Clinical urine analysis: specific gravity - 1018, no protein, leukocytes - 10-15 in the vision field. What investigation method can verify the diagnosis of urinary system infection?
132. During assessment of work conditions at the mercury thermometer manufacture, content of mercury vapors in the air of working area is revealed to exceed maximum concentration limit. Specify the main way of mercury penetration into the body:
133. During health assessment of car drivers and police officers on point duty, the physicians detected carboxyhemoglobin in the blood of the patients, weakened reflex responses, disturbed activity of a number of enzymes. Revealed professional health disorders are most likely to be associated with the effect of:
134. On the 3rd day of life a newborn, who had suffered birth asphyxia, developed hemorrhage from the umbilical wound. Laboratory analysis reveals hypocoagulation, thrombocytopenia, and hypothrombinemia. What is the cause of such clinical developments?
135. A 46-year-old woman came to a maternity clinic with complaints of moderate blood discharge from the vagina, which developed after the menstruation delay of 1,5 months. On vaginal examination: the cervix is clean; the uterus is not enlarged, mobile, painless; appendages without changes. Make the diagnosis:
136. An infant is 2,5 months old. The onset of the disease was gradual, the child had normal body temperature but presented with slight cough. Within a week the cough intensified, especially at night; on the 12th day the child developed cough fits occurring up to 20 times per day and followed by vomiting. There was one instance of respiratory arrest. Make the diagnosis:
137. Vaginal examination reveals the head of the fetus, which fills the posterior surface of symphysis pubis and hollow of the sacrum. The lower edge of symphysis pubis, ischiadic spines, and sacrococcygeal joint can be palpated. Where in the lesser pelvis is the fetal head situated?
138. A man works in casting of nonferrous metals and alloys for 12 years. In the air of working area there was registered high content of heavy metals, carbon monoxide, and nitrogen. During periodic health examination the patient presents with asthenovegetative syndrome, sharp pains in the stomach, constipations, pain in the hepatic area. In urine: aminolevulinic acid and coproporphyrin are detected. In blood: reticulocytosis, low hemoglobin level. Such intoxication is caused by:
139. A 30-year-old multigravida has been in labour for 18 hours. 2 hours ago the pushing stage began. Fetal heart rate is clear, rhythmic, 136/min. Vaginal examination reveals complete cervical dilatation, the fetal head in the pelvic outlet plane. Sagittal suture is in line with obstetric conjugate, the occipital fontanel is near the pubis. The patient has been diagnosed with primary uterine inertia. What is the further tactics of labour management?
140. A patient, who had eaten canned mushrooms (honey agaric) three days ago, developed vision impairment (diplopia, mydriasis), speech disorder, disturbed swallowing. What type of food poisoning occurred in the patient?
141. An infant is 3 weeks old. Since birth there has been observed periodical vomiting within a few minutes after feeding. The amount of vomitive masses does not exceed the volume of previous feeding. The infant has age-appropriate body weight. What is the most likely cause of this symptom?
142. A newborn with gestational age of 31 weeks presents with hypotonia and depressed consciousness. Hematocrit is 35%, general cerebrospinal fluid analysis shows increased content of erythrocytes and protein, and low glucose. These data correspond with the clinical presentation of:
143. A 50-year-old patient was delivered to a hospital with complaints of blood traces in urine. Urination is painless and undisturbed. Macrohematuria had been observed for 3 days. Objectively: kidneys cannot be palpated, suprapubic area is without alterations, external genitalia are non-pathologic. On rectal investigation: prostate is not enlarged, painless, has normal structure. Cystoscopy revealed no alterations. What is the most likely diagnosis?
144. A man complains of constant dull pain in the perineum and suprapubic area, weak flow of urine, frequent difficult painful urination, nocturia. The patient has been suffering from this condition for several months, during which urination was becoming increasingly difficult, and pain in the perineum has developed. On rectal examination: the prostate is enlarged (mainly its right lobe), dense, asymmetrical, central fissure is smoothed out, the right lobe is of stony density, painless, tuberous. What disease is it?
145. A boy was born at 32 weeks of gestation. 2 hours after the birth he developed respiratory distress (RD). The RD severity assessed by Silverman score was 5. The respiratory disorders progressed, respiratory failure could not be eliminated by Martin-Bouyer CPAP (continuous positive airway pressure). X-ray of lungs shows reticular and nodular pattern, air bronchogram. What is the most likely cause of respiratory distress syndrome?
146. An 8-year-old child with a 3-year-long history of diabetes was hospitalized in hyperglycemic coma. Specify the initial dose of insulin to be administered:
ExplanationInitial intravenous administration of 10 to 14 units of short-acting insulin has to be prescribed for the patient during the first hour. Continuous intravenous infusion of insulin in a dose 0,1 unit/kg/hour in 0,9 % sodium chloride infusion has to be given after that.
147. A 17-year-old young man complains of general weakness, trismus, twitching of the muscles in his left shin. 7 days ago he pierced his foot with a nail. Objectively: at the sole of the foot there is a wound, 0,3х0,2 mm in size, with small amount of serous-purulent discharge, the skin around the wound is hyperemic. What is the most likely diagnosis?
148. A patient with trauma of the lower third of the forearm volar surface caused by a glass shard came to a first-aid center. Objectively: flexion of the IV and V fingers is impaired, sensitivity of the inner dorsal and palmar surfaces of the hand and IV finger is decreased. What nerve is damaged?
149. A 58-year-old patient complains of pain in the lower left extremity, which aggravates during walking, sensation of cold and numbness in the both feet. The patient has been suffering from this condition for 6 years. Objectively: the skin is pale and dry, with hyperkeratosis. On the left shin hair is scarce, ”furrow” symptom of inflamed inguinal lymph nodes is positive. Pulse cannot be detected over the pedal and popliteal arteries and is weakened over the femoral artery. In the right limb popliteal artery pulsation is retained. What is the most likely diagnosis?
150. A 9-month-old child presents with fever, cough, dyspnea. The symptoms appeared 5 days ago after a contact with a person with URTI. Objectively: the child is in grave condition. Temperature is 38oC, cyanosis of nasolabial triangle is present. RR- 54/min, nasal flaring during breathing is observed. There was percussion dullness on the right below the scapula angle and tympanic sound over the other areas of lungs. Auscultation revealed bilateral fine moist crackles predominating on the right. What is the most likely diagnosis?
151. The mother of a 3-month-old child came to a family doctor with complaints of her child being physically underdeveloped and suffering from cough attacks and dyspnea. Anamnesis: the child is the result of the second full-term pregnancy with the risk of miscarriage (the first child died of pulmonary pathology at the age of 4 months, according to the mother). Body mass at birth is 2500 g. Cough attacks were observed from the fi- rst days of life, twice the child was treated for bronchitis. Considering the severity of the child’s condition the doctor made the referral for hospitalization. What diagnosis was most likely stated in the referral?
Explanation
Cystic fibrosis (Mucoviscidosis) is an inherited disorder that results in a buildup of thick and sticky mucus in the lungs, airways, and other organs. Excess mucus in the lungs can lead to coughing, breathing problems, scarring (fibrosis), and an increased risk of lung infections. There is no cure, but treatments can improve both the length and quality of life for people with the disease.
Cystic fibrosis is caused by mutations in the gene that encodes the cystic fibrosis transmembrane conductance regulator (CFTR). This protein functions as a channel across the membrane of cells that produce mucus, sweat, saliva, tears, and digestive enzymes.
From the history, the mother already had a child that died of a pulmonary pathology (inherited disorder) and the recurrent infections (bronchitis) all points to Cystic Fibrosis.
All other options given are not hereditary.
152. A 46-year-old man notes swollen legs, weakness, sensation of fullness and heaviness in the right subcostal area; it is the first occurrence of these signs in the patient. The patient has 20-year-long history of rheumatoid arthritis. The liver and spleen are enlarged and dense. Blood creatinine - 0,23 mmol/l, proteinemia - 68 g/l, cholesterol - 4,2 mmol/l, urine specific gravity - 1012, proteinuria - 3,3 g/l, isolated wax-like cylinders, leached erythrocytes in the vision field, leukocytes - 5-6 in the vision field. What is the most likely complication?
153. A 23-year-old man had taken 1 g of aspirin to treat acute respiratory infection. After that he developed an asthmatic fit with labored expiration that was arrested by introduction of aminophylline. The patient has no medical history of allergies. The patient has undergone two surgeries for nasal polyposis in the past. What is the most likely diagnosis?
154. A 45-year-old patient complains of pain in the epigastric region, left subcostal area, abdominal distension, diarrhea, loss of weight. He has been suffering from this condition for 5 years. Objectively: the tongue is moist with white coating near the root; deep palpation of abdomen reveals slight pain in the epigastric region and Мауо-Robson’s point. Liver is painless and protrudes by 1 cm from the costal arch. Spleen cannot be palpated. What disease can be primarily suspected?
155. For three years a 31-year-old woman has been complaining of pain and swelling of her radiocarpal and metacarpophalangeal articulations, their reduced mobility in the morning, which persisted up to 1,5 hours. Two weeks ago she developed pain, swelling, and reddening of her knee joints, her body temperature increased up to 37,5oC. The treatment was belated. Examination of the internal organs revealed no pathologic alterations. Diagnosis of rheumatoid arthritis was made. What alterations are the most likely to be visible on the arthrogram?
Explanation
The question stem clearly states that the patient has been diagnosed with Rheumatoid Arthritis.
So basically, we need to differentiate Rheumatoid Arthritis and Osteoarthritis so that we can arrive at the correct answer specific for Rheumatoid Arthritis.
RA: autoimmune which erodes articulated cartilage and bone. The inflammatory cells and cytokines then induce pannus (proliferative granulation tissue) formation, deep usurations.
Associated with pain, swelling and morning stiffness, lasting >1hr and the pain improves with use.
Joint findings: joint space narrowing; erosions; juxtaarticular osteopenia; soft tissue swelling; subchondral cysts
Involves Metacarpophalangeal joints; wrist; proximal interphalangeal joints. Does not affect distal interphalangeal joints on the hands
OA: mechanical wear and tear - it’s a degenerative joint disease.
Associated with Pain in weight bearing joints after use (i.e. at the end of the day), and the pain improves with rest.
Joint findings: joint space narrowing; osteophytes (bone spurs); subchondral sclerosis and cysts.
Involves distal interphalangeal joints on the hands (heberden nodes) and Proximal interphalangeal joints (Bouchard nodes); does not affect Metacarpophalangeal joints.
So let’s answer the question:
From the question stem - Radiocarpal (wrist joints); metacarpophalangeal joints were affected with morning stiffness lasting >1.5hrs
These are clearly signs and symptoms of Rheumatoid Arthritis...
From the options it is clear that the only option talking about RA is joint space narrowing; usuration
The other options are talking about Osteoarthritis.
156. A 58-year-old woman complains of spontaneous bruises, weakness, bleeding gums, dizziness. Objectively: the mucous membranes and skin are pale with numerous hemorrhages of various time of origin. Lymph nodes are not enlarged. Ps- 100/min, BP110/70 mm Hg. There are no alterations of internal organs. Blood test results: RBC3, 0 · 1012/l, Нb- 92 g/l, color index - 0,9, anisocytosis, poikilocytosis, WBC- 10 · 109/l, eosinophils - 2%, stab neutrophils - 12%, segmented neutrophils - 68%, lymphocytes - 11%, monocytes - 7%, ESR- 12 mm/h. What laboratory test should be performed additionally to make the diagnosis?
157. After tonsillectomy a woman with systemic lupus erythematosus, who has been taking prednisolone for a year, developed acute weakness, nausea, vomiting, pain in the right iliac area, watery stool up to 5 times per day. Ps- 96/min., BP- 80/50 mm Hg. What preventive therapy should have been administered prior to the surgery?
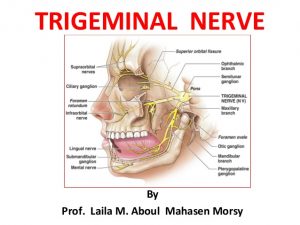
158. A 45-year-old woman complains of paroxysmal intolerable facial pain on the left with attacks that last for 1-2 minutes. Attacks are provoked by chewing. The disease onset was two month ago after overexposure to cold. Objectively: pain at the exit points of the trigeminal nerve on the left. Touching near the wing of nose on the left induces new pain attack with tonic spasm of the facial muscles. What is the most likely diagnosis among those listed?
Explanation
Trigeminal Neuralgia is a condition which produces repetitive,unilateral, shooting/shot-like pain in the areas innervated by the trigeminal nerve ( the face). It is triggered by chewing, talking or touching certain parts of the face. Typically lasts for seconds to minutes but episodes often increase in intensity and frequency over time.
Recall that the trigeminal nerve, CV is a mixed type of nerve, has 3 major branches;
V1 (ophthalmic), V2( Maxillar), V3(mandibular). This nerve is responsible for mastication, facial sensation, somatosensation from anterior ⅔ of the tongue, and innervates the tensor tympani.
159. A 28-year-old man complains of skin rash and itching on the both of his hands. The condition persists for 1,5 years. The exacerbation of his condition he ascribes to the occupational contact with formaldehyde resins. Objectively: lesion foci are symmetrically localized on both hands. Against the background of erythema with blurred margins there are papulae, vesicles, erosions, crusts, and scales. What is the most likely pathology?
160. A 10-year-old boy with symptoms of arthritis and myocarditis was delivered into a hospital. Based on clinical examination the preliminary diagnosis of juvenile rheumatoid arthritis was made. What symptom is the most contributive for the diagnostics of this disease?
161. A 25-year-old patient was delivered to an infectious diseases unit on the 3rd day of illness with complaints of headache, pain in the lumbar spine and gastrocnemius muscles, high fever, chills. Objectively: condition is of moderate severity. Scleras are icteric. Pharynx is hyperemic. Tongue is dry with dry brown coating. Abdomen is distended. Liver is enlarged by 2 cm. Spleen is not enlarged. Palpation of muscles, especially gastrocnemius muscles, is painful. Urine is dark in color. Feces are normal in color. What is the most likely diagnosis?
162. A 28-year-old woman complains of skin hemorrhages after minor traumas and spontaneous appearance of hemorrhages on the front of her torso and extremities. On examination: the skin is variegated (old and new hemorrhages), bleeding gums. Blood platelets - 20·109/l; in the bone marrow there is increased number of megakaryocytes and no platelet production. Treatment with steroid hormones was effective. What disease is it?
163. A 74-year-old patient was delivered into admission room with clinical presentations of acute deep vein thrombosis of the shin. What symptom is the most typical of this pathology?
164. A 45-year-old man complains of cough fits and tickling in his nasopharynx. He had been staying for 10 days in the polluted area created by the Chornobyl nuclear power plant accident. Rhinoscopy shows signs of severe nasopharynx irritation. What radionuclide is the cause of this irritation?
165. A 20-year-old patient complains of severe headache, double vision, weakness, fever, irritability. Objectively: body temperature is 38,1oC, the patient is reluctant to contact, sensitive to stimuli. There are ptosis of the left eyelid, exotropia, anisocoria S>D, pronounced meningeal syndrome. On lumbar puncture the cerebrospinal fluid flowed out under a pressure of 300 mm Hg, the fluid is clear, slightly opalescent. 24 hours later there appeared fibrin film. Protein - 1,4 g/l, lymphocytes - 600/3 per mm3, sugar - 0,3 mmol/l. What is the provisional diagnosis?
166. A 37-year-old worker during a fire ended up in the area of high CO concentration. He was delivered to a hospital in unconscious state. Objectively: the skin of his face and hands is crimson. Respiration rate is 20/min. ECG: alterations specific for hypoxic myocardium. Hourly diuresis is 40 ml. Blood test: erythrocytes - 4, 5 · 1012/l, Нb- 136 g/l, color index - 0,89, ESR- 3 mm/hour, carboxyhemoglobin - 5%. What criterion allows determining the severity of the patient’s condition?
167. After a case of purulent otitis a 1-year-old boy has developed pain in the upper third of the left thigh, body temperature up to 39oC. Objectively: swelling of the thigh in its upper third and smoothed out inguinal fold. The limb is in semiflexed position. Active and passive movements are impossible due to severe pain. What diagnosis is the most likely?
168. A patient with suspected pheochromocytoma has normal blood pressure in the periods between the atacks and a tendency towards tachycardia. Urine test revealed no pathologies. It was decided to use a provocative test with histamine. What medication should be prepared to provide emergency care in case of positive test result?
169. A 42-year-old woman complains of severe pulsing headache in the frontoparietal area, vertigo, palpitations. She has been suffering from hypertension for 3 years. Significant increase of BP occurs 2-3 times per month and lasts for 3-8 hours. The left ventricle is enlarged, heart sounds are clear, heart rate - 105/min., BP- 225/115 mm Hg. ECG: signs of left ventricular hypertrophy. What drug would be the most effective for termination of cerebral crisis attack?
170. A woman came to a doctor with complaints of increased body temperature up to 37,8oC and moderately sore throat for the last 3 days. Objectively: mandibular lymph nodes are enlarged up to 3 cm. Palatine tonsils are hypertrophied, with gray coating that spreads to the uvula and anterior pillars of the fauces. What is the most likely diagnosis?
171. A primigravida at the term of 20 weeks complains of pain in her lower abdomen, smearing blood-streaked discharge from the genital tracts. Uterine tone is increased, fetus is mobile. On vaginal examination: the uterus is enlarged according to the term, uterine cervix is shortened to 0,5 cm, external cervical orifice is open by 2 cm. What is the most likely diagnosis?
172. A 65-year-old man was diagnosed with B12-deficient anemia and the treatment was prescribed. A week later control blood test was performed. What would be the early indicator of the therapy effectiveness?
173. A 35-year-old woman complains of heart pain (”aching and drilling”) occurring mainly in the morning in autumn and spring and irradiating to the neck, back and abdomen; rapid heartbeat; low vitality. Occurrence of this condition is not associated with physical activity. In the evening, the patient’s condition improves. Study of somatic and neurological status and ECG reveal no pathology. What pathology is most likely to have caused these clinical presentations?
174. On the 4th day after recovery from a cold a patient was hospitalized with complaints of solitary spittings of mucoid sputum. On the 2nd day there was a single discharge of about 250 ml of purulent blood-streaked sputum. Objectively: the patient’s condition is moderately severe. Respiratory rate - 28-30/min., Ps- 96/min., BP- 110/70 mm Hg. Respiration over the left lung is vesicular, over the right lung - weakened. There are various moist crackles over the lower lobe and amphoric breath sounds near the angle of scapula. What is the most likely diagnosis?
175. A 65-year-old woman on abdominal palpation presents with a tumor in the umbilical region and above it; the tumor is 13x8 cm in size, moderately painful, non-mobile, pulsing. On auscultation systolic murmur can be observed. What is the most likely diagnosis?
176. For a week a 42-year-old patient has been suffering from fever attacks followed by high temperature, which occur each 48 hours. Body temperature raises up to 40oC and decreases in 3-4 hours with excessive sweating. The patient presents with loss of appetite and general fatigue. The skin is pale and sallow. The liver and spleen are enlarged and dense on palpation. What method of diagnosis verifi- cation would be most efficient?
177. A 28-year-old patient is a drug addict. He has been sick for a year, when noticed general weakness, increased sweating, and weight loss. He often had cases of respiratory diseases. Within the last 2 days he demonstrates intermittent fever with profuse night sweating, increased general weakness, developed diarrhea with mucus and blood admixtures. On examination: polylymphadenopathy, herpetic rashes in the oral cavity; on abdominal palpation: the liver and spleen are enlarged. What is the most likely diagnosis?
178. A 40-year-old patient has acute onset of disease caused by overexposure to cold. Temperature has increased up to 39oC. Foul-smelling sputum is expectorated during coughig. Various moist crackles can be auscultated above the 3rd segment on the right. Blood test: leukocytes - 15, 0 · 109/l, stab neutrophils - 12%, ESR- 52 mm/hour. On Xray: in the 3rd segment on the right there is a focus of shadow 3 cm in diameter, low density, with fuzzy smooth margins and a clearing in its center. What disease is most likely in the given case?
179. A 48-year-old patient was found to have diffuse enlargement of the thyroid gland, exophthalmia, weight loss of 4 kg in 2 months, sweating. Objectively: HR- 105/min, BP140/70 mm Hg. Defecation act is normal. What kind of therapy is recommended in this case?
180. A 26-year-old woman is suspected to suffer from systemic lupus erythematosus due to systemic lesions of skin, vessels, joints, serous tunics, and heart that developed after photosensitization. The following is detected: LE cells, antibodies to native DNA, isolated anti-centromere antibodies, rheumatoid factor is 1:100, Wassermann reaction is positive, circulating immune complex is 120 units. What immunological indicators are considered to be specific to this disease?
181. A 39-year-old man complains of morning headaches, appetite loss, nausea, morning vomiting, periodic nasal hemorrhages. The patient had a case of acute glomerulonephritis at the age of 15. Examination revealed rise of arterial pressure up to 220/130 mm Hg, skin hemorrhages on his arms and legs, pallor of skin and mucous membranes. What biochemical parameter is the most important for making diagnosis in this case?
182. A worker of a glass-blowing workshop complains of headache, irritability, visual impairment - he sees everything as if through a ”net”. Objectively: hyperemic sclera, thickened cornea, decreased opacity of pupils, visual acuity is 0,8 in the left eye, 0,7 in the right eye. The worker uses no means of personal protection. What is the most likely diagnosis?
183. An infant has been born at the 41st week of gestation. The pregnancy was complicated with severe gestosis of the second semester. The weight of the baby is 2400 g, the height is 50 cm. Objectively: the skin is flabby, the layer of subcutaneous fat is thin, hypomyotonia is observed, neonatal reflexes are weak. The internal organs are without pathologic alterations. This newborn can be assessed as a:
184. A patient suffering from infiltrative pulmonary tuberculosis was prescribed streptomycin, rifampicin, isoniazid, pyrazinamide, vitamin C. One month after the beginning of the treatment the patient started complaining of reduced hearing and tinnitus. What drug has such a side effect?
Explanation
Tuberculosis is a disease caused by an acid fast bacteria, Mycobacterium tuberculosis. Streptomycin, Rifampicin, Isoniazid, pyrazinamide and ethambutol are very active drugs chosen for its treatment. The following are lists of side effects associated with these drugs:
Streptomycin- vestibular and auditory ( ototoxicity) dysfunction, non oliguric renal failure
Rifampicin- red/ orange discoloration of body fluids e.g. tears, urine; flu-like symptoms, hepatitis, diarrhea, thrombocytopenia.
Isoniazid- hepatitis, peripheral neuropathies
Pyrazinamide- asymptomatic hyperuricemia, joint pain, rash
Ethambutol- retrobulbar optic neuritis
185. A 9-year-old boy has been suffering from multiple bronchiectasis since he was 3 years old. Exacerbations occur frequently (3- 4 times a year), after conservative therapy there are short remission periods. The disease progresses, the child is physically underdeveloped, presents with pale skin, acrocyanosis, deformed nail plates in the shape of ”clock-face”. Bronchography reveals saccular bronchiectases in the lower lobe of the right lung. What further treatment tactics should be chosen?
186. Caries morbidity rate is 89% among residents of a community. It is determined that fluorine content in water is 0,1 mg/l. What preventive measures should be taken?
187. A patient received flame burns of both hands. On the dorsal and palmar surface of the hands there are blisters filled with serous fluid. The wrist joint region is hyperemic. The forearms were not injured. What is the provisional diagnosis?
Explanation
rule of “nines” – area of different areas of the body is proportional: anterior surface of the trunk – 18 %, posterior – 18 %, lower limb – 18 %, external genitals – 1 %)
" rule of “palm”. It is used if burns are limited and located on different areas of the body. According to the rule of palm takes 1 % of the skin surface.
Division of the burns on superficial (I, II, III A st.) and deep (III B-IV st.)
I stage – hyperemia of the skin
II stage – separation of epidermis with formation of bullas
III A stage – necrosis of superficial layers of the skin with saving of bulbs hair, sweat glands and sebaceous glands.
III B stage – necrosis of all the derma
IV stage – necrosis of the skin and underlying tissues.
Notice that the patient has suffered burns affecting just the surface with the appearance of blisters ( bulla)
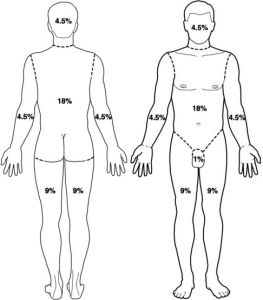
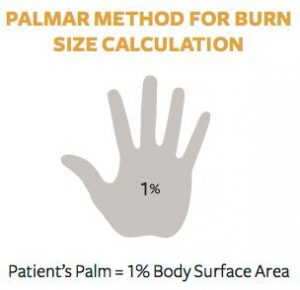
188. During the periodic medical examination an assembly fitter (works on soldering details) didn’t report any health problems. Closer examination revealed signs of asthenicvegetative syndrome. Blood included red blood cells with basophilic aggregations and a somewhat higher number of reticulocytes, urine had a high concentration of delta-aminolevulinic acid. The complex of symptoms indicates the initial stage of chronic intoxication with:
189. A 29-year-old woman came to a gynecologist with complaints of irritability, tearfulness, headache, nausea, occasional vomiting, pain in the heart area, tachycardia attacks, memory impairment, meteorism. These signs appear 6 days before menstruation and disappear the day before menstruation or during its first 2 days. On vaginal examination: the uterus and uterine appendages are without alterations. What diagnosis is the most likely?
ExplanationPremenstrual syndrome is a wide variety of signs and symptoms that affects a woman’s emotion, physical health, and behavior during certain days of the menstrual cycle, generally just before her menses. Symptoms start five to 11 days before menstruation and typically go away once menstruation begins. Signs include abdominal pain and bloating, vomiting ,meteorism, change in sleep patterns, emotional instability etc.
Also called Stein- Leventhal syndrome, Ovarian sclerocytosis is the process of ovarian regeneration, accompanied by the formation of small cystic formations up to 1 cm in size. It usually occurs in patients with polycystic ovarian syndrome. Key findings include; infertility, male pattern hair distribution, weight loss, hormonal disbalance, bilateral enlargement of the ovaries, violation of menstrual cycle etc.
190. Examination of a group of persons living on the same territory revealed the following common symptoms: dark-yellow pigmentation of the tooth enamel, diffuse osteoporosis of bone apparatus, ossification of ligaments and joints, functional disorders of the central nervous system. This condition may be caused by the excessive concentration of the following microelement in food or drinking water:
191. A 52-year-old patient, who has been suffering from angina pectoris, for 2 weeks has increasingly frequent pain attacks in the area behind his sternum and his need for nitroglycerine has increased. Objectively: the condition is of moderate severity. The skin is pale. Heart sounds are weakened, rhythmic. Heart rate is 84/min. ECG shows no signs of focal myocardial injury. What is the most likely diagnosis?
192. 5 weeks after hypothermia a 22-yearold patient developed fever, weakness, muscle pain, inability to move independently. Objectively: tenderness, induration of shoulder and shin muscles, restricted active movements, erythema on the anterior surface of the chest. There is a periorbital edema with heliotropic erythema. Gottron’s sign is present. What investigation is required for the diagnosis verification?
193. A 37-year-old woman complains of headaches, nausea, vomiting, spasms. The onset of the disease occurred the day before due to her overexposure to cold. Objectively: fever up to 40oC; somnolence; rigid neck; Kernig’s symptom is positive on the both sides; general hyperesthesia. Blood test: leucocytosis, increased ESR. Cerebrospinal fluid is turbid, yellow-tinted. What changes of the cerebrospinal fluid are most likely?
194. A 44-year-old patient complains of diffi- cult urination, sensation of incomplete urinary bladder emptying. Sonographic examination of the urinary bladder near the urethra entrance revealed an oval welldefined hyperechogenic formation 2x3 cm large that was changing its position during the examination. What conclusion can be made?
195. 4 days after a patient received a gunshot wound to the soft tissues of middle third of the thigh, his condition suddenly began deteriorating. There are complaints of bursting pain in the wound; pain has been increasing during the last 12 hours. Edema of skin and hypodermic tissue quickly grows. Body temperature is 38,2oC, heart rate is 102/min. The wound edges gape, are dull in color; the muscles, viable as of day before, now protrude into the wound, look boiled, are dull in color, have dirty-gray coating, and fall apart when held with forceps. What infection has developed in the wound?
196. A 35-year-old patient has been suffering from an illness for 3 days. 5 days ago he returned from a trip to Africa. The onset of disease was accompanied by fever up to 40oC, chills, acute headache, myalgia. In the axillary region the lymph node enlarged up to 3x6 cm can be palpated. The lymph node is dense, intensely painful, slightly mobile, without clear margins; the skin over the node is hyperenic and tight. Tachycardia is present. Make the preliminary diagnosis:
197. A parturient woman complains of pain in her mammary gland. In the painful area there is an infiltration 3x4 cm in size with softened center. Body temperature is 38,5oC. What is the most likely diagnosis?
198. After a 5-day-long celebration of his daughter’s wedding a 65-year-old patient ”saw” in his yard many cats, chickens, and rats. He tried to chase them away, but was scared off when the animals started to scold him and tried to harm him. Make the diagnosis:
199. An 8-year-old boy developed a temperature of 37, 5oC two days after his recovery from the case of URTI. He complains of suffocation, heart pain. Objectively: the skin is pale, tachycardia, the I heart sound is weakened, short systolyc murmur in the 4th intercostal area near the left edge of the breastbone. What heart disorder such clincal presentation is characteristic of?
200. A 28-year-old woman has been delivered to a hospital with acute pain in the lower abdomen. There was a brief syncope. The delay of menstruation is 2 months. Objectively: the patient has pale skin, BP- 90/50 mm Hg, Ps- 110/min. Lower abdomen is extremely painful. Vaginal examination reveals uterus enlargement. Promtov’s sign (pain during bimanual gynecological examination) is positive. Right uterine appendages are enlarged and very painful. Posterior vault hangs over. What is the most likely diagnosis?